Risk Factors for Delayed Enteral Nutrition in Critically Ill Children
- PMID: 26237658
- PMCID: PMC4592402
- DOI: 10.1097/PCC.0000000000000527
Risk Factors for Delayed Enteral Nutrition in Critically Ill Children
Abstract
Objective: Delayed enteral nutrition, defined as enteral nutrition started 48 hours or more after admission to the PICU, is associated with an inability to achieve full enteral nutrition and worse outcomes in critically ill children. We reviewed nutritional practices in six medical-surgical PICUs and determined risk factors associated with delayed enteral nutrition in critically ill children.
Design: Retrospective cross-sectional study using medical records as source of data.
Setting: Six medical-surgical PICUs in northeastern United States.
Patients: Children less than 21 years old admitted to the PICU for 72 hours or more excluding those awaiting or recovering from abdominal surgery.
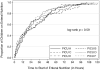
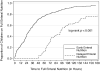
Measurements and main results: A total of 444 children with a median age of 4.0 years were included in the study. Enteral nutrition was started at a median time of 20 hours after admission to the PICU. There was no significant difference in time to start enteral nutrition among the PICUs. Of those included, 88 children (19.8%) had delayed enteral nutrition. Risk factors associated with delayed enteral nutrition were noninvasive (odds ratio, 3.37; 95% CI, 1.69-6.72) and invasive positive-pressure ventilation (odds ratio, 2.06; 95% CI, 1.15-3.69), severity of illness (odds ratio for every 0.1 increase in pediatric index of mortality 2 score, 1.39; 95% CI, 1.14-1.71), procedures (odds ratio, 3.33; 95% CI, 1.67-6.64), and gastrointestinal disturbances (odds ratio, 2.05; 95% CI, 1.14-3.68) within 48 hours after admission to the PICU. Delayed enteral nutrition was associated with failure to reach full enteral nutrition while in the PICU (odds ratio, 4.09; 95% CI, 1.97-8.53). Nutrition consults were obtained in less than half of the cases, and none of the PICUs used tools to assure the adequacy of energy and protein nutrition.
Conclusions: Institutions in this study initiated enteral nutrition for a high percentage of patients by 48 hours of admission. Noninvasive positive-pressure ventilation was most strongly associated with delay enteral nutrition. A better understanding of these risk factors and assessments of nutritional requirements should be explored in future prospective studies.
Conflict of interest statement
The other authors do not have any real or perceived conflicts of interest.
Figures
Comment in
-
Early Enteral Nutrition in the PICU: Should We Trust Our Gut?Pediatr Crit Care Med. 2015 Oct;16(8):786-9. doi: 10.1097/PCC.0000000000000530. Pediatr Crit Care Med. 2015. PMID: 26427815 No abstract available.
References
-
- Hulst JM, van Goudoever JB, Zimmermann LJ, et al. The effect of cumulative energy and protein deficiency on anthropometric parameters in a pediatric ICU population. Clin Nutr. 2004;23:1381–1389. - PubMed
-
- Pollack MM, Ruttimann UE, Wiley JS. Nutritional depletions in critically ill children: associations with physiologic instability and increased quantity of care. JPEN Journal of Parenteral and Enteral Nutrition. 1985;9:309–313. - PubMed
-
- Briassoulis G, Zavras N, Hatzis T. Malnutrition, nutritional indices, and early enteral feeding in critically ill children. Nutrition. 2001;17:548–557. - PubMed
-
- Leite HP, Isatugo MK, Sawaki L, et al. Anthropometric nutritional assessment of critically ill hospitalized children. Rev Paul Med. 1993;111:309–313. - PubMed
-
- Joosten K, de Betue C. Adequate enteral feeding in the pediatric intensive care unit may be associated with fewer nosocomial infections and deaths. Evid Based Med. 2013;18:151–152. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources