Serum Uric Acid and Renal Transplantation Outcomes: At Least 3-Year Post-transplant Retrospective Multivariate Analysis
- PMID: 26208103
- PMCID: PMC4514650
- DOI: 10.1371/journal.pone.0133834
Serum Uric Acid and Renal Transplantation Outcomes: At Least 3-Year Post-transplant Retrospective Multivariate Analysis
Abstract
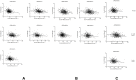
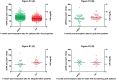
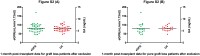
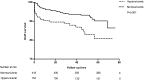
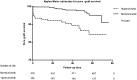
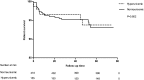
Since the association of serum uric acid and kidney transplant graft outcome remains disputable, we sought to evaluate the predictive value of uric acid level for graft survival/function and the factors could affect uric acid as time varies. A consecutive cohort of five hundred and seventy three recipients transplanted during January 2008 to December 2011 were recruited. Data and laboratory values of our interest were collected at 1, 3, 6, 12, 24 and 36 months post-transplant for analysis. Cox proportional hazard model, and multiple regression equation were built to adjust for the possible confounding variables and meet our goals as appropriate. The current cohort study lasts for 41.86 ± 15.49 months. Uric acid level is proven to be negatively associated with eGFR at different time point after adjustment for age, body mass index and male gender (standardized β ranges from -0.15 to -0.30 with all P<0.001).Males with low eGFR but high level of TG were on CSA, diuretics and RAS inhibitors and experienced at least one episode of acute rejection and diabetic issue were associated with a higher mean uric acid level. Hyperuricemia was significantly an independent predictor of pure graft failure (hazard ratio=4.01, 95% CI: 1.25-12.91, P=0.02) after adjustment. But it was no longer an independent risk factor for graft loss after adjustment. Interestingly, higher triglyceride level can make incidence of graft loss (hazard ratio=1.442, for each unit increase millimoles per liter 95% CI: 1.008-2.061, P=0.045) and death (hazard ratio=1.717, 95% CI: 1.105-2.665, P=0.016) more likely. The results of our study suggest that post-transplant elevated serum uric acid level is an independent predictor of long-term graft survival and graft function. Together with the high TG level impact on poor outcomes, further investigations for therapeutic effect are needed.
Conflict of interest statement
Figures
Similar articles
-
The independent association between serum uric acid and graft outcomes after kidney transplantation.Transplantation. 2010 Mar 15;89(5):573-9. doi: 10.1097/TP.0b013e3181c73c18. Transplantation. 2010. PMID: 19997058
-
Kidney Transplantation From Old Deceased Donors: Impact of Uric Acid Level-A Quarter-Century of Experience in One Transplant Center.Transplant Proc. 2018 Jul-Aug;50(6):1701-1704. doi: 10.1016/j.transproceed.2018.02.127. Epub 2018 Mar 14. Transplant Proc. 2018. PMID: 30056885
-
Uric acid contributes to glomerular filtration rate deterioration in renal transplantation.Nephron Clin Pract. 2011;118(2):c136-42. doi: 10.1159/000320616. Epub 2010 Dec 10. Nephron Clin Pract. 2011. PMID: 21150221
-
Uric acid and transplantation.Semin Nephrol. 2005 Jan;25(1):50-5. doi: 10.1016/j.semnephrol.2004.09.008. Semin Nephrol. 2005. PMID: 15660335 Review.
-
The Impact of hyperuricemia on long-term clinical outcomes of renal transplant recipients: a systematic review and meta-analysis.J Pharm Pharm Sci. 2021;24:292-307. doi: 10.18433/jpps31620. J Pharm Pharm Sci. 2021. PMID: 34107240
Cited by
-
Serum Uric Acid Is Positively Associated with Muscle Mass and Strength, but Not with Functional Capacity, in Kidney Transplant Patients.Nutrients. 2020 Aug 10;12(8):2390. doi: 10.3390/nu12082390. Nutrients. 2020. PMID: 32785016 Free PMC article.
-
Association between post-transplant uric acid level and renal allograft fibrosis: Analysis using Banff pathologic scores from renal biopsies.Sci Rep. 2018 Aug 2;8(1):11601. doi: 10.1038/s41598-018-29948-9. Sci Rep. 2018. PMID: 30072753 Free PMC article.
-
Prevalence of Musculoskeletal and Metabolic Disorders in Kidney Transplant Recipients: A Systematic Review and Meta-Analysis.Transpl Int. 2024 Apr 24;37:12312. doi: 10.3389/ti.2024.12312. eCollection 2024. Transpl Int. 2024. PMID: 38720821 Free PMC article.
References
-
- Levy AR, Briggs AH, Johnston K, MacLean JR, Yuan Y, L'Italien GJ, et al. Projecting long-term graft and patient survival after transplantation. Value in health: the journal of the International Society for Pharmacoeconomics and Outcomes Research. 2014;17(2):254–60. Epub 2014/03/19. 10.1016/j.jval.2014.01.001 . - DOI - PubMed
-
- Sarnak MJ, Levey AS, Schoolwerth AC, Coresh J, Culleton B, Hamm LL, et al. Kidney disease as a risk factor for development of cardiovascular disease: a statement from the American Heart Association Councils on Kidney in Cardiovascular Disease, High Blood Pressure Research, Clinical Cardiology, and Epidemiology and Prevention. Circulation. 2003;108(17):2154–69. Epub 2003/10/29. 10.1161/01.CIR.0000095676.90936.80 . - DOI - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

