Curative Resection of Adrenocortical Carcinoma: Rates and Patterns of Postoperative Recurrence
- PMID: 26282907
- PMCID: PMC4962540
- DOI: 10.1245/s10434-015-4810-y
Curative Resection of Adrenocortical Carcinoma: Rates and Patterns of Postoperative Recurrence
Abstract
Background: Adrenocortical carcinoma (ACC) is a rare malignancy. The aim of this study was to determine the incidence and patterns of recurrence after curative-intent surgery for ACC.
Methods: Patients who underwent curative-intent resection for ACC between 1993 and 2014 were identified from 13 academic institutions participating in the United States ACC study group. Patients with metastasis or an R2 margin were excluded. Patterns and rates of recurrence were determined and classified as locoregional and distant recurrence.
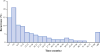
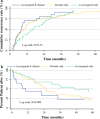
Results: A total of 180 patients with a median age of 52 years (interquartile range 43-61) were identified. Most patients underwent open surgery (n = 111, 64.5 %) and had an R0 resection margin (n = 117, 75.0 %). At last follow-up, 116 patients (64.4 %) had experienced recurrence (locoregional only, n = 41, 36.3 %; distant only, n = 51, 45.1 %; locoregional and distant, n = 21, 18.6 %). Median time to recurrence was 18.8 months. Several factors were associated with locoregional recurrence, including left-sided ACC location (odds ratio [OR] 2.71, 95 % confidence interval [CI] 1.06-6.89) and T3/T4 disease (reference T1/T2, OR 3.04, 95 % CI 1.19-7.80) (both p < 0.05). Distant recurrence was associated with larger tumor size (OR 1.11, 95 % CI 1.01-1.24) and T3/T4 disease (reference T1/T2, OR 5.23, 95 % CI 1.70-16.10) (both p < 0.05). Patients with combined locoregional and distant recurrence had worse survival (3- and 5-year survival: 39.5, 19.7 %) versus patients with distant-only (3- and 5-year survival 55.1, 43.3 %) or locoregional-only recurrence (3- and 5-year survival 81.4, 64.1 %) (p = 0.01).
Conclusions: Nearly two-thirds of patients experienced disease recurrence after resection of ACC. Although a subset of patients experienced recurrence with locoregional disease only, many patients experienced recurrence with distant disease as a component of recurrence and had a poor prognosis.
Conflict of interest statement
Figures
References
-
- Kebebew E, Reiff E, Duh QY, Clark OH, McMillan A. Extent of disease at presentation and outcome for adrenocortical carcinoma: have we made progress? World J Surg. 2006;30:872–78. - PubMed
-
- Fassnacht M, Johanssen S, Fenske W, et al. Improved survival in patients with stage II adrenocortical carcinoma followed up prospectively by specialized centers. J Clin Endocrinol Metab. 2010;95:4925–32. - PubMed
-
- Dackiw AP, Lee JE, Gagel RF, Evans DB. Adrenal cortical carcinoma. World J Surg. 2001;25:914–26. - PubMed
-
- Pommier RF, Brennan MF. An eleven-year experience with adrenocortical carcinoma. Surgery. 1992;112:963–70. - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical