Acceptability and adherence to Isoniazid preventive therapy in HIV-infected patients clinically screened for latent tuberculosis in Dar es Salaam, Tanzania
- PMID: 26306511
- PMCID: PMC4549887
- DOI: 10.1186/s12879-015-1085-7
Acceptability and adherence to Isoniazid preventive therapy in HIV-infected patients clinically screened for latent tuberculosis in Dar es Salaam, Tanzania
Abstract
Background: Proper adherence to isoniazid preventive therapy (IPT) may depend upon the results of tuberculosis (TB) screening test and patients' understanding of their risk of developing active TB. We conducted a study to assess the acceptability, adherence and completion profile of IPT among HIV-infected patients who were clinically screened for latent TB Infection (LTBI).
Methods: A multicenter observational study was conducted in Dar es Salaam, Tanzania between February 2012 and March 2014. HIV-infected patients 10 years or older were clinically screened using a validated symptom-based screening tool to rule out active TB. Patients found to have no symptoms in the screening tool were given 300 mg of isoniazid (INH) daily for 6 months. Patients were followed up monthly at the National and Municipal hospital HIV clinics for INH refill and assessment of treatment adherence. Adherence was defined as consumption of 90 % or more of the monthly prescription of INH.
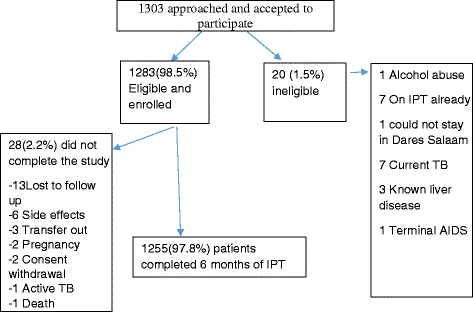
Results: All 1303 invited patients agreed to participate in the study. Of 1303 invited HIV-infected patients, 1283 (98.5 %) were recruited into the study. Twenty eight (2.2 %) did not complete treatment. Those who did not complete the treatment were exclusively adults aged 18 years or older, p = 0.302. The overall mean (±SD) adherence was 98.9 % (±2.9). Adherence level among children aged <18 years (92.2 %) was significantly lower than adherence level among patients aged 18-29 years (98.3 %), 30-49 years (98.8 %) and ≥ 50 years (98.5), p-value = 0.011. Sex, occupation, socio-economic status, duration of HIV infection, being on antiretroviral drugs (ARV) and duration of ARV use were not associated with adherence.
Conclusion: IPT is highly accepted by HIV infected patients. Patients demonstrated high level of adherence to IPT. The level of adherence among children was slightly lower than that among adults. IPT non-completers were exclusively adults. Children might need adult supervision in taking IPT.
Figures
Similar articles
-
Cost-Effectiveness of isoniazid preventive therapy among HIV-infected patients clinicaly screened for latent tuberculosis infection in Dar es Salaam, Tanzania: A prospective Cohort study.BMC Public Health. 2017 Jul 19;18(1):35. doi: 10.1186/s12889-017-4597-9. BMC Public Health. 2017. PMID: 28724374 Free PMC article.
-
Effect of isoniazid preventive therapy on tuberculosis incidence and associated risk factors among HIV infected adults in Tanzania: a retrospective cohort study.BMC Infect Dis. 2019 Jan 17;19(1):62. doi: 10.1186/s12879-019-3696-x. BMC Infect Dis. 2019. PMID: 30654753 Free PMC article.
-
Successful implementation of isoniazid preventive therapy at a pediatric HIV clinic in Tanzania.BMC Infect Dis. 2020 Oct 7;20(1):738. doi: 10.1186/s12879-020-05471-z. BMC Infect Dis. 2020. PMID: 33028260 Free PMC article.
-
Treatment guidelines for latent tuberculosis infection.Kekkaku. 2014 Jan;89(1):21-37. Kekkaku. 2014. PMID: 24654427 Review.
-
Isoniazid preventive therapy in HIV-infected and -uninfected children (0 - 14 years).S Afr Med J. 2013 Sep 4;103(10):714-5. doi: 10.7196/samj.7189. S Afr Med J. 2013. PMID: 24079619 Review.
Cited by
-
Increased uptake of tuberculosis preventive therapy (TPT) among people living with HIV following the 100-days accelerated campaign: A retrospective review of routinely collected data at six urban public health facilities in Uganda.PLoS One. 2023 Feb 23;18(2):e0268935. doi: 10.1371/journal.pone.0268935. eCollection 2023. PLoS One. 2023. PMID: 36821550 Free PMC article.
-
Implementing isoniazid preventive therapy in a tuberculosis treatment-experienced cohort on ART.Int J Tuberc Lung Dis. 2017 May 1;21(5):537-543. doi: 10.5588/ijtld.16.0775. Int J Tuberc Lung Dis. 2017. PMID: 28399969 Free PMC article.
-
The social implications of participant choice on adherence to Isonaizid Preventive Therapy (IPT): A follow-up study to high completion rates in Eswatini.PLoS One. 2020 May 29;15(5):e0232841. doi: 10.1371/journal.pone.0232841. eCollection 2020. PLoS One. 2020. PMID: 32469990 Free PMC article.
-
Loss to follow-up among people living with HIV on tuberculosis preventive treatment at four regional referral hospitals, Uganda, 2019-2021.J Clin Tuberc Other Mycobact Dis. 2024 Jun 8;36:100454. doi: 10.1016/j.jctube.2024.100454. eCollection 2024 Aug. J Clin Tuberc Other Mycobact Dis. 2024. PMID: 38966799 Free PMC article.
-
Determinants of isoniazid preventive therapy completion among people living with HIV attending care and treatment clinics from 2013 to 2017 in Dar es Salaam Region, Tanzania. A cross-sectional analytical study.BMC Infect Dis. 2020 Apr 10;20(1):276. doi: 10.1186/s12879-020-04997-6. BMC Infect Dis. 2020. PMID: 32276618 Free PMC article.
References
-
- WHO. Global Tuberculosis Report 2014 Geneva, Switzerland; 2014. Available from: http://apps.who.int/iris/bitstream/10665/137094/1/9789241564809_eng.pdf?.... Accessed February 10, 2015.
-
- WHO. Guidelines for intensified case finding isoniazid preventive therapy for people living with HIV in resource constrained settings. 2011. Available from http://whqlibdoc.who.int/publications/2011/9789241500708_eng.pdf. Acessed February 10, 2015.
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical