Blunt splenic injury and severe brain injury: a decision analysis and implications for care
- PMID: 26100770
- PMCID: PMC4467501
- DOI: 10.1503/cjs.015814
Blunt splenic injury and severe brain injury: a decision analysis and implications for care
Abstract
Background: The initial nonoperative management (NOM) of blunt splenic injuries in hemodynamically stable patients is common. In soldiers who experience blunt splenic injuries with concomitant severe brain injury while on deployment, however, NOM may put the injured soldier at risk for secondary brain injury from prolonged hypotension.
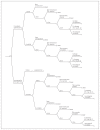
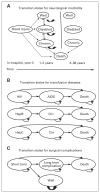
Methods: We conducted a decision analysis using a Markov process to evaluate 2 strategies for managing hemodynamically stable patients with blunt splenic injuries and severe brain injury--immediate splenectomy and NOM--in the setting of a field hospital with surgical capability but no angiography capabilities. We considered the base case of a 40-year-old man with a life expectancy of 78 years who experienced blunt trauma resulting in a severe traumatic brain injury and an isolated splenic injury with an estimated failure rate of NOM of 19.6%. The primary outcome measured was life expectancy. We assumed that failure of NOM would occur in the setting of a prolonged casualty evacuation, where surgical capability was not present.
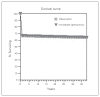
Results: Immediate splenectomy was the slightly more effective strategy, resulting in a very modest increase in overall survival compared with NOM. Immediate splenectomy yielded a survival benefit of only 0.4 years over NOM.
Conclusion: In terms of overall survival, we would not recommend splenectomy unless the estimated failure rate of NOM exceeded 20%, which corresponds to an American Association for the Surgery of Trauma grade III splenic injury. For military patients for whom angiography may not be available at the field hospital and who require prolonged evacuation, immediate splenectomy should be considered for grade III-V injuries in the presence of severe brain injury.
Contexte: La gestion non chirurgicale (GNC) initiale des traumatismes spléniques fermés chez les patients hémodynamiquement stables est fréquente. Toutefois, dans les cas de traumatismes spléniques fermés accompagnés de graves lésions cérébrales concomitantes durant leur déploiement, la GNC peut exposer les soldats blessés à un risque de lésion cérébrale secondaire par suite d’une hypotension prolongée.
Méthodes: Nous avons appliqué un modèle de Markov à l’analyse décisionnelle pour évaluer 2 stratégies de prise en charge des patients hémodynamiquement stables porteurs de traumatismes spléniques fermés et de graves lésions cérébrales, soit la splénectomie immédiate et la GNC, dans le contexte d’un hôpital de campagne doté d’installations chirurgicales mais non d’installations angiographiques. Nous avons étudié le scénario de référence d’un homme de 40 ans ayant une espérance de vie de 78 ans, victime d’un traumatisme fermé entraînant une lésion cérébrale grave et un traumatisme splénique isolé, avec un taux estimé d’échec de la GNC de 19,6 %. Le principal paramètre mesuré était l’espérance de vie. Nous avons présumé que l’échec de la GNC surviendrait dans le contexte d’une évacuation prolongée des blessés en l’absence d’installations chirurgicales.
Résultants: La splénectomie immédiate s’est révélée être une stratégie légèrement plus efficace, entraînant une augmentation très modeste de la survie globale comparativement à la GNC. La splénectomie immédiate a produit un avantage de 0,4 an seulement au plan de la survie par rapport à la GNC.
Conclusion: Au plan de la survie globale, nous ne recommanderions pas la splénectomie, à moins que le taux d’échec estimé de la GNC n’excède 20 %, ce qui correspond à un traumatisme splénique de grade III selon l’American Association for the Surgery of Trauma. Pour le personnel militaire blessé chez qui il est impossible de procéder à une angiographie dans un hôpital de campagne, et qui requiert une évacuation prolongée, il faut envisager une splénectomie immédiate pour les traumatisme de grade III V en présence de graves lésions cérébrales.
Figures

Similar articles
-
Nonoperative Management Is as Effective as Immediate Splenectomy for Adult Patients with High-Grade Blunt Splenic Injury.J Am Coll Surg. 2016 Aug;223(2):249-58. doi: 10.1016/j.jamcollsurg.2016.03.043. Epub 2016 Apr 23. J Am Coll Surg. 2016. PMID: 27112125
-
Blunt assault is associated with failure of nonoperative management of the spleen independent of organ injury grade and despite lower overall injury severity.J Trauma. 2009 Mar;66(3):630-5. doi: 10.1097/TA.0b013e3181991aed. J Trauma. 2009. PMID: 19276730
-
Proximal splenic angioembolization does not improve outcomes in treating blunt splenic injuries compared with splenectomy: a cohort analysis.J Trauma. 2008 Dec;65(6):1346-51; discussion 1351-3. doi: 10.1097/TA.0b013e31818c29ea. J Trauma. 2008. PMID: 19077625
-
Blunt splenic injury.Curr Opin Crit Care. 2010 Dec;16(6):575-81. doi: 10.1097/MCC.0b013e3283402f3a. Curr Opin Crit Care. 2010. PMID: 20885317 Review.
-
Nonoperative management of blunt splenic injury in adults: there is (still) a long way to go. The results of the Bologna-Maggiore Hospital trauma center experience and development of a clinical algorithm.Surg Today. 2015 Oct;45(10):1210-7. doi: 10.1007/s00595-014-1084-0. Epub 2014 Dec 5. Surg Today. 2015. PMID: 25476466 Review.
Cited by
-
Management of blunt splenic injury in a UK major trauma centre and predicting the failure of non-operative management: a retrospective, cross-sectional study.Eur J Trauma Emerg Surg. 2018 Jun;44(3):397-406. doi: 10.1007/s00068-017-0807-5. Epub 2017 Jun 9. Eur J Trauma Emerg Surg. 2018. PMID: 28600670
-
Laparoscopic splenectomy as a definitive management option for high-grade traumatic splenic injury when non operative management is not feasible or failed: a 5-year experience from a level one trauma center with minimally invasive surgery expertise.Updates Surg. 2021 Aug;73(4):1515-1531. doi: 10.1007/s13304-021-01045-z. Epub 2021 Apr 10. Updates Surg. 2021. PMID: 33837949 Free PMC article.
-
Angioembolization in patients with blunt splenic trauma in Germany -guidelines vs. Reality a retrospective registry-based cohort study of the TraumaRegister DGU®.Eur J Trauma Emerg Surg. 2024 Oct;50(5):2451-2462. doi: 10.1007/s00068-024-02640-6. Epub 2024 Sep 16. Eur J Trauma Emerg Surg. 2024. PMID: 39283492 Free PMC article.
-
Splenic trauma: WSES classification and guidelines for adult and pediatric patients.World J Emerg Surg. 2017 Aug 18;12:40. doi: 10.1186/s13017-017-0151-4. eCollection 2017. World J Emerg Surg. 2017. PMID: 28828034 Free PMC article. Review.
-
Concurrent Surgery of Craniectomy and Splenectomy as Initial Treatment in Severe Traumatic Head Injury: A Case Report.Korean J Neurotrauma. 2017 Oct;13(2):141-143. doi: 10.13004/kjnt.2017.13.2.141. Epub 2017 Oct 31. Korean J Neurotrauma. 2017. PMID: 29201849 Free PMC article.
References
-
- Esposito TJ, Gamelli RL. Injury to the spleen. In: Mattox KL, Feliciano DL, Moore EE, editors. Trauma. 4th Edition. New York: McGraw-Hill; 2000.
-
- Ellison EC, Fabri PJ. Complications of splenectomy. Surg Clin North Am. 1983;63:1313–30. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
