Evaluation of bone regeneration potential of dental follicle stem cells for treatment of craniofacial defects
- PMID: 26342992
- PMCID: PMC4592822
- DOI: 10.1016/j.jcyt.2015.07.013
Evaluation of bone regeneration potential of dental follicle stem cells for treatment of craniofacial defects
Abstract
Background aims: Stem cell-based tissue regeneration offers potential for treatment of craniofacial bone defects. The dental follicle, a loose connective tissue surrounding the unerupted tooth, has been shown to contain progenitor/stem cells. Dental follicle stem cells (DFSCs) have strong osteogenesis capability, which makes them suitable for repairing skeletal defects. The objective of this study was to evaluate bone regeneration capability of DFSCs loaded into polycaprolactone (PCL) scaffold for treatment of craniofacial defects.
Methods: DFSCs were isolated from the first mandibular molars of postnatal Sprague-Dawley rats and seeded into the PCL scaffold. Cell attachment and cell viability on the scaffold were examined with the use of scanning electron microscopy and alamar blue reduction assay. For in vivo transplantation, critical-size defects were created on the skulls of 5-month-old immunocompetent rats, and the cell-scaffold constructs were transplanted into the defects.
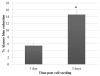
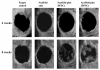
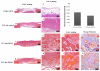
Results: Skulls were collected at 4 and 8 weeks after transplantation, and bone regeneration in the defects was evaluated with the use of micro-computed tomography and histological analysis. Scanning electron microscopy and Alamar blue assay demonstrated attachment and proliferation of DFSCs in the PCL scaffold. Bone regeneration was observed in the defects treated with DFSC transplantation but not in the controls without DFSC transplant. Transplanting DFSC-PCL with or without osteogenic induction before transplantation achieved approximately 50% bone regeneration at 8 weeks. Formation of woven bone was observed in the DFSC-PCL treatment group. Similar results were seen when osteogenic-induced DFSC-PCL was transplanted to the critical-size defects.
Conclusions: This study demonstrated that transplantation of DFSCs seeded into PCL scaffolds can be used to repair craniofacial defects.
Keywords: bone regeneration; craniofacial defects; dental follicle stem cells; stem cell transplantation.
Copyright © 2015 International Society for Cellular Therapy. Published by Elsevier Inc. All rights reserved.
Figures




Similar articles
-
CA1 induced dental follicle stem cells co-culture with dental pulp stem cells and loaded three-dimensional printed PCL/β-TCP scaffold: a novel strategy for alveolar cleft bone regeneration.J Mater Sci Mater Med. 2025 Apr 25;36(1):37. doi: 10.1007/s10856-025-06889-0. J Mater Sci Mater Med. 2025. PMID: 40278949 Free PMC article.
-
Repair of calvarial defects with customized tissue-engineered bone grafts I. Evaluation of osteogenesis in a three-dimensional culture system.Tissue Eng. 2003;9 Suppl 1:S113-26. doi: 10.1089/10763270360697021. Tissue Eng. 2003. PMID: 14511475
-
Xenogenous implanted dental follicle stem cells promote periodontal regeneration through inducing the N2 phenotype of neutrophils.Stem Cell Res Ther. 2024 Aug 26;15(1):270. doi: 10.1186/s13287-024-03882-2. Stem Cell Res Ther. 2024. PMID: 39183362 Free PMC article.
-
Dental Follicle Stem Cells: Tissue Engineering and Immunomodulation.Stem Cells Dev. 2019 Aug 1;28(15):986-994. doi: 10.1089/scd.2019.0012. Epub 2019 May 7. Stem Cells Dev. 2019. PMID: 30968740 Review.
-
Dental follicle stem cells and tissue engineering.J Oral Sci. 2010 Dec;52(4):541-52. doi: 10.2334/josnusd.52.541. J Oral Sci. 2010. PMID: 21206155 Review.
Cited by
-
Polymeric vs hydroxyapatite-based scaffolds on dental pulp stem cell proliferation and differentiation.World J Stem Cells. 2015 Nov 26;7(10):1215-21. doi: 10.4252/wjsc.v7.i10.1215. World J Stem Cells. 2015. PMID: 26640621 Free PMC article.
-
Bone regeneration driven by a nano-hydroxyapatite/chitosan composite bioaerogel for periodontal regeneration.Front Bioeng Biotechnol. 2024 Jul 30;12:1355950. doi: 10.3389/fbioe.2024.1355950. eCollection 2024. Front Bioeng Biotechnol. 2024. PMID: 39139296 Free PMC article.
-
A ROS-responsive hydrogel incorporated with dental follicle stem cell-derived small extracellular vesicles promotes dental pulp repair by ameliorating oxidative stress.Bioact Mater. 2024 Jul 5;36:524-540. doi: 10.1016/j.bioactmat.2024.06.036. eCollection 2024 Jun. Bioact Mater. 2024. PMID: 39072284 Free PMC article.
-
Potential application of dental stem cells in regenerative reconstruction of oral and maxillofacial tissues: a narrative review.Front Oral Maxillofac Med. 2022 Jun;4:14. doi: 10.21037/fomm-21-10. Epub 2022 Jun 10. Front Oral Maxillofac Med. 2022. PMID: 35813450 Free PMC article.
-
Expression of odontogenic ameloblast-associated protein in the dental follicle and its role in osteogenic differentiation of dental follicle stem cells.Arch Oral Biol. 2017 Jun;78:6-12. doi: 10.1016/j.archoralbio.2017.02.001. Epub 2017 Feb 5. Arch Oral Biol. 2017. PMID: 28189884 Free PMC article.
References
-
- Mitchell D. An introduction to oral and maxillofacial surgery. 4th ed. Oxford University Press; Oxford: 2005.
-
- Nkenke E, Schultze-Mosgau S, Radespiel-Troger M, Kloss F, Neukam FW. Morbidity of harvesting of chin grafts: a prospective study. Clin Oral Implants Res. 2001;12:495–502. - PubMed
-
- Nkenke E, Radespiel-Troger M, Wiltfang J, Schultze-Mosgau S, Winkler G, Neukam FW. Morbidity of harvesting of retromolar bone grafts: a prospective study. Clin Oral Implants Res. 2002;13:514–21. - PubMed
-
- Cowan CM, Shi YY, Aalami OO, Chou YF, Mari C, Thomas R, et al. Adipose-derived adult stromal cells heal critical-size mouse calvarial defects. Nat Biotechnol. 2004;22:560–7. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

