Acetaminophen-induced Liver Injury: from Animal Models to Humans
- PMID: 26355817
- PMCID: PMC4521247
- DOI: 10.14218/JCTH.2014.00014
Acetaminophen-induced Liver Injury: from Animal Models to Humans
Abstract
Drug-induced liver injury is an important clinical problem and a challenge for drug development. Whereas progress in understanding rare and unpredictable (idiosyncratic) drug hepatotoxicity is severely hampered by the lack of relevant animal models, enormous insight has been gained in the area of predictable hepatotoxins, in particular acetaminophen-induced liver injury, from a broad range of experimental models. Importantly, mechanisms of toxicity obtained with certain experimental systems, such as in vivo mouse models, primary mouse hepatocytes, and metabolically competent cell lines, are being confirmed in translational studies in patients and in primary human hepatocytes. Despite this progress, suboptimal models are still being used and experimental data can be confusing, leading to controversial conclusions. Therefore, this review attempts to discuss mechanisms of drug hepatotoxicity using the most studied drug acetaminophen as an example. We compare the various experimental models that are used to investigate mechanisms of acetaminophen hepatotoxicity, discuss controversial topics in the mechanisms, and assess how these experimental findings can be translated to the clinic. The success with acetaminophen in demonstrating the clinical relevance of experimental findings could serve as an example for the study of other drug toxicities.
Keywords: Drug hepatotoxicity; Necrosis; Sterile inflammation; Translational studies.
Conflict of interest statement
Figures
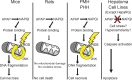
References
-
- Kaplowitz N. Idiosyncratic drug hepatotoxicity. Nat Rev Drug Discov. 2005;4:489–499. 10.1038/nrd1750. - DOI - PubMed
-
- Fontana RJ. Pathogenesis of idiosyncratic drug-induced liver injury and clinical perspectives. Gastroenterology. 2014;146:914–928. 10.1053/j.gastro.2013.12.032. - DOI - PMC - PubMed
-
- Uetrecht J, Naisbitt DJ. Idiosyncratic adverse drug reactions: current concepts. Pharmacol Rev. 2013;65:779–808. 10.1124/pr.113.007450. - DOI - PMC - PubMed
-
- Urban TJ, Shen Y, Stolz A, Chalasani N, Fontana RJ, Rochon J, et al. Limited contribution of common genetic variants to risk for liver injury due to a variety of drugs. Pharmacogenet Genomics. 2012;22:784–795. 10.1097/FPC.0b013e3283589a76. - DOI - PMC - PubMed
-
- Budnitz DS, Lovegrove MC, Crosby AE. Emergency department visits for overdoses of acetaminophen-containing products. Am J Prev Med. 2011;40:585–592. 10.1016/j.amepre.2011.02.026. - DOI - PubMed
Publication types
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
