Current trends in the surgical management and treatment of adult glioblastoma
- PMID: 26207249
- PMCID: PMC4481356
- DOI: 10.3978/j.issn.2305-5839.2015.05.10
Current trends in the surgical management and treatment of adult glioblastoma
Abstract
This manuscript discusses the current surgical management of glioblastoma. This paper highlights the common pathophysiology attributes of glioblastoma, surgical options for diagnosis/treatment, current thoughts of extent of resection (EOR) of tumor, and post-operative (neo)adjuvant treatment. Glioblastoma is not a disease that can be cured with surgery alone, however safely performed maximal surgical resection is shown to significantly increase progression free and overall survival while maximizing quality of life. Upon invariable tumor recurrence, re-resection also is shown to impact survival in a select group of patients. As adjuvant therapy continues to improve survival, the role of surgical resection in the treatment of glioblastoma looks to be further defined.
Keywords: Glioblastoma; neoplasm; neurosurgery; surgical resection; therapeutics.
Figures

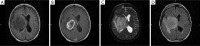


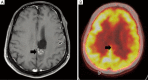


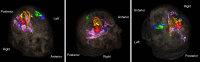
References
-
- Louis DN, International Agency for Research on Cancer, World Health Organization. WHO classification of tumours of the central nervous system. 4th ed. Lyon: International Agency for Research on Cancer, 2007.
-
- Ellor SV, Pagano-Young TA, Avgeropoulos NG. Glioblastoma: background, standard treatment paradigms, and supportive care considerations. J Law Med Ethics 2014;42:171-82. - PubMed
-
- Snyder H, Robinson K, Shah D, et al. Signs and symptoms of patients with brain tumors presenting to the emergency department. J Emerg Med 1993;11:253-8. - PubMed
-
- Witwer BP, Moftakhar R, Hasan KM, et al. Diffusion-tensor imaging of white matter tracts in patients with cerebral neoplasm. J Neurosurg 2002;97:568-75. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources
