Is Transient Ischemic Attack a Medical Emergency? An Evidence-Based Analysis
- PMID: 26355823
- PMCID: PMC4558772
Is Transient Ischemic Attack a Medical Emergency? An Evidence-Based Analysis
Abstract
Background: Transient ischemic attack (TIA) is a brief episode of dysfunction in a confined area of the brain. The risk of stroke following TIA is approximately 4% within the first 2 days and 9% within the first month. Therefore, early diagnosis and treatment is critical to reduce mortality and risk of stroke in patients who have experienced a TIA.
Objectives: This systematic review aimed to investigate the impact of the urgent evaluation and initiation of treatment of patients with TIA on the risk of subsequent stroke and death.
Data sources: A literature search was performed for studies published from January 1, 2007, until December 21, 2012. The search was updated monthly to April 1, 2013.
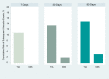
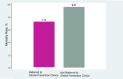
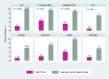
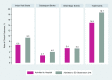
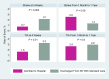
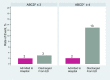
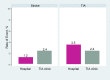
Results: All identified studies showed that urgent assessment and initiation of treatment of TIA is an effective strategy in reducing the incidence of stroke. Among these, a large observational study found a large effect in that the risk of stroke was reduced by 80%, and a Canadian study found that providing urgent care significantly reduced the rate of stroke in high-risk patients. Another Canadian study reported a significant reduction in the rate of death among patients referred to stroke prevention clinics, compared to patients not referred to such services. One study showed that patients discharged from an emergency department with standard care had significantly higher rates of stroke and subsequent TIA in the first month, compared to those who were hospitalized. However, another study showed that for patients at low to moderate risk, rate of stroke was similar between inpatients and those managed in a TIA clinic.
Limitations: Our analysis was restricted to the effect of the combined interventions. The magnitude of benefit of each individual component of the intervention cannot be determined through this review.
Conclusions: The results of this systematic review have important clinical and health system implications. Urgent management of TIA patients in specialized TIA clinics rather than regular practice results in a lower rate of stroke and disability.
Figures

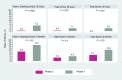
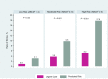
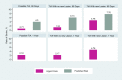
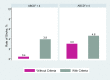

Similar articles
-
Home treatment for mental health problems: a systematic review.Health Technol Assess. 2001;5(15):1-139. doi: 10.3310/hta5150. Health Technol Assess. 2001. PMID: 11532236
-
A Current Estimation of the Early Risk of Stroke after Transient Ischemic Attack: A Systematic Review and Meta-Analysis of Recent Intervention Studies.Cerebrovasc Dis. 2017;43(1-2):90-98. doi: 10.1159/000452978. Epub 2016 Dec 20. Cerebrovasc Dis. 2017. PMID: 27992865
-
Sertindole for schizophrenia.Cochrane Database Syst Rev. 2005 Jul 20;2005(3):CD001715. doi: 10.1002/14651858.CD001715.pub2. Cochrane Database Syst Rev. 2005. PMID: 16034864 Free PMC article.
-
Sexual Harassment and Prevention Training.2024 Mar 29. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan–. 2024 Mar 29. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan–. PMID: 36508513 Free Books & Documents.
-
Systemic pharmacological treatments for chronic plaque psoriasis: a network meta-analysis.Cochrane Database Syst Rev. 2021 Apr 19;4(4):CD011535. doi: 10.1002/14651858.CD011535.pub4. Cochrane Database Syst Rev. 2021. Update in: Cochrane Database Syst Rev. 2022 May 23;5:CD011535. doi: 10.1002/14651858.CD011535.pub5. PMID: 33871055 Free PMC article. Updated.
Cited by
-
Ischemic stroke recurrence and mortality in different imaging phenotypes of ischemic cerebrovascular disease: The SMART-MR Study.Eur Stroke J. 2023 Jun;8(2):522-531. doi: 10.1177/23969873231162122. Epub 2023 Mar 10. Eur Stroke J. 2023. PMID: 37231699 Free PMC article.
-
Age-Related Differences in Non-Persistence with Statin Treatment in Patients after a Transient Ischaemic Attack.Clin Drug Investig. 2017 Nov;37(11):1047-1054. doi: 10.1007/s40261-017-0559-3. Clin Drug Investig. 2017. PMID: 28791591
-
Patients' anticipated actions following transient ischaemic attack symptoms: a qualitative vignette-based study.BMC Fam Pract. 2017 Feb 3;18(1):14. doi: 10.1186/s12875-017-0594-4. BMC Fam Pract. 2017. PMID: 28158992 Free PMC article.
-
Imaging Diagnosis of Transient Ischemic Attack in Clinic and Traditional Chinese Medicine.Biomed Res Int. 2019 Feb 17;2019:5094842. doi: 10.1155/2019/5094842. eCollection 2019. Biomed Res Int. 2019. PMID: 30906774 Free PMC article. Review.
-
From Inpatient to Ambulatory Care: The Introduction of a Rapid Access Transient Ischaemic Attack Service.Healthcare (Basel). 2018 Jun 1;6(2):57. doi: 10.3390/healthcare6020057. Healthcare (Basel). 2018. PMID: 29865148 Free PMC article.
References
-
- Johnston SC, Rothwell PM, Nguyen-Huynh MN, Giles MF, Elkins JS, Bernstein AL, et al. Validation and refinement of scores to predict very early stroke risk after transient ischaemic attack. Lancet. 2007. Jan 27; 369 (9558):283–92. - PubMed
-
- Gorelick PB. The burden and management of TIA and stroke in government-funded healthcare programs. Am J Manag Care. 2009. Jun; 15 (6 Suppl): S177–S184. - PubMed
-
- Kapral MK, Hall R, Stamplecoski M, Meyer S, Asllani E, Fang J, Richards J, O'Callaghan C, Silver FL. Registry of the Canadian Stroke Network – report on the 2008/09 Ontario Stroke Audit [Internet]. Toronto, ON: Institute for Clinical Evaluative Sciences; 2011. [cited: 2014 Dec 18]. 4 p. Available from: http://ontariostrokenetwork.ca/pdf/ICES_Stroke_Report_Final_2011_March.pdf
-
- Guidelines and protocols advisory committee. Stroke and transient ischemic attack management and prevention [Internet]. Vancouver, BC: British Columbia Medical Association, Joint publication of the British Columbia Ministry of Health; 2012. Apr 29 [cited: 2012 Nov]. 8 p. Available from: http://www.bcguidelines.ca/pdf/stroke.pdf
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous
