Neuroendocrine Disorders in Pediatric Craniopharyngioma Patients
- PMID: 26239246
- PMCID: PMC4470135
- DOI: 10.3390/jcm4030389
Neuroendocrine Disorders in Pediatric Craniopharyngioma Patients
Abstract
Childhood-onset craniopharyngiomas are partly cystic embryonic malformations of the sellar/parasellar region. The therapy of choice in patients with favorable tumor localization is complete resection with a specific focus on maintaining optical and hypothalamic neuroendocrine functions. In patients with unfavorable tumor localization (i.e., hypothalamic involvement), a limited hypothalamus-sparing surgical strategy followed by local irradiation is recommended. Involvement and/or surgical lesions of posterior hypothalamic areas cause major neuroendocrine sequelae. The overall survival rates are high (92%) but neuroendocrine disorders such as obesity and metabolic syndrome due to involvement and/or treatment-related hypothalamic lesions have major negative impact on survival and quality of life. Recurrences and progressions are frequent post-surgical events. Because irradiation is efficient in preventing tumor progression, appropriate timing of post-surgical irradiation is currently under investigation in a randomized multinational trial (KRANIOPHARYNGEOM 2007). Childhood-onset craniopharyngioma should be recognized as a chronic disease requiring treatment and constant monitoring of the clinical and quality of life consequences, frequently impaired due to neuroendocrine disorders, by experienced multidisciplinary teams in order to provide optimal care of surviving patients.
Keywords: brain tumors; craniopharyngioma; hypothalamic obesity; irradiation; neurocognitive; neuroendocrinology; neurosurgery; pituitary; quality of life; recurrence; sleep.
Figures
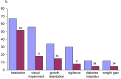





References
-
- Muller H.L. Childhood craniopharyngioma: Current controversies on management in diagnostics, treatment and follow-up. Expert Rev. Neurother. 2010;10:515–524. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources
Molecular Biology Databases

