Laparoscopic single-incision gastric bypass: initial experience, technique and short-term outcomes
- PMID: 26473005
- PMCID: PMC4606897
- DOI: 10.1186/s13022-015-0016-z
Laparoscopic single-incision gastric bypass: initial experience, technique and short-term outcomes
Abstract
Background: Single incision laparoscopic surgery (SILS) research has been limited. The aim of this study is to describe our technique and to evaluate the short term outcomes and efficacy of SILS Roux-en-Y gastric bypass (RYGB) in a selected group of patients in a single center.
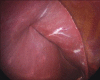
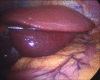
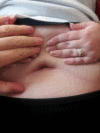
Methods: From March 2012 to January 2013, a total of fourteen patients underwent SILS RYGB using a single vertical 2.5-3 cm intra-umbilical incision, 3-ports placed trans-fascially, and a liver suspension technique in Cleveland Clinic's Bariatric & Metabolic Institute, in Cleveland, Ohio, USA. Patient selection, short-term outcomes and technical issues were retrospectively viewed in this study.
Results: A total of 14 morbid obese patients (12 women and 2 men; mean age, 46 years). Mean operative time was 196 (range 131-265) min. Mean weight at surgery was 113 (range 91-135) kg. One patient required placement of one additional port (7 %). No conversions to conventional laparoscopic surgery (CLS) or open surgery was needed. The estimated blood loss was 40 (range 20-100) ml. In terms of pain control, the frequency of patient controlled analgesia had a mean use of 21 times in postoperative day 0 (POD), 37 times in POD1 and 13 times in POD2. Pain score (assessed by visual analogue scale) had a median score of 6.9 in POD0, 5.2 In POD1 and 3.8 in POD2. Weight loss was approximately 7.25 lb. (±4.5) after first postoperative visit, 28.9 lb. (±11.86) after 1 month and 45.4 lb. (±15.4) after 4 months. No patients required re-operation or readmission during the 90 days after surgery.
Conclusion: Single incision is feasible, safe and reproducible technique used as an access to complex surgeries like gastric bypass in carefully selected patients. Results in short-term outcomes are comparable to those observed in literature. Some potential benefits include less postoperative pain, improved cosmesis, and patient satisfaction. Randomized trials involving larger patient series with a longer follow-up and larger cohort studies and/or systematic reviews will be necessary to assess the extent of the benefits and limitations of SILS in bariatric surgery.
Keywords: Bariatric surgery; Cosmesis; Morbid obesity; Post-operative Pain; Single incision gastric bypass; Single incision laparoscopic surgery.
Figures
References
-
- Reoch J, Mottillo S, Shimony A, et al. Safety of laparoscopic vs open bariatric surgery: A systematic review and meta-analysis. Arch Surg. 2011;146:1314–22. - PubMed
-
- Huang C-K, Lo C-H, Houng J-Y, Chen, Y-S, Lee P-H. Surgical results of single-incision transumbilical laparoscopic Roux-en-Y gastric bypass.Surg Obes Relat Dis. 2012;8:201–7. - PubMed
-
- Hawker GA, Mian S, Kendzerska T, French M. Measures of adult pain: Visual Analog Scale for Pain (VAS Pain), Numeric Rating Scale for Pain (NRS Pain), McGill Pain Questionnaire (MPQ), Short-Form McGill Pain Questionnaire (SF-MPQ), Chronic Pain Grade Scale (CPGS), Short Form-36 Bodily Pain Scale (SF-36 BPS), and Measure of Intermittent and Constant Osteoarthritis Pain (ICOAP). Arthritis Care Res (Hoboken). 2011;63 Suppl 11: S240–52. - PubMed
-
- Mittermair R, Pratschke J, Sucher R. Single-incision laparoscopic sleeve gastrectomy. Am Surg. 2013;79:393–397. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials