Multicenter retrospective study of cefmetazole and flomoxef for treatment of extended-spectrum-β-lactamase-producing Escherichia coli bacteremia
- PMID: 26100708
- PMCID: PMC4538479
- DOI: 10.1128/AAC.00701-15
Multicenter retrospective study of cefmetazole and flomoxef for treatment of extended-spectrum-β-lactamase-producing Escherichia coli bacteremia
Abstract
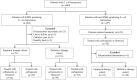
The efficacy of cefmetazole and flomoxef (CF) for the treatment of patients with extended-spectrum β-lactamase-producing Escherichia coli (ESBL-EC) bacteremia (ESBL-CF group) was compared with that of carbapenem treatment for ESBL-EC patients (ESBL-carbapenem group) and with that of CF treatment in patients with non-ESBL-EC bacteremia (non-ESBL-CF group). Adult patients treated for E. coli bacteremia in four hospitals were retrospectively evaluated. The 30-day mortality rates in patients belonging to the ESBL-CF, ESBL-carbapenem, and non-ESBL-CF groups were compared as 2 (empirical and definitive therapy) cohorts. The adjusted hazard ratios (aHRs) for mortality were calculated using Cox regression models with weighting according to the inverse probability of propensity scores for receiving CF or carbapenem treatment. The empirical-therapy cohort included 104 patients (ESBL-CF, 26; ESBL-carbapenem, 45; non-ESBL-CF, 33), and the definitive-therapy cohort included 133 patients (ESBL-CF, 59; ESBL-carbapenem, 54; non-ESBL-CF, 20). The crude 30-day mortality rates for patients in the ESBL-CF, ESBL-carbapenem, and non-ESBL-CF groups were, respectively, 7.7%, 8.9%, and 3.0% in the empirical-therapy cohort and 5.1%, 9.3%, and 5.0% in the definitve-therapy cohort. In patients without hematological malignancy and neutropenia, CF treatment for ESBL-EC patients was not associated with mortality compared with carbapenem treatment (empirical-therapy cohort: aHR, 0.87; 95% confidence interval [CI], 0.11 to 6.52; definitive therapy cohort: aHR, 1.04; CI, 0.24 to 4.49). CF therapy may represent an effective alternative to carbapenem treatment for patients with ESBL-EC bacteremia for empirical and definitive therapy in adult patients who do not have hematological malignancy and neutropenia.
Copyright © 2015, American Society for Microbiology. All Rights Reserved.
Figures
Similar articles
-
Carbapenem therapy is associated with improved survival compared with piperacillin-tazobactam for patients with extended-spectrum β-lactamase bacteremia.Clin Infect Dis. 2015 May 1;60(9):1319-25. doi: 10.1093/cid/civ003. Epub 2015 Jan 13. Clin Infect Dis. 2015. PMID: 25586681 Free PMC article.
-
Bloodstream infections due to extended-spectrum beta-lactamase-producing Escherichia coli and Klebsiella pneumoniae: risk factors for mortality and treatment outcome, with special emphasis on antimicrobial therapy.Antimicrob Agents Chemother. 2004 Dec;48(12):4574-81. doi: 10.1128/AAC.48.12.4574-4581.2004. Antimicrob Agents Chemother. 2004. PMID: 15561828 Free PMC article.
-
[Evaluation of Antibiotics for the Treatment of Bacteremia Due to Extended-spectrum β-Lactamase-producing Escherichia coli].Yakugaku Zasshi. 2015;135(6):829-33. doi: 10.1248/yakushi.14-00253. Yakugaku Zasshi. 2015. PMID: 26028418 Japanese.
-
Comparative effectiveness of flomoxef versus carbapenems in the treatment of bacteraemia due to extended-spectrum β-lactamase-producing Escherichia coli or Klebsiella pneumoniae with emphasis on minimum inhibitory concentration of flomoxef: a retrospective study.Int J Antimicrob Agents. 2015 Dec;46(6):610-5. doi: 10.1016/j.ijantimicag.2015.07.020. Epub 2015 Sep 7. Int J Antimicrob Agents. 2015. PMID: 26387064
-
Beta-lactam/beta-lactamase inhibitors versus carbapenem for bloodstream infections due to extended-spectrum beta-lactamase-producing Enterobacteriaceae: systematic review and meta-analysis.Int J Antimicrob Agents. 2018 Nov;52(5):554-570. doi: 10.1016/j.ijantimicag.2018.07.021. Epub 2018 Aug 3. Int J Antimicrob Agents. 2018. PMID: 30081138
Cited by
-
Effect of rapid cefpodoxime disk screening for early detection of third-generation cephalosporin resistance in Escherichia coli and Klebsiella pneumoniae bacteremia.J Pharm Health Care Sci. 2023 Dec 1;9(1):43. doi: 10.1186/s40780-023-00313-x. J Pharm Health Care Sci. 2023. PMID: 38037095 Free PMC article.
-
Change in the Antimicrobial Resistance Profile of Extended-Spectrum β-Lactamase-Producing Escherichia coli.J Clin Med Res. 2019 Sep;11(9):635-641. doi: 10.14740/jocmr3928. Epub 2019 Sep 1. J Clin Med Res. 2019. PMID: 31523337 Free PMC article.
-
Diagnosis and treatment of community-acquired pneumonia in adults: 2016 clinical practice guidelines by the Chinese Thoracic Society, Chinese Medical Association.Clin Respir J. 2018 Apr;12(4):1320-1360. doi: 10.1111/crj.12674. Epub 2017 Sep 26. Clin Respir J. 2018. PMID: 28756639 Free PMC article. Review.
-
Is Cefoxitin a Carbapenem Sparing Agent in the Management of Urinary Tract Infections Caused by ESBL Producing Enterobacterales?Hosp Pharm. 2022 Aug;57(4):568-574. doi: 10.1177/00185787211066460. Epub 2021 Dec 30. Hosp Pharm. 2022. PMID: 35898247 Free PMC article.
-
Cefaclor as a first-line treatment for acute uncomplicated cystitis: a retrospective single-center study.BMC Urol. 2020 Apr 6;20(1):38. doi: 10.1186/s12894-020-00605-6. BMC Urol. 2020. PMID: 32252747 Free PMC article.
References
-
- Rottier WC, Ammerlaan HS, Bonten MJ. 2012. Effects of confounders and intermediates on the association of bacteraemia caused by extended-spectrum β-lactamase-producing Enterobacteriaceae and patient outcome: a meta-analysis. J Antimicrob Chemother 67:1311–1320. doi:10.1093/jac/dks065. - DOI - PubMed
-
- Vardakas KZ, Tansarli GS, Rafailidis PI, Falagas ME. 2012. Carbapenems versus alternative antibiotics for the treatment of bacteraemia due to Enterobacteriaceae producing extended-spectrum β-lactamases: a systematic review and meta-analysis. J Antimicrob Chemother 67:2793–2803. doi:10.1093/jac/dks301. - DOI - PubMed