Low Incidence of HIV-1C Acquired Drug Resistance 10 Years after Roll-Out of Antiretroviral Therapy in Ethiopia: A Prospective Cohort Study
- PMID: 26512902
- PMCID: PMC4626118
- DOI: 10.1371/journal.pone.0141318
Low Incidence of HIV-1C Acquired Drug Resistance 10 Years after Roll-Out of Antiretroviral Therapy in Ethiopia: A Prospective Cohort Study
Abstract
The emergence of HIV-1 drug resistance mutations has mainly been linked to the duration and composition of antiretroviral treatment (ART), as well as the level of adherence. This study reports the incidence and pattern of acquired antiretroviral drug resistance mutations and long-term outcomes of ART in a prospective cohort from Northwest Ethiopia. Two hundred and twenty HIV-1C infected treatment naïve patients were enrolled and 127 were followed-up for up to 38 months on ART. ART initiation and patients' monitoring was based on the WHO clinical and immunological parameters. HIV viral RNA measurement and drug resistance genotyping were done at baseline (N = 160) and after a median time of 30 (IQR, 27-38) months on ART (N = 127). Viral suppression rate (HIV RNA levels ≤ 400 copies/ml) after a median time of 30 months on ART was found to be 88.2% (112/127), which is in the range for HIV drug resistance prevention suggested by WHO. Of those 15 patients with viral load >400 copies/ml, six harboured one or more drug resistant associated mutations in the reverse transcriptase (RT) region. Observed NRTIs resistance associated mutations were the lamivudine-induced mutation M184V (n = 4) and tenofovir associated mutation K65R (n = 1). The NNRTIs resistance associated mutations were K103N (n = 2), V106M, Y181S, Y188L, V90I, K101E and G190A (n = 1 each). Thymidine analogue mutations and major drug resistance mutations in the protease (PR) region were not detected. Most of the patients (13/15) with virologic failure and accumulated drug resistance mutations had not met the WHO clinical and/or immunological failure criteria and continued the failing regimen. The incidence and pattern of acquired antiretroviral drug resistance mutations is lower and less complex than previous reports from sub Saharan Africa countries. Nevertheless, the data suggest the need for virological monitoring and resistance testing for early detection of failure. Moreover, adherence reinforcement will contribute to improving overall treatment outcomes.
Conflict of interest statement
Figures
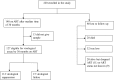
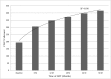
References
-
- Gilks CF, Crowley S, Ekpini R, Gove S, Perriens J, Souteyrand Y,et al. The WHO public-health approach to antiretroviral treatment against HIV in resource-limited settings. Lancet 2006. August 5; 368(9534). - PubMed
-
- World Health Organization. Towards universal access: scaling up priority HIV/AIDS interventions in the health sector (2010): progress report. Available: http://www.who.int/hiv/pub/2010progressreport/report/en/index.html
-
- Ivers LC, Kendrick D, Doucette K. Efficacy of antiretroviral therapy programs in resource-poor settings: a meta-analysis of the published literature. Clin Infect Dis 2005. July 15; 41(2). - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Molecular Biology Databases
Research Materials
Miscellaneous

