Ex situ reimplantation technique, in central lung tumors
- PMID: 26366395
- PMCID: PMC4543329
- DOI: 10.3978/j.issn.2305-5839.2015.08.03
Ex situ reimplantation technique, in central lung tumors
Abstract
Background: The parenchyma-sparing resection is most often performed in patients with impaired preoperative lung or cardiovascular function who would not be able to tolerate a pneumonectomy.
Methods: Our experience on the ex situ reimplantation procedure and the outcome of patients with lung malignancies, who underwent upper or upper-middle lobectomy, with reimplantation of the lower lobe was reported.
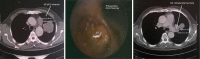
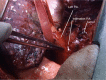
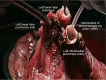
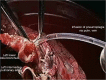
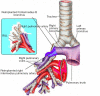
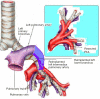
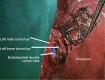
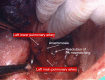
Results: We present 9 patients mean age 62.6+16.2 years (7 males/2 females) underwent ex situ reimplantation due to extensive lung tumor of upper lobes. The surgical technique precludes IV heparinization and then radical pneumonectomy. The entire lung was immersed in Ringer's solution (temperature 4 degrees centigrade) and bench surgery was performed. The involved upper (or upper-middle) lobes with involved lymph nodes were resected, thus leaving the healthy lower lobe of the lung. Pneumoplegia solution, named "Papworth pneumoplegia", was administered (1,473 mL) through catheterization of the pulmonary artery and vein stumps (ante grade and retrograde) along with 250 mL of prostaglandin E1. Re-implantation of the lower lobe was performed (I) on the right side, implantation involved the anastomosis of lower pulmonary vein in the site of the cuff of left atrium, followed by suturing the stump of the intermedius pulmonary artery to the right main pulmonary artery and finally the bronchial stumps-intermedius bronchus to the right main bronchus; (II) on the left side the pulmonary vein was anastomosed first, followed by the bronchial stumps and finally by the pulmonary artery. The graft ischemia time was 70.2+8.4 minutes ranged between 55 and 80 minutes.
Conclusions: Re-implantation or auto-transplantation should be considered as a safe option for the appropriate patient with lung cancer. The ex situ separation of the cancerous lobes is technically feasible and allows extensive pulmonary resection while minimizing the loss of pulmonary reserve. Based on our work, the major factors that play a role for the survival of initially resected and then re-implanted lung graft, are: (I) the ischemia time of the re-implanted lobe; (II) the proper use of pneumoplegia solutions, along with prostaglandin E1 and heparin; (III) the occurrence of pulmonary vein thrombosis; and (IV) the bronchial anastomosis.
Keywords: Non-small lung cancer; auto-transplantation; bench surgery; ex situ; re-implantation.
Conflict of interest statement
Figures
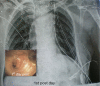
Similar articles
-
Operation for preservation of lung parenchyma in central lung cancer--in vivo and ex situ reimplantation techniques.Anticancer Res. 2015 Mar;35(3):1675-81. Anticancer Res. 2015. PMID: 25750327
-
Extended sleeve lobectomy: one more step toward avoiding pneumonectomy in centrally located lung cancer.Ann Thorac Surg. 2013 Dec;96(6):1988-97. doi: 10.1016/j.athoracsur.2013.07.011. Epub 2013 Sep 12. Ann Thorac Surg. 2013. PMID: 24035301
-
Lung autotransplantation technique in the treatment for central lung cancer of upper lobe.J Thorac Oncol. 2008 Jun;3(6):609-11. doi: 10.1097/JTO.0b013e31817589a8. J Thorac Oncol. 2008. PMID: 18520799
-
International expert consensus on the management of bleeding during VATS lung surgery.Ann Transl Med. 2019 Dec;7(23):712. doi: 10.21037/atm.2019.11.142. Ann Transl Med. 2019. PMID: 32042728 Free PMC article. Review.
-
[The indications of bronchial resection and anastomosis in lung cancer].Pneumologia. 2001 Apr-Jun;50(2):109-14. Pneumologia. 2001. PMID: 11584670 Review. Romanian.
Cited by
-
Right basilar segmental autologous lung transplantation with carinal reconstruction in a patient with central lung squamous cell carcinoma: Case report.JTCVS Tech. 2025 May 15;32:198-200. doi: 10.1016/j.xjtc.2025.04.021. eCollection 2025 Aug. JTCVS Tech. 2025. PMID: 40814674 Free PMC article. No abstract available.
-
Neoadjuvant immunochemotherapy followed by ex situ lung auto-transplant (Oto procedure) for central lung cancer: A case report with literature review.Respirol Case Rep. 2024 Oct 11;12(10):e70045. doi: 10.1002/rcr2.70045. eCollection 2024 Oct. Respirol Case Rep. 2024. PMID: 39398253 Free PMC article.
-
Extended resections for the treatment of patients with T4 stage IIIA non-small cell lung cancer (NSCLC) (T4N0-1M0) with or without cardiopulmonary bypass: a 15-year two-center experience.J Thorac Dis. 2019 Dec;11(12):5489-5501. doi: 10.21037/jtd.2019.11.33. J Thorac Dis. 2019. PMID: 32030268 Free PMC article.
References
-
- Pearson FG, Cooper JD, Deslauriers J, et al, editors. Thoracic surgery 2nd ed. New York: Churchill Livingstone 2002:837-47.
-
- Tedder M, Anstadt MP, Tedder SD, et al. Current morbidity, mortality, and survival after bronchoplastic procedures for malignancy. Ann Thorac Surg 1992;54:387-91. - PubMed
-
- Venuta F, Rendina EA, Bufi M, et al. Preimplantation retrograde pneumoplegia in clinical lung transplantation. J Thorac Cardiovasc Surg 1999;118:107-14. - PubMed
-
- Martin-Ucar AE, Chaudhuri N, Edwards JG, et al. Can pneumonectomy for non-small cell lung cancer be avoided? An audit of parenchymal sparing lung surgery. Eur J Cardiothorac Surg 2002;21:601-5. - PubMed
-
- de Perrot M, Liu M, Waddell TK, et al. Ischemia-reperfusion-induced lung injury. Am J Respir Crit Care Med 2003;167:490-511. - PubMed
LinkOut - more resources
Full Text Sources
