Mycobacterium abscessus Complex Infections in Humans
- PMID: 26295364
- PMCID: PMC4550155
- DOI: 10.3201/2109.141634
Mycobacterium abscessus Complex Infections in Humans
Abstract
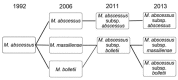
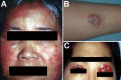
Mycobacterium abscessus complex comprises a group of rapidly growing, multidrug-resistant, nontuberculous mycobacteria that are responsible for a wide spectrum of skin and soft tissue diseases, central nervous system infections, bacteremia, and ocular and other infections. M. abscessus complex is differentiated into 3 subspecies: M. abscessus subsp. abscessus, M. abscessus subsp. massiliense, and M. abscessus subsp. bolletii. The 2 major subspecies, M. abscessus subsp. abscessus and M. abscessus subsp. massiliense, have different erm(41) gene patterns. This gene provides intrinsic resistance to macrolides, so the different patterns lead to different treatment outcomes. M. abscessus complex outbreaks associated with cosmetic procedures and nosocomial transmissions are not uncommon. Clarithromycin, amikacin, and cefoxitin are the current antimicrobial drugs of choice for treatment. However, new treatment regimens are urgently needed, as are rapid and inexpensive identification methods and measures to contain nosocomial transmission and outbreaks.
Keywords: Mycobacterium abscessus; Mycobacterium abscessus complex; Mycobacterium bolletii; Mycobacterium massiliense; bacteria; clinical disease; cosmetic procedures; identification methods; multidrug resistant; mycobacteria; nomenclature; nontuberculous; nosocomial; outbreaks; taxonomy; transmission.
Figures
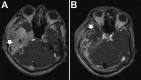
References
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
