Gestational diabetes among Saudi women: prevalence, risk factors and pregnancy outcomes
- PMID: 26409797
- PMCID: PMC6074454
- DOI: 10.5144/0256-4947.2015.222
Gestational diabetes among Saudi women: prevalence, risk factors and pregnancy outcomes
Abstract
Background and objectives: The prevalence of gestational diabetes (GDM) has increased recently worldwide, mainly due to adoption of the International Association of Diabetes and Pregnancy Study Group (IADPSG) criteria. The objectives of this study were to determine the prevalence of GDM in Saudi women and to assess risk factors and pregnancy outcomes using the IADPSG criteria.
Design and setting: A prospective descriptive study of pregnant Saudi women presenting at the Maternity and Children Hospital, Medina, Saudi Arabia, between October 2011 and June 2014.
Methods: Fasting plasma glucose, glycated hemoglobin, and random plasma glucose concentrations were obtained for all participants at the first antenatal visit. In women with normal results, screening for GDM was performed at 24 to 28 weeks of gestation, with a 75-g oral glucose tolerance test (OGTT). Women who had GDM were treated with diet, exercise, and insulin as needed. Pregnancy outcomes were recorded after delivery. Multiple logistic regression was used to assess possible risk factors for GDM.
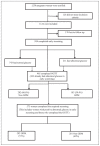
Results: Early screenings showed abnormal glucose in 211 of 954 women (22.1%). In 445 women, the OGTT showed GDM in 183 women (39.4%). GDM cases identified by OGTT and by early screening increased the rate of GDM to 51% (292 women). Older maternal age, higher body mass index, higher blood pressure, past GDM, history of delivering a malformed child, and family history of diabetes were the main risk factors for GDM. GDM increased the risk of neonatal hypoglycemia (OR 9.353), low Apgar score (OR 5.546), and induction of labor (OR 2.33). The newborns of GDM mothers had a higher birth weight: 3043 g vs. 2890 g in the non-GDM group (P=.004). Other maternal and neonatal outcomes were not significantly different between the two groups.
Conclusion: The prevalence of GDM is high among Saudi women. Timely and effective treatment reduces perinatal morbidity and improves outcomes.
Conflict of interest statement
The author has no conflicts of interest.
Figures
References
-
- Metzger BE, Coustan DR. Summary and recommendations of the Fourth International Workshop-Conference on Gestational Diabetes Mellitus. The Organizing Committee. Diabetes care. 1998;21:B161. - PubMed
-
- Bevier WC, Jovanovic-Peterson L, Peterson CM. Pancreatic disorders of pregnancy. Diagnosis, management, and outcome of gestational diabetes. Endocrinology and metabolism clinics of North America. 1995;24(1):103–38. - PubMed
-
- Jovanovic L, Pettitt DJ. Gestational diabetes mellitus. JAMA: the journal of the American Medical Association. 2001;286(20):2516–8. - PubMed
-
- Association AAD. Gestational diabetes mellitus. Diabetes Care. 2004;27(1):s88–s90. - PubMed
-
- Lapolla A, Dalfrà M, Ragazzi E, De Cata A, Fedele D. New International Association of the Diabetes and Pregnancy Study Groups (IADPSG) recommendations for diagnosing gestational diabetes compared with former criteria: a retrospective study on pregnancy outcome. Diabetic Medicine. 2011;28(9):1074–7. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous