Hypercoagulability Is a Stronger Risk Factor for Ischaemic Stroke than for Myocardial Infarction: A Systematic Review
- PMID: 26252207
- PMCID: PMC4529149
- DOI: 10.1371/journal.pone.0133523
Hypercoagulability Is a Stronger Risk Factor for Ischaemic Stroke than for Myocardial Infarction: A Systematic Review
Abstract
Background and purpose: Hypercoagulability increases the risk of arterial thrombosis; however, this effect may differ between various manifestations of arterial disease.
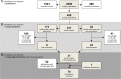
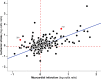
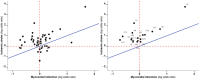
Methods: In this study, we compared the effect of coagulation factors as measures of hypercoagulability on the risk of ischaemic stroke (IS) and myocardial infarction (MI) by performing a systematic review of the literature. The effect of a risk factor on IS (relative risk for IS, RRIS) was compared with the effect on MI (RRMI) by calculating their ratio (RRR = RRIS/RRMI). A relevant differential effect was considered when RRR was >1+ its own standard error (SE) or <1-SE.
Results: We identified 70 publications, describing results from 31 study populations, accounting for 351 markers of hypercoagulability. The majority (203/351, 58%) had an RRR greater than 1. A larger effect on IS risk than MI risk (RRE>1+1SE) was found in 49/343 (14%) markers. Of these, 18/49 (37%) had an RRR greater than 1+2SE. On the opposite side, a larger effect on MI risk (RRR<1-1SE) was found in only 17/343 (5%) markers.
Conclusions: These results suggest that hypercoagulability has a more pronounced effect on the risk of IS than that of MI.
Conflict of interest statement
Figures
References
-
- Simons LA, Simons J. A Comparison of Risk Factors for Coronary Heart Disease and Ischaemic Stroke. Heart Lung and Circulation. 2012;21(3): 198–9. - PubMed
-
- Borissoff JI, Spronk HMH, ten Cate H. Mechanisms of Disease the Hemostatic System As A Modulator of Atherosclerosis. New England Journal of Medicine. 2011;364(18): 1746–60. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

