Isoflurane favorably modulates guanosine triphosphate cyclohydrolase-1 and endothelial nitric oxide synthase during myocardial ischemia and reperfusion injury in rats
- PMID: 26192027
- PMCID: PMC4543441
- DOI: 10.1097/ALN.0000000000000778
Isoflurane favorably modulates guanosine triphosphate cyclohydrolase-1 and endothelial nitric oxide synthase during myocardial ischemia and reperfusion injury in rats
Abstract
Background: The authors investigated the hypothesis that isoflurane modulates nitric oxide (NO) synthesis and protection against myocardial infarction through time-dependent changes in expression of key NO regulatory proteins, guanosine triphosphate cyclohydrolase (GTPCH)-1, the rate-limiting enzyme involved in the biosynthesis of tetrahydrobiopterin and endothelial nitric oxide synthase (eNOS).
Methods: Myocardial infarct size, NO production (ozone-mediated chemiluminescence), GTPCH-1, and eNOS expression (real-time reverse transcriptase polymerase chain reaction and western blotting) were measured in male Wistar rats with or without anesthetic preconditioning (APC; 1.0 minimum alveolar concentration isoflurane for 30 min) and in the presence or absence of an inhibitor of GTPCH-1, 2,4-diamino-6-hydroxypyrimidine.
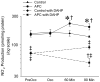
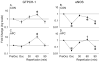
Results: NO2 production (158 ± 16 and 150 ± 13 pmol/mg protein at baseline in control and APC groups, respectively) was significantly (P < 0.05) increased 1.5 ± 0.1 and 1.4 ± 0.1 fold by APC (n = 4) at 60 and 90 min of reperfusion, respectively, concomitantly, with increased expression of GTPCH-1 (1.3 ± 0.3 fold; n = 5) and eNOS (1.3 ± 0.2 fold; n = 5). In contrast, total NO (NO2 and NO3) was decreased after reperfusion in control experiments. Myocardial infarct size was decreased (43 ± 2% of the area at risk for infarction; n = 6) by APC compared with control experiments (57 ± 1%; n = 6). 2, 4-Diamino-6-hydroxypyrimidine decreased total NO production at baseline (221 ± 25 and 175 ± 31 pmol/mg protein at baseline in control and APC groups, respectively), abolished isoflurane-induced increases in NO at reperfusion, and prevented reductions of myocardial infarct size by APC (60 ± 2%; n = 6).
Conclusion: APC favorably modulated a NO biosynthetic pathway by up-regulating GTPCH-1 and eNOS, and this action contributed to protection of myocardium against ischemia and reperfusion injury.
Conflict of interest statement
Figures

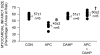


References
-
- Amour J, Brzezinska AK, Weihrauch D, Billstrom AR, Zielonka J, Krolikowski JG, Bienengraeber MW, Warltier DC, Pratt PF, Jr, Kersten JR. Role of heat shock protein 90 and endothelial nitric oxide synthase during early anesthetic and ischemic preconditioning. Anesthesiology. 2009;110:317–25. - PMC - PubMed
-
- Amour J, Brzezinska AK, Jager Z, Sullivan C, Weihrauch D, Du J, Vladic N, Shi Y, Warltier DC, Pratt PF, Jr, Kersten JR. Hyperglycemia adversely modulates endothelial nitric oxide synthase during anesthetic preconditioning through tetrahydrobiopterin- and heat shock protein 90-mediated mechanisms. Anesthesiology. 2010;112:576–85. - PMC - PubMed
-
- Michel T. NO way to relax: The complexities of coupling nitric oxide synthase pathways in the heart. Circulation. 2010;121:484–6. - PubMed
-
- Chiari PC, Bienengraeber MW, Weihrauch D, Krolikowski JG, Kersten JR, Warltier DC, Pagel PS. Role of endothelial nitric oxide synthase as a trigger and mediator of isoflurane-induced delayed preconditioning in rabbit myocardium. Anesthesiology. 2005;103:74–83. - PubMed
-
- Ludwig LM, Patel HH, Gross GJ, Kersten JR, Pagel PS, Warltier DC. Morphine enhances pharmacological preconditioning by isoflurane: Role of mitochondrial K(ATP) channels and opioid receptors. Anesthesiology. 2003;98:705–11. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources

