Lack of cardioprotection by single-dose magnesium prophylaxis on isoprenaline-induced myocardial infarction in adult Wistar rats
- PMID: 26212925
- PMCID: PMC4780018
- DOI: 10.5830/CVJA-2015-055
Lack of cardioprotection by single-dose magnesium prophylaxis on isoprenaline-induced myocardial infarction in adult Wistar rats
Abstract
Aim: Magnesium (Mg(2+)) is effective in treating cardiovascular disorders such as arrhythmias and pre-eclampsia, but its role during myocardial infarction (MI) remains uncertain. In this study, we investigated the effects of Mg(2+)pre-treatment on isoprenaline (ISO) -induced MI in vivo.
Methods: Rats divided into four groups were each pre-treated with either MgSO4 (270 mg/kg intraperitoneally) or an equivalent volume of physiological saline, prior to the ISO (67 mg/kg subcutaneously) or saline treatments. One day post-treatment, the electrocardiogram and left ventricular blood pressures were recorded. Infarcts were determined using 2,3,5-triphenyltetrazolium chloride staining, and serum markers of lipid peroxidation were measured with spectrophotometric assays.
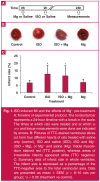
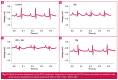
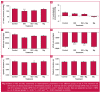
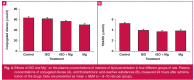
Results: Mg(2+) pre-treatment neither altered the ISO-induced infarct size compared with ISO treatment alone (p > 0.05), nor reversed the low-voltage electrocardiogram or the prominent Q waves induced by ISO, despite a trend to decreased Q waves. Similarly, Mg(2+) did not prevent the ISO-induced decrease in peak left ventricular blood pressure or the decrease in minimal rate of pressure change. Mg(2+) did not reverse the ISO-induced gain in heart weight or loss of body weight. Neither ISO nor Mg(2+) altered the concentrations of lipid peroxidation markers 24 hours post MI induction.
Conclusion: Although Mg(2+) had no detrimental effects on electrical or haemodynamic activity in ISO-induced MI, the lack of infarct prevention may detract from its utility in MI therapy.
Figures
Similar articles
-
Cardioprotective and Anti-arrhythmic Effects of Magnesium Pretreatment Against Ischaemia/Reperfusion Injury in Isoprenaline-Induced Hypertrophic Rat Heart.Cardiovasc Toxicol. 2017 Jan;17(1):49-57. doi: 10.1007/s12012-015-9355-6. Cardiovasc Toxicol. 2017. PMID: 26696240
-
Acute treatment with metformin improves cardiac function following isoproterenol induced myocardial infarction in rats.Pharmacol Rep. 2012;64(6):1476-84. doi: 10.1016/s1734-1140(12)70945-3. Pharmacol Rep. 2012. PMID: 23406758
-
Cardioprotective effect of HPLC standardized ethanolic extract of Terminalia pallida fruits against isoproterenol-induced myocardial infarction in albino rats.J Ethnopharmacol. 2012 May 7;141(1):33-40. doi: 10.1016/j.jep.2012.01.011. Epub 2012 Feb 1. J Ethnopharmacol. 2012. PMID: 22366678
-
Mechanisms of cardioprotective effect of Withania somnifera in experimentally induced myocardial infarction.Basic Clin Pharmacol Toxicol. 2004 Apr;94(4):184-90. doi: 10.1111/j.1742-7843.2004.pto940405.x. Basic Clin Pharmacol Toxicol. 2004. PMID: 15078343
-
Folic acid and vitamin B(12) supplementation attenuates isoprenaline-induced myocardial infarction in experimental hyperhomocysteinemic rats.Pharmacol Res. 2002 Sep;46(3):213-19. doi: 10.1016/s1043-6618(02)00095-6. Pharmacol Res. 2002. PMID: 12220963
Cited by
-
(E)-N'-(1-(7-Hydroxy-2-Oxo-2H-Chromen-3-Yl) Ethylidene) Benzohydrazide, a Novel Synthesized Coumarin, Ameliorates Isoproterenol-Induced Myocardial Infarction in Rats through Attenuating Oxidative Stress, Inflammation, and Apoptosis.Oxid Med Cell Longev. 2020 Mar 6;2020:2432918. doi: 10.1155/2020/2432918. eCollection 2020. Oxid Med Cell Longev. 2020. PMID: 32215169 Free PMC article.
-
Integration of Metabolomics With Pharmacodynamics to Elucidate the Anti-myocardial Ischemia Effects of Combination of Notoginseng Total Saponins and Safflower Total Flavonoids.Front Pharmacol. 2018 Jun 25;9:667. doi: 10.3389/fphar.2018.00667. eCollection 2018. Front Pharmacol. 2018. PMID: 29988484 Free PMC article.
-
Metabolomics analysis reveals the effects of Salvia Miltiorrhiza Bunge extract on ameliorating acute myocardial ischemia in rats induced by isoproterenol.Heliyon. 2024 Apr 30;10(9):e30488. doi: 10.1016/j.heliyon.2024.e30488. eCollection 2024 May 15. Heliyon. 2024. PMID: 38737264 Free PMC article.
References
-
- James MFM. Magnesium: an emerging drug in anaesthesia. Br J Anaesth. 2009;103:465–467. PMID:19749114. - PubMed
-
- Horner SM. Efficacy of intravenous magnesium in acute myocardial infarction in reducing arrhythmias and mortality. Meta-analysis of magnesium in acute myocardial infarction. Circulation. 1992;86:774–779. PMID:1387591. - PubMed
-
- Woods KL, Fletcher S, Roffe C, Haider Y. Intravenous magnesium sulphate in suspected acute myocardial infarction: results of the second Leicester Intravenous Magnesium Intervention Trial (LIMIT-2). Lancet. 1992;339:1553–1558. PMID:1351547. - PubMed
-
- Shechter M, Hod H, Chouraqui P, Kaplinsky E, Rabinowitz B. Magnesium therapy in acute myocardial infarction when patients are not candidates for thrombolytic therapy. Am J Cardiol. 1995;75:321–323. PMID:7856520. - PubMed
-
- Collins R Peto R Flather M Parish S Sleight P Conway M et al.ISIS-4: a randomised factorial trial assessing early oral captopril, oral mononitrate, and intravenous magnesium sulphate in 58,050 patients with suspected acute myocardial infarction. ISIS-4 (Fourth International Study of Infarct Survival) Collaborative. Lancet 1995345669–685.PMID:7661937 - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

