Clinical evaluation of a model-updated image-guidance approach to brain shift compensation: experience in 16 cases
- PMID: 26476637
- PMCID: PMC4834281
- DOI: 10.1007/s11548-015-1295-x
Clinical evaluation of a model-updated image-guidance approach to brain shift compensation: experience in 16 cases
Abstract
Purpose: Brain shift during neurosurgical procedures must be corrected for in order to reestablish accurate alignment for successful image-guided tumor resection. Sparse-data-driven biomechanical models that predict physiological brain shift by accounting for typical deformation-inducing events such as cerebrospinal fluid drainage, hyperosmotic drugs, swelling, retraction, resection, and tumor cavity collapse are an inexpensive solution. This study evaluated the robustness and accuracy of a biomechanical model-based brain shift correction system to assist with tumor resection surgery in 16 clinical cases.
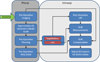
Methods: Preoperative computation involved the generation of a patient-specific finite element model of the brain and creation of an atlas of brain deformation solutions calculated using a distribution of boundary and deformation-inducing forcing conditions (e.g., sag, tissue contraction, and tissue swelling). The optimum brain shift solution was determined using an inverse problem approach which linearly combines solutions from the atlas to match the cortical surface deformation data collected intraoperatively. The computed deformations were then used to update the preoperative images for all 16 patients.
Results: The mean brain shift measured ranged on average from 2.5 to 21.3 mm, and the biomechanical model-based correction system managed to account for the bulk of the brain shift, producing a mean corrected error ranging on average from 0.7 to 4.0 mm.
Conclusions: Biomechanical models are an inexpensive means to assist intervention via correction for brain deformations that can compromise surgical navigation systems. To our knowledge, this study represents the most comprehensive clinical evaluation of a deformation correction pipeline for image-guided neurosurgery.
Keywords: Biomechanical model; Brain shift; Finite element; Image-guided surgery; Inverse model; Registration.
Conflict of interest statement
Figures


Similar articles
-
A comparison of thin-plate spline deformation and finite element modeling to compensate for brain shift during tumor resection.Int J Comput Assist Radiol Surg. 2020 Jan;15(1):75-85. doi: 10.1007/s11548-019-02057-2. Epub 2019 Aug 23. Int J Comput Assist Radiol Surg. 2020. PMID: 31444624 Free PMC article.
-
Brain-shift compensation using intraoperative ultrasound and constraint-based biomechanical simulation.Med Image Anal. 2017 Aug;40:133-153. doi: 10.1016/j.media.2017.06.003. Epub 2017 Jun 15. Med Image Anal. 2017. PMID: 28651099
-
Evaluation of conoscopic holography for estimating tumor resection cavities in model-based image-guided neurosurgery.IEEE Trans Biomed Eng. 2014 Jun;61(6):1833-43. doi: 10.1109/TBME.2014.2308299. IEEE Trans Biomed Eng. 2014. PMID: 24845293 Free PMC article.
-
IBIS: an OR ready open-source platform for image-guided neurosurgery.Int J Comput Assist Radiol Surg. 2017 Mar;12(3):363-378. doi: 10.1007/s11548-016-1478-0. Epub 2016 Aug 31. Int J Comput Assist Radiol Surg. 2017. PMID: 27581336 Review.
-
[Image-guided neurosurgery using intraoperative MRI].Brain Nerve. 2009 Jul;61(7):823-34. Brain Nerve. 2009. PMID: 19618860 Review. Japanese.
Cited by
-
A Minireview on Brain Models Simulating Geometrical, Physical, and Biochemical Properties of the Human Brain.Front Bioeng Biotechnol. 2022 Mar 28;10:818201. doi: 10.3389/fbioe.2022.818201. eCollection 2022. Front Bioeng Biotechnol. 2022. PMID: 35419353 Free PMC article. Review.
-
Accounting for Deformation in Deep Brain Stimulation Surgery With Models: Comparison to Interventional Magnetic Resonance Imaging.IEEE Trans Biomed Eng. 2020 Oct;67(10):2934-2944. doi: 10.1109/TBME.2020.2974102. Epub 2020 Feb 14. IEEE Trans Biomed Eng. 2020. PMID: 32078527 Free PMC article.
-
Intraoperative Imaging Modalities and Compensation for Brain Shift in Tumor Resection Surgery.Int J Biomed Imaging. 2017;2017:6028645. doi: 10.1155/2017/6028645. Epub 2017 Jun 5. Int J Biomed Imaging. 2017. PMID: 28676821 Free PMC article. Review.
-
SLIMBRAIN database: A multimodal image database of in vivo human brains for tumour detection.Sci Data. 2025 May 21;12(1):836. doi: 10.1038/s41597-025-04993-y. Sci Data. 2025. PMID: 40399336 Free PMC article.
-
Gesture-based registration correction using a mobile augmented reality image-guided neurosurgery system.Healthc Technol Lett. 2018 Sep 27;5(5):137-142. doi: 10.1049/htl.2018.5063. eCollection 2018 Oct. Healthc Technol Lett. 2018. PMID: 30800320 Free PMC article.
References
-
- Nabavi A, Black PM, Gering DT, Westin CF, Mehta V, Pergolizzi RS, Ferrant M, Warfield SK, Hata N, Schwartz RB, Wells WM, Kikinis R, Jolesz FA. Serial intraoperative magnetic resonance imaging of brain shift. Neurosurgery. 2001;48(4):787–797. - PubMed
-
- Roberts DW, Hartov A, Kennedy FE, Miga MI, Paulsen KD. Intraoperative brain shift and deformation: a quantitative analysis of cortical displacement in 28 cases. Neurosurgery. 1998;43(4):749–758. - PubMed
-
- Hill DLG, Maurer CR, Maciunas RJ, Barwise JA, Fitzpatrick JM, Wang MY. Measurement of intraoperative brain surface deformation under a craniotomy. Neurosurgery. 1998;43(3):514–526. - PubMed
-
- Maurer CR, Hill DLG, Martin AJ, Liu HY, McCue M, Rueckert D, Lloret D, Hall WA, Maxwell RE, Hawkes DJ, Truwit CL. Investigation of intraoperative brain deformation using a 1.5-t interventional MR system: preliminary results. IEEE Trans Med Imaging. 1998;17(5):817–825. - PubMed
-
- Nimsky C, Ganslandt O, Cerny S, Hastreiter P, Greiner G, Fahlbusch R. Quantification of visualization of, compensation for brain shift using intraoperative magnetic resonance imaging. Neurosurgery. 2000;47(5):1070–1079. - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

