Retrospective study of the predictors of mortality and radiographic deterioration in 782 patients with nodular/bronchiectatic Mycobacterium avium complex lung disease
- PMID: 26246077
- PMCID: PMC4538251
- DOI: 10.1136/bmjopen-2015-008058
Retrospective study of the predictors of mortality and radiographic deterioration in 782 patients with nodular/bronchiectatic Mycobacterium avium complex lung disease
Abstract
Objectives: Some patients with nodular/bronchiectatic Mycobacterium avium complex lung disease (NB MAC-LD) deteriorate and die. The main aim of the study is to evaluate the prognostic factors and radiographic outcomes in patients with NB MAC-LD.
Setting: Retrospective single-centre review.
Participants: 782 HIV-negative patients with NB MAC-LD treated at our institution in Japan.
Primary and secondary outcome measures: All-cause and MAC-LD progression mortality rates and the prognostic factors, and radiographic deterioration rates and the prognostic factors.
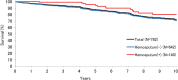
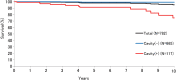
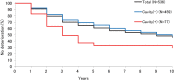
Results: Mean age was 68.1 years, and median follow-up period was 4.3 years. Death from any cause and progression of MAC lung disease (MAC-LD) occurred in 130 (16.6%), and 19 (2.4%) patients, respectively. All-cause and MAC-LD progression 10-year mortality rates were 27.4% and 4.8%, respectively. In 536 patients with MAC-LD who were followed-up for more than 1 year, radiographic deterioration occurred in 221 (41.2%) patients and median time-to-radiographic deterioration was 9 years. A multivariate Cox proportional hazard model showed male sex, older age, body mass index <18.5 kg/m(2), absence of bloody sputum, hypoalbuminaemia and erythrocyte sedimentation rate >40 mm/h to be negative prognostic factors for all-cause mortality, and the presence of idiopathic pulmonary fibrosis, haemoglobin <11.3 mg/dL, C reactive protein >1.0 mg/dL and the presence of cavity to be negative prognostic factors for radiographic deterioration.
Conclusions: Only 2.4% of patients with NB MAC-LD died from MAC-LD progression. As clinical trials testing the effectiveness of drug therapy in patients with NB MAC-LD are being designed and implemented, the primary end point could be time-to-radiographic deterioration, and trial patients need to be stratified according to these prognostic factors before randomisation.
Published by the BMJ Publishing Group Limited. For permission to use (where not already granted under a licence) please go to http://group.bmj.com/group/rights-licensing/permissions.
Figures
References
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous
