Hypothetical Atopic Dermatitis-Myeloproliferative Neoplasm Syndrome
- PMID: 26379670
- PMCID: PMC4547498
- DOI: 10.3389/fimmu.2015.00434
Hypothetical Atopic Dermatitis-Myeloproliferative Neoplasm Syndrome
Abstract
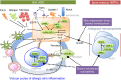
Atopic dermatitis (AD) is a chronic inflammatory skin disease. Myeloproliferative neoplasms (MPNs) are hematopoietic malignancies caused by uncontrolled proliferation of hematopoietic stem/progenitor cells. Recent studies have described several mutant mice exhibiting both AD-like skin inflammation and MPN. Common pathways for skin inflammation encompass overexpression of thymic stromal lymphopoietin and reduced signaling of epidermal growth factor receptor in the epidermis, while overproduction of granulocyte-colony-stimulating factor by keratinocytes and constitutive activation of Stat5 in hematopoietic stem cells are important for the development of MPN. The murine studies suggest the existence of a similar human disease tentatively termed as the atopic dermatitis-myeloproliferative neoplasm syndrome.
Keywords: atopic dermatitis; hematopoietic stem cell; mast cell; mouse models; myeloproliferative neoplasm.
Figures
Similar articles
-
Atopic dermatitis-like disease and associated lethal myeloproliferative disorder arise from loss of Notch signaling in the murine skin.PLoS One. 2010 Feb 18;5(2):e9258. doi: 10.1371/journal.pone.0009258. PLoS One. 2010. PMID: 20174635 Free PMC article.
-
Dysregulated activation of activator protein 1 in keratinocytes of atopic dermatitis patients with enhanced expression of granulocyte/macrophage-colony stimulating factor.J Invest Dermatol. 2000 Dec;115(6):1134-43. doi: 10.1046/j.1523-1747.2000.00149.x. J Invest Dermatol. 2000. PMID: 11121152
-
Requirement of MyD88 signaling in keratinocytes for Langerhans cell migration and initiation of atopic dermatitis-like symptoms in mice.Eur J Immunol. 2016 Apr;46(4):981-92. doi: 10.1002/eji.201545710. Epub 2016 Jan 18. Eur J Immunol. 2016. PMID: 26694221
-
The contribution of keratinocytes to the pathogenesis of atopic dermatitis.Eur J Dermatol. 2006 Mar-Apr;16(2):125-31. Eur J Dermatol. 2006. PMID: 16581561 Review.
-
Cellular and molecular mechanisms in atopic dermatitis.Adv Immunol. 2009;102:135-226. doi: 10.1016/S0065-2776(09)01203-6. Adv Immunol. 2009. PMID: 19477321 Review.
Cited by
-
Primary atopic disorders.J Exp Med. 2018 Apr 2;215(4):1009-1022. doi: 10.1084/jem.20172306. Epub 2018 Mar 16. J Exp Med. 2018. PMID: 29549114 Free PMC article. Review.
References
Publication types
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials
Miscellaneous

