Revisiting Unplanned Endotracheal Extubation and Disease Severity in Intensive Care Units
- PMID: 26484674
- PMCID: PMC4617893
- DOI: 10.1371/journal.pone.0139864
Revisiting Unplanned Endotracheal Extubation and Disease Severity in Intensive Care Units
Abstract
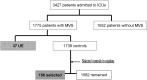
Most reports regarding unplanned extubation (UE) are case-control studies with matching age and disease severity. To avoid diminishing differences in matched factors, this study with only matching duration of mechanical ventilation aimed to re-examine the risk factors and the factors governing outcomes of UE in intensive care units (ICUs). This case-control study was conducted on 1,775 subjects intubated for mechanical ventilation. Thirty-seven (2.1%) subjects with UE were identified, and 156 non-UE subjects were randomly selected as the control group. Demographic data, acute Physiological and Chronic Health Evaluation II (APACHE II) scores, and outcomes of UE were compared between the two groups. Logistic regression analysis was used to identify the risk factors of UE. Milder disease, younger age, and higher Glasgow Coma Scale (GCS) scores with more frequently being physically restrained (all p<0.05) were related to UE. Logistic regression revealed that APACHE II score (odds ratio (OR) 0.91, p<0.01), respiratory infection (OR 0.24, p<0.01), physical restraint (OR 5.36, p<0.001), and certain specific diseases (OR 3.79-5.62, p<0.05) were related to UE. The UE patients had a lower ICU mortality rate (p<0.01) and a trend of lower in-hospital mortality rate (p = 0.08). Cox regression analysis revealed that in-hospital mortality was associated with APACHE II score, age, shock, and oxygen used, all of which were co-linear, but not UE. The results showed that milder disease with higher GCS scores thereby requiring a higher use of physical restraints were related to UE. Disease severity but not UE was associated with in-hospital mortality.
Conflict of interest statement
Figures
Similar articles
-
Complicated acute myocardial infarction requiring mechanical ventilation in the intensive care unit: prognostic factors of clinical outcome in a series of 157 patients.Crit Care Med. 2004 Jan;32(1):100-5. doi: 10.1097/01.CCM.0000098605.58349.76. Crit Care Med. 2004. PMID: 14707566
-
Prognostic factors and outcomes of unplanned extubation.Sci Rep. 2017 Aug 17;7(1):8636. doi: 10.1038/s41598-017-08867-1. Sci Rep. 2017. PMID: 28819204 Free PMC article.
-
Incidence and Risk Factors of Unplanned Extubation in Critically Ill Surgical Patients: The Multi-center Thai University-based Surgical Intensive Care Units Study (THAI-SICU Study).J Med Assoc Thai. 2016 Sep;99 Suppl 6:S153-S162. J Med Assoc Thai. 2016. PMID: 29906373
-
Factors associated with unplanned extubation in the Intensive Care Unit for adult patients: A systematic review and meta-analysis.Intensive Crit Care Nurs. 2018 Aug;47:62-68. doi: 10.1016/j.iccn.2018.03.008. Epub 2018 Apr 10. Intensive Crit Care Nurs. 2018. PMID: 29653888
-
Unplanned extubation in critically ill adults: clinical review.Nurs Crit Care. 2013 May;18(3):123-34. doi: 10.1111/j.1478-5153.2012.00542.x. Epub 2012 Nov 22. Nurs Crit Care. 2013. PMID: 23577947 Review.
Cited by
-
Self-Extubation in Patients with Traumatic Head Injury: Determinants, Complications, and Outcomes.Anesth Essays Res. 2019 Jul-Sep;13(3):589-595. doi: 10.4103/aer.AER_92_19. Anesth Essays Res. 2019. PMID: 31602083 Free PMC article.
-
The Japanese Clinical Practice Guidelines for Management of Sepsis and Septic Shock 2020 (J-SSCG 2020).Acute Med Surg. 2021 Aug 26;8(1):e659. doi: 10.1002/ams2.659. eCollection 2021 Jan-Dec. Acute Med Surg. 2021. PMID: 34484801 Free PMC article.
-
Prevention of unplanned endotracheal extubation in intensive care unit: An overview of systematic reviews.Nurs Open. 2023 Feb;10(2):392-403. doi: 10.1002/nop2.1317. Epub 2022 Aug 15. Nurs Open. 2023. PMID: 35971250 Free PMC article. Review.
-
The Japanese Clinical Practice Guidelines for Management of Sepsis and Septic Shock 2020 (J-SSCG 2020).J Intensive Care. 2021 Aug 25;9(1):53. doi: 10.1186/s40560-021-00555-7. J Intensive Care. 2021. PMID: 34433491 Free PMC article.
-
"Patient Comfort Can Be Sacrificed for Patient Safety"-Perception and Practice Reported by Critical Care Nurses Toward Physical Restraints: A Qualitative Descriptive Study.Front Med (Lausanne). 2021 Jul 23;8:573601. doi: 10.3389/fmed.2021.573601. eCollection 2021. Front Med (Lausanne). 2021. PMID: 34368171 Free PMC article.
References
-
- de Lassence A, Alberti C, Azoulay E, Le Miere E, Cheval C, Vincent F, et al. (2002) Impact of unplanned extubation and reintubation after weaning on nosocomial pneumonia risk in the intensive care unit: a prospective multicenter study. Anesthesiology 97: 148–156. - PubMed
-
- Atkins PM, Mion LC, Mendelson W, Palmer RM, Slomka J, Franko T (1997) Characteristics and outcomes of patients who self-extubate from ventilatory support: a case-control study. Chest 112: 1317–1323. - PubMed
-
- Boulain T (1998) Unplanned extubations in the adult intensive care unit: a prospective multicenter study. Association des Reanimateurs du Centre-Ouest. Am J Respir Crit Care Med 157: 1131–1137. - PubMed
-
- Chevron V, Menard JF, Richard JC, Girault C, Leroy J, Bonmarchand G (1998) Unplanned extubation: risk factors of development and predictive criteria for reintubation. Crit Care Med 26: 1049–1053. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical