How much might a society spend on life-saving interventions at different ages while remaining cost-effective? A case study in a country with detailed data
- PMID: 26155199
- PMCID: PMC4493819
- DOI: 10.1186/s12963-015-0052-2
How much might a society spend on life-saving interventions at different ages while remaining cost-effective? A case study in a country with detailed data
Abstract
Objective: We aimed to estimate the maximum intervention cost (EMIC) a society could invest in a life-saving intervention at different ages while remaining cost-effective according to a user-specified cost-effectiveness threshold.
Methods: New Zealand (NZ) was used as a case study, and a health system perspective was taken. Data from NZ life tables and morbidity data from a burden of disease study were used to estimate health-adjusted life-years (HALYs) gained by a life-saving intervention. Health system costs were estimated from a national database of all publicly funded health events (hospitalizations, outpatient events, pharmaceuticals, etc.). For illustrative purposes we followed the WHO-CHOICE approach and used a cost-effectiveness threshold of the gross domestic product (GDP) per capita (NZ$45,000 or US$30,000 per HALY). We then calculated EMICs for an "ideal" life-saving intervention that fully returned survivors to the same average morbidity, mortality, and cost trajectories as the rest of their cohort.
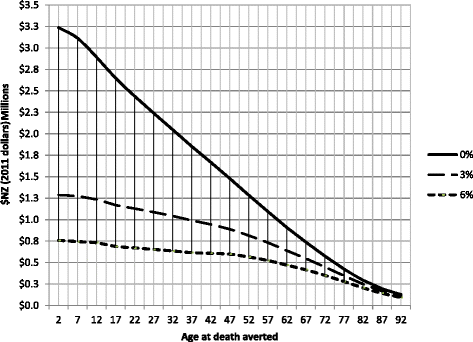
Findings: The EMIC of the "ideal" life-saving intervention varied markedly by age: NZ$1.3 million (US$880,000) for an intervention to save the life of a child, NZ$0.8 million (US$540,000) for a 50-year-old, and NZ$0.235 million (US$158,000) for an 80-year-old. These results were predictably very sensitive to the choice of discount rate and to the selected cost-effectiveness threshold. Using WHO data, we produced an online calculator to allow the performance of similar calculations for all other countries.
Conclusions: We present an approach to estimating maximal cost-effective investment in life-saving health interventions, under various assumptions. Our online calculator allows this approach to be applied in other countries. Policymakers could use these estimates as a rapid screening tool to determine if more detailed cost-effectiveness analyses of potential life-saving interventions might be worthwhile or which proposed life-saving interventions are very unlikely to benefit from such additional research.
Keywords: Age; Cost-effective; Cost-effectiveness threshold; Health system costs; Health-adjusted life expectancy (HALE); Health-adjusted life-years (HALYs); Morbidity; Quality-adjusted life-years (QALYs).
Figures
Similar articles
-
Impact of low-dose CT screening for lung cancer on ethnic health inequities in New Zealand: a cost-effectiveness analysis.BMJ Open. 2020 Sep 24;10(9):e037145. doi: 10.1136/bmjopen-2020-037145. BMJ Open. 2020. PMID: 32973060 Free PMC article.
-
Colorectal Cancer Screening: How Health Gains and Cost-Effectiveness Vary by Ethnic Group, the Impact on Health Inequalities, and the Optimal Age Range to Screen.Cancer Epidemiol Biomarkers Prev. 2017 Sep;26(9):1391-1400. doi: 10.1158/1055-9965.EPI-17-0150. Epub 2017 Jun 16. Cancer Epidemiol Biomarkers Prev. 2017. PMID: 28626068
-
Home safety assessment and modification to reduce injurious falls in community-dwelling older adults: cost-utility and equity analysis.Inj Prev. 2016 Dec;22(6):420-426. doi: 10.1136/injuryprev-2016-041999. Epub 2016 May 24. Inj Prev. 2016. PMID: 27222247
-
Comparing health gains, costs and cost-effectiveness of 100s of interventions in Australia and New Zealand: an online interactive league table.Popul Health Metr. 2022 Jul 27;20(1):17. doi: 10.1186/s12963-022-00294-3. Popul Health Metr. 2022. PMID: 35897104 Free PMC article. Review.
-
Quality-adjusted life-years lack quality in pediatric care: a critical review of published cost-utility studies in child health.Pediatrics. 2005 May;115(5):e600-14. doi: 10.1542/peds.2004-2127. Pediatrics. 2005. PMID: 15867026 Review.
Cited by
-
Prioritization of intervention domains to prevent cardiovascular disease: a country-level case study using global burden of disease and local data.Popul Health Metr. 2023 Jan 26;21(1):1. doi: 10.1186/s12963-023-00301-1. Popul Health Metr. 2023. PMID: 36703150 Free PMC article.
-
Health Gain, Cost Impacts, and Cost-Effectiveness of a Mass Media Campaign to Promote Smartphone Apps for Physical Activity: Modeling Study.JMIR Mhealth Uhealth. 2020 Jun 11;8(6):e18014. doi: 10.2196/18014. JMIR Mhealth Uhealth. 2020. PMID: 32525493 Free PMC article.
-
Development and Validation of a Predictive Model to Identify Patients With an Ascending Thoracic Aortic Aneurysm.J Am Heart Assoc. 2021 Nov 16;10(22):e022102. doi: 10.1161/JAHA.121.022102. Epub 2021 Nov 6. J Am Heart Assoc. 2021. PMID: 34743563 Free PMC article.
-
Long-term cost-effectiveness analysis of rugby fans in training-New Zealand: a body weight reduction programme for males.BMJ Open. 2024 Jul 23;14(7):e073740. doi: 10.1136/bmjopen-2023-073740. BMJ Open. 2024. PMID: 39043600 Free PMC article.
-
The international trial of nasal oxygen therapy after cardiac surgery (NOTACS) in patients at high risk of postoperative pulmonary complications: Economic evaluation protocol and analysis plan.PLoS One. 2025 Jan 28;20(1):e0311861. doi: 10.1371/journal.pone.0311861. eCollection 2025. PLoS One. 2025. PMID: 39874369 Free PMC article.
References
-
- The World Bank. Health expenditure, total (% of GDP). The World Bank. 2014. http://data.worldbank.org/indicator/SH.XPD.TOTL.ZS. Accessed 18 June 2014.
-
- Ministry of Health . Health Expenditure Trends in New Zealand 2000–2010. Wellington: Ministry of Health; 2012.
-
- Bell M, Blick G, Parkyn O, Rodway P, Vowles P. Challenges and Choices: Modelling New Zealand's Long-term Fiscal Position. The Treasury Wellington. 2010. http://www.treasury.govt.nz/publications/research-policy/wp/2010/10-01. Accessed 18 June 2014.
-
- Morton J. Measure the quality of healthcare spending. New Zeal Med J. 2008;121(1284):92–94. - PubMed
-
- Appleby J, Harrison A. Spending on Health Care United Kingdom: King's Fund. 2006.
LinkOut - more resources
Full Text Sources
Other Literature Sources