Schistosoma mansoni Infection in Ugandan Men Is Associated with Increased Abundance and Function of HIV Target Cells in Blood, but Not the Foreskin: A Cross-sectional Study
- PMID: 26335139
- PMCID: PMC4559468
- DOI: 10.1371/journal.pntd.0004067
Schistosoma mansoni Infection in Ugandan Men Is Associated with Increased Abundance and Function of HIV Target Cells in Blood, but Not the Foreskin: A Cross-sectional Study
Abstract
Background: Schistosoma mansoni infection has been associated with an increased HIV prevalence in humans and SHIV incidence in primate models. We hypothesized that immune activation from this gastrointestinal mucosa infection would increase highly HIV-susceptible CD4 T cell subsets in the blood and the foreskin through common mucosal homing.
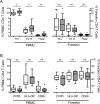
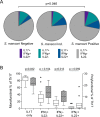
Methodology/principal findings: Foreskin tissue and blood were obtained from 34 HIV- and malaria-uninfected Ugandan men who volunteered for elective circumcision, 12 of whom were definitively positive for S. mansoni eggs in stool and 12 definitively negative for both S. mansoni eggs and worm antigen. Tissue and blood T cell subsets were characterized by flow cytometry and immunohistochemistry (IHC). Th17 and Th1 cells from both the blood and foreskin expressed higher levels of CCR5 and were more activated than other CD4 T cell subsets. S. mansoni-infected men had a higher frequency of systemic Th1 cells (22.9 vs. 16.5% of blood CD4 T cells, p<0.05), Th17 cells (2.3 vs. 1.5%, p<0.05), and Th22 cells (0.5 vs. 0.3%, p<0.01) than uninfected men. Additionally, Th17 cells in the blood of S. mansoni-infected men demonstrated enhanced function (28.1 vs. 16.3% producing multiple cytokines, p = 0.046). However, these immune alterations were not observed in foreskin tissue.
Conclusions/significance: S. mansoni infection was associated with an increased frequency of highly HIV-susceptible Th1, Th17 and Th22 cell subsets in the blood, but these T cell immune differences did not extend to the foreskin. S. mansoni induced changes in T cell immunology mediated through the common mucosal immune system are not likely to increase HIV susceptibility in the foreskin.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures


References
-
- UNAIDS. Global Report: UNAIDS report on the global AIDS epidemic 2013. WHO Library Cataloguing-in-Publication Data: 2013.
-
- Keele BF, Giorgi EE, Salazar-Gonzalez JF, Decker JM, Pham KT, Salazar MG, et al. Identification and characterization of transmitted and early founder virus envelopes in primary HIV-1 infection. Proc Natl Acad Sci U S A. 2008;105(21):7552–7. Epub 2008/05/21. 10.1073/pnas.0802203105 - DOI - PMC - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials

