Impact of a Contralateral Tumor Nodule on Survival in Non-Small-Cell Lung Cancer
- PMID: 26317917
- PMCID: PMC4636460
- DOI: 10.1097/JTO.0000000000000655
Impact of a Contralateral Tumor Nodule on Survival in Non-Small-Cell Lung Cancer
Abstract
Introduction: Contralateral lung tumors in non-small-cell lung cancer (NSCLC) are classified as stage M1a yet may represent hematogenous metastases or synchronous primary tumors. The impact of these tumors on overall survival (OS) is poorly understood. Here, we aim to determine whether NSCLC patients with M1a disease due only to a contralateral tumor nodule exhibit a favorable prognosis relative to other M1a or M1b patients.
Methods: Retrospective evaluation of the impact of contralateral tumor nodules on OS in NSCLC stratified by primary tumor size and N stage attained from Surveillance, Epidemiology, and End Results database.
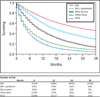
Results: Of 173,640 patients, 5161 M1a-contra patients were identified. Median and 3-year OS for these patients exceeded that of patients with M1b (p < 0.0001) or other M1a disease (p < 0.0001). Primary tumor size and N stage were strongly associated with OS in M1a-contra patients. Three-year OS demonstrated a delayed convergence between M1a-contra and other M1a patients with primary tumors greater than or equal to 3 cm or mediastinal lymph node involvement. Proportional hazard modeling indicated that T1-2N0-1M1a-contra patients exhibit OS not significantly different (p = 0.258) from that predicted with comparable T and N stage disease plus a second early-stage primary.
Conclusions: Contralateral tumors in NSCLC carry a more favorable prognosis than other M1a or M1b disease. Primary tumor size and N stage may help distinguish M1a-contra patients with hematogenous metastasis from those with a synchronous, second primary.
Conflict of interest statement
Figures




Similar articles
-
Tumor, node and metastasis classification of lung cancer--M1a versus M1b--analysis of M descriptors and other prognostic factors.Lung Cancer. 2014 May;84(2):182-9. doi: 10.1016/j.lungcan.2014.02.006. Epub 2014 Feb 23. Lung Cancer. 2014. PMID: 24629637
-
Does Lymph Node Metastasis Have a Negative Prognostic Impact in Patients with NSCLC and M1a Disease?J Thorac Oncol. 2016 Oct;11(10):1745-54. doi: 10.1016/j.jtho.2016.06.030. Epub 2016 Aug 24. J Thorac Oncol. 2016. PMID: 27567989
-
The impact of extent and location of mediastinal lymph node involvement on survival in Stage III non-small cell lung cancer patients treated with definitive radiotherapy.Int J Radiat Oncol Biol Phys. 2012 May 1;83(1):340-7. doi: 10.1016/j.ijrobp.2011.05.070. Epub 2011 Nov 19. Int J Radiat Oncol Biol Phys. 2012. PMID: 22104359
-
The revised TNM staging system for lung cancer.Ann Thorac Cardiovasc Surg. 2009 Feb;15(1):4-9. Ann Thorac Cardiovasc Surg. 2009. PMID: 19262443 Review.
-
Current readings: the most influential and recent studies regarding resection of lung cancer in m1a disease.Semin Thorac Cardiovasc Surg. 2013 Autumn;25(3):251-5. doi: 10.1053/j.semtcvs.2013.08.002. Semin Thorac Cardiovasc Surg. 2013. PMID: 24331148 Review.
Cited by
-
Prediction model for hyperprogressive disease in non-small cell lung cancer treated with immune checkpoint inhibitors.Thorac Cancer. 2020 Oct;11(10):2793-2803. doi: 10.1111/1759-7714.13594. Epub 2020 Aug 11. Thorac Cancer. 2020. PMID: 32779394 Free PMC article.
-
A novel LASSO-derived prognostic model predicting survival for non-small cell lung cancer patients with M1a diseases.Cancer Med. 2022 Mar;11(6):1561-1572. doi: 10.1002/cam4.4560. Epub 2022 Feb 6. Cancer Med. 2022. PMID: 35128839 Free PMC article.
References
-
- Goldstraw P, Crowley J, Chansky K, et al. The IASLC Lung Cancer Staging Project: proposals for the revision of the TNM stage groupings in the forthcoming (seventh) edition of the TNM Classification of malignant tumours. Journal of thoracic oncology : official publication of the International Association for the Study of Lung Cancer. 2007 Aug;2(8):706–714. - PubMed
-
- Kim AW, Cooke DT. Additional pulmonary nodules in the patient with lung cancer: controversies and challenges. Clinics in chest medicine. 2011 Dec;32(4):811–825. - PubMed
-
- Aisner DL, Marshall CB. Molecular pathology of non-small cell lung cancer: a practical guide. American journal of clinical pathology. 2012 Sep;138(3):332–346. - PubMed
-
- Martini N, Melamed MR. Multiple primary lung cancers. The Journal of thoracic and cardiovascular surgery. 1975 Oct;70(4):606–612. - PubMed
-
- Adamo M, Dickie L, J R. 2014 SEER Program Coding and Staging Manual and Appendix C. Bethesda, MD: National Cancer Institute; 2014. pp. 20850–29765.
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

