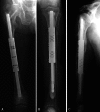
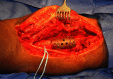
Outcomes of a Modular Intercalary Endoprosthesis as Treatment for Segmental Defects of the Femur, Tibia, and Humerus
- PMID: 26475032
- PMCID: PMC4709281
- DOI: 10.1007/s11999-015-4588-z
Outcomes of a Modular Intercalary Endoprosthesis as Treatment for Segmental Defects of the Femur, Tibia, and Humerus
Abstract
Background: Resection of diaphyseal bone tumors for local tumor control and stabilization often results in an intercalary skeletal defect and presents a reconstructive challenge for orthopaedic surgeons. Although many options for reconstruction have been described, relatively few studies report on the functional outcomes and complications of patients treated with modular intercalary endoprostheses.
Questions/purposes: The objectives of this study were to examine clinical outcomes after reconstruction with a modular intercalary endoprosthesis with a specific focus on (1) the rate of complication or failure; (2) differences in complication rates by anatomic site; (3) functional results as assessed by the Musculoskeletal Tumor Society System (MSTS); and (4) differences in complication rate between patients treated with cemented versus noncemented fixation.
Methods: We conducted a retrospective chart review of patients treated with a modular intercalary endoprosthesis from three musculoskeletal oncology centers from 2008 to 2013. The indication for use of this intercalary endoprosthesis was segmental bone loss from aggressive or malignant tumor with sparing of the joint above and below and deemed unsuitable for biologic reconstruction. No other implant was used for this indication during this period. During this period, 41 patients received a total of 44 intercalary implants, which included 18 (40%) humeri, 5 (11%) tibiae, and 21 (48%) femora. There were 27 (66%) men and 14 (34%) women with a mean age of 63 years (range, 18–91 years). Eight patients (20%) had primary bone tumors and 33 (80%) had metastatic lesions. Thirty-five (85%) patients were being operated on as an initial treatment and six (15%) for revision of a previous reconstruction. Twenty-nine (66%) procedures had cemented stem fixation and 15 (34%) were treated with noncemented fixation. The overall mean followup was 14 months (range, 1–51 months). Patients with primary tumors had a mean followup of 19 months (range, 4–48 months) and patients with metastatic disease had a mean followup of 11 months (range, 1–51 months). Causes of implant failure were categorized according to Henderson et al. [19] into five types as follows: Type I (soft tissue failure), Type II (aseptic loosening), Type III (structural failure), Type IV (infection), and Type V (tumor progression). At 2 years of followup, 38 (93%) of these patients were accounted for with three (7%) lost to followup. MSTS functional assessment was available for 39 of 41 patients (95%).
Results: At latest followup of these 41 patients, 14 (34%) patients were dead of disease, two patients (5%) dead of other causes, seven (17%) are continuously disease-free, one (2%) shows no evidence of disease, and 17 (41%) are alive with disease. There were 12 (27%) nononcologic complications. Five (11%) of these were Type II failures occurring in noncemented implants between the stem and bone, and six (14%) were Type III failures occurring in cemented implants at the clamp-rod implant interface. One patient developed a deep infection (2%, Type IV failure) and underwent removal of the implant. Additionally, one patient (2%, Type V failure) was treated by amputation after local progression of his metastatic disease. Complications were more common in femoral reconstructions than in tibial or humeral reconstructions. Twelve of 21 patients (57%) with femoral reconstructions had complications versus 0% of tibial or humeral reconstructions (0 of 23; odds ratio [OR], 62; 95% confidence interval [CI], 3–1154; p < 0.0001). The mean overall MSTS score was 77%. Implants with cemented fixation (29) had higher mean MSTS scores when compared with implants with noncemented (15) fixation (84% versus 66%, p = 0.0017). The complication rate was 33% in noncemented cases and 21% in cemented cases (p = 0.39); however, Type II failure at the bone-stem interface was associated with noncemented fixation and Type III failure at the clamp-rod interface was associated with cemented fixation (OR, 143; 95% CI, 2.413–8476; p = 0.0022).
Conclusions: The results of this study indicate that this modular intercalary endoprosthesis yields equivalent results to other studies of intercalary endoprostheses in terms of MSTS scores. We found that patients treated with intercalary endoprostheses in the femur experienced more frequent complications than those treated for lesions in either the humerus or tibia and that the femoral complication rate of this endoprosthesis is higher when compared with other studies of intercalary endoprostheses for femoral reconstruction. Further studies are still needed to determine the long-term outcomes of this endoprosthesis in patients with primary tumors where longevity of the implant is of more importance than in the metastatic setting. We recommend cemented fixation for this intercalary modular endoprostheses because this provides improved MSTS scores and allows immediate return to weightbearing, which is of advantage to metastatic patients with limited lifespans. Level of Evidence: Level III, therapeutic study.
Figures
Comment in
-
CORR Insights(®): Outcomes of a Modular Intercalary Endoprosthesis as Treatment for Segmental Defects of the Femur, Tibia, and Humerus.Clin Orthop Relat Res. 2016 Feb;474(2):549-50. doi: 10.1007/s11999-015-4635-9. Epub 2015 Nov 19. Clin Orthop Relat Res. 2016. PMID: 26584801 Free PMC article. No abstract available.
Similar articles
-
Do Massive Allograft Reconstructions for Tumors of the Femur and Tibia Survive 10 or More Years after Implantation?Clin Orthop Relat Res. 2020 Mar;478(3):517-524. doi: 10.1097/CORR.0000000000000806. Clin Orthop Relat Res. 2020. PMID: 32168064 Free PMC article.
-
What Are the Long-term Results of MUTARS® Modular Endoprostheses for Reconstruction of Tumor Resection of the Distal Femur and Proximal Tibia?Clin Orthop Relat Res. 2017 Mar;475(3):708-718. doi: 10.1007/s11999-015-4644-8. Clin Orthop Relat Res. 2017. PMID: 26649558 Free PMC article.
-
Are Complications Associated With the Repiphysis(®) Expandable Distal Femoral Prosthesis Acceptable for Its Continued Use?Clin Orthop Relat Res. 2015 Sep;473(9):3003-13. doi: 10.1007/s11999-015-4355-1. Epub 2015 May 21. Clin Orthop Relat Res. 2015. PMID: 25995179 Free PMC article.
-
Causes and Frequencies of Reoperations After Endoprosthetic Reconstructions for Extremity Tumor Surgery: A Systematic Review.Clin Orthop Relat Res. 2019 Apr;477(4):894-902. doi: 10.1097/CORR.0000000000000630. Clin Orthop Relat Res. 2019. PMID: 30801278 Free PMC article.
-
Proximal Tibial Reconstruction After Tumor Resection: A Systematic Review of the Literature.JBJS Rev. 2019 Jul;7(7):e1. doi: 10.2106/JBJS.RVW.18.00146. JBJS Rev. 2019. PMID: 31268862
Cited by
-
Three-dimensional-printed porous prosthesis for the joint-sparing reconstruction of the proximal humeral tumorous defect.Front Bioeng Biotechnol. 2023 Jan 12;10:1098973. doi: 10.3389/fbioe.2022.1098973. eCollection 2022. Front Bioeng Biotechnol. 2023. PMID: 36714618 Free PMC article.
-
Intercalary Prosthetic Reconstruction with Three-Dimensional-Printed Custom-Made Porous Component for Defects of Long Bones with Short Residual Bone Segments After Tumor Resection.Orthop Surg. 2024 Feb;16(2):374-382. doi: 10.1111/os.13969. Epub 2023 Dec 18. Orthop Surg. 2024. PMID: 38111053 Free PMC article.
-
Is three-dimensional-printed custom-made ultra-short stem with a porous structure an acceptable reconstructive alternative in peri-knee metaphysis for the tumorous bone defect?World J Surg Oncol. 2021 Aug 8;19(1):235. doi: 10.1186/s12957-021-02355-7. World J Surg Oncol. 2021. PMID: 34365976 Free PMC article.
-
Ultra-short stem intercalary prosthetic reconstruction for joint preservation in metaphyseal tumor management: a retrospective review of twenty-five cases.BMC Musculoskelet Disord. 2025 May 24;26(1):513. doi: 10.1186/s12891-025-08780-z. BMC Musculoskelet Disord. 2025. PMID: 40413518 Free PMC article.
-
Intercalary Diaphyseal Endoprosthetic Reconstruction.J Am Acad Orthop Surg Glob Res Rev. 2025 Jul 2;9(7):e24.00201. doi: 10.5435/JAAOSGlobal-D-24-00201. eCollection 2025 Jul 1. J Am Acad Orthop Surg Glob Res Rev. 2025. PMID: 40591808 Free PMC article. Review.
References
-
- Abudu A, Carter SR, Grimer RJ. The outcome and functional results of diaphyseal endoprostheses after tumour excision. J Bone Joint Surg Br. 1996;78:652–657. - PubMed
-
- Alman BA, De Bari A, Krajbich JI. Massive allografts in the treatment of osteosarcoma and Ewing sarcoma in children and adolescents. J Bone Joint Surg Am. 1995;77:54–64. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical