End-of-Life Practices Among Tertiary Care PICUs in the United States: A Multicenter Study
- PMID: 26335128
- PMCID: PMC4562059
- DOI: 10.1097/PCC.0000000000000520
End-of-Life Practices Among Tertiary Care PICUs in the United States: A Multicenter Study
Abstract
Objective: To describe variability in end-of-life practices among tertiary care PICUs in the United States.
Design: Secondary analysis of data prospectively collected from a random sample of patients (n = 10,078) admitted to PICUs affiliated with the Collaborative Pediatric Critical Care Research Network between December 4, 2011, and April 7, 2013.
Setting: Seven clinical centers affiliated with the Collaborative Pediatric Critical Care Research Network.
Patients: Patients included in the primary study were less than 18 years old, admitted to a PICU, and not moribund on PICU admission. Patients included in the secondary analysis were those who died during their hospital stay.
Interventions: None.
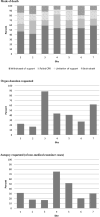
Measurements and main results: Two hundred and seventy-five (2.7%; range across sites, 1.3-5.0%) patients died during their hospital stay; of these, 252 (92%; 76-100%) died in a PICU. Discussions with families about limitation or withdrawal of support occurred during the initial PICU stay for 173 patients (63%; 47-76%; p = 0.27) who died. Of these, palliative care was consulted for 67 (39%; 12-46%); pain service for 11 (6%; 10 of which were at a single site); and ethics committee for six (3%, from three sites). Mode of death was withdrawal of support for 141 (51%; 42-59%), failed cardiopulmonary resuscitation for 53 (19%; 12-28%), limitation of support for 46 (17%; 7-24%), and brain death for 35 (13%; 8-20%); mode of death did not differ across sites (p = 0.58). Organ donation was requested from 101 families (37%; 17-88%; p < 0.001). Of these, 20 donated (20%; 0-64%). Sixty-two deaths (23%; 10-53%; p < 0.001) were medical examiner cases. Of nonmedical examiner cases (n = 213), autopsy was requested for 79 (37%; 17-75%; p < 0.001). Of autopsies requested, 53 (67%; 50-100%) were performed.
Conclusions: Most deaths in Collaborative Pediatric Critical Care Research Network-affiliated PICUs occur after life support has been limited or withdrawn. Wide practice variation exists in requests for organ donation and autopsy.
Figures
References
-
- Fontana MS, Farrell C, Gauvin F, et al. Modes of death in pediatrics: Differences in the ethical approach in neonatal and pediatric patients. J Pediatr. 2013;162:1107–1111. - PubMed
-
- Launes C, Cambra FJ, Jordan I, et al. Withholding or withdrawing life-sustaining treatments: An 8-yr retrospective review in a Spanish pediatric intensive care unit. Pediatr Crit Care Med. 2011;12:e383–e385. - PubMed
-
- American Academy of Pediatrics. Section on Hospice and Palliative Medicine and Committee on Hospital Care: Pediatric palliative care and hospice care commitments, guidelines, and recommendations. Pediatrics. 2013;132:966–972. - PubMed
Publication types
MeSH terms
Grants and funding
- U10 HD063108/HD/NICHD NIH HHS/United States
- U01HD049934/HD/NICHD NIH HHS/United States
- U10 HD050012/HD/NICHD NIH HHS/United States
- U10HD049981/HD/NICHD NIH HHS/United States
- UG1 HD049983/HD/NICHD NIH HHS/United States
- UG1 HD050096/HD/NICHD NIH HHS/United States
- U10 HD050096/HD/NICHD NIH HHS/United States
- U10 HD049983/HD/NICHD NIH HHS/United States
- U10 HD063106/HD/NICHD NIH HHS/United States
- RL1 HD107773/HD/NICHD NIH HHS/United States
- U10HD063114/HD/NICHD NIH HHS/United States
- U10HD050096/HD/NICHD NIH HHS/United States
- U10 HD063114/HD/NICHD NIH HHS/United States
- U01 HD049934/HD/NICHD NIH HHS/United States
- UG1 HD049981/HD/NICHD NIH HHS/United States
- U10HD050012/HD/NICHD NIH HHS/United States
- U10 HD049981/HD/NICHD NIH HHS/United States
- U10HD063106/HD/NICHD NIH HHS/United States
- U10HD049983/HD/NICHD NIH HHS/United States
- U10HD063108/HD/NICHD NIH HHS/United States
LinkOut - more resources
Full Text Sources
Miscellaneous