Variation in breast cancer care quality in New York and California based on race/ethnicity and Medicaid enrollment
- PMID: 26536043
- PMCID: PMC4724235
- DOI: 10.1002/cncr.29777
Variation in breast cancer care quality in New York and California based on race/ethnicity and Medicaid enrollment
Abstract
Background: Racial/ethnic and socioeconomic disparities persist in part because our current understanding of the care provided to minority and disadvantaged populations is limited. The authors evaluated the quality of breast cancer care in 2 large states to understand the disparities experienced by African Americans, Hispanics, Asian/Pacific Islanders (APIs), and Medicaid enrollees and to prioritize remediation strategies.
Methods: Statewide cancer registry data for 80,436 women in New York and 121,233 women in California who were diagnosed during 2004 to 2009 with stage 0 through III breast cancer were used to assess underuse and overuse of surgery, radiation, chemotherapy, and hormone therapy based on 34 quality measures. Concordance values were compared across racial/ethnic and Medicaid-enrollment groups. Multivariable models were used to quantify disparities across groups for each treatment in each state.
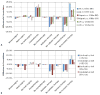
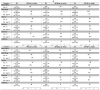
Results: Overall concordance was 76% for underuse measures and 87% for overuse measures. The proportions of patients who received care concordant with all relevant measures were 35% in New York and 33% in California. Compared with whites, African Americans were less likely to receive recommended surgery, radiation, and hormone therapy; Hispanics and APIs were usually more likely to receive recommended chemotherapy. Across states, the same racial/ethnic groups did not always experience the same disparities. Medicaid enrollment was associated with decreased likelihood of receiving all recommended treatments, except chemotherapy, in both states. Overuse was evident for hormone therapy and axillary surgery but was not associated with race/ethnicity or Medicaid enrollment.
Conclusions: Patient-level measures of quality identify substantial problems with care quality and meaningful disparities. Remediating these problems will require prioritizing low-performing measures and targeting high-risk populations, possibly in different ways for different regions.
Keywords: Medicaid; breast cancer; disparities; quality.
© 2015 American Cancer Society.
Conflict of interest statement
Conflicts of Interest: All authors declare no conflicts
Figures





References
-
- Malin JL, Schneider EC, Epstein AM, Adams J, Emanuel EJ, Kahn KA. Results of the National Initiative for Cancer Care Quality: How Can We Improve the Quality of Cancer Care in the United States? Journal of Clinical Oncology. 2006;24:626–634. - PubMed
-
- Du XL, Key CR, Osborne C, Mahnken JD, Goodwin JS. Discrepancy between consensus recommendations and actual community use of adjuvant chemotherapy in women with breast cancer. Annals of Internal Medicine. 2003;138:90–97. [see comment][erratum appears in Ann Intern Med. 2003 Nov 18;139(10):873][summary for patients in Ann Intern Med. 2003 Jan 21;138(2):I16; PMID: 12529113] - PMC - PubMed
-
- Harlan LC, Abrams J, Warren JL, Clegg L, Stevens J, Ballard-Barbash R. Adjuvant therapy for breast cancer: practice patterns of community physicians. Journal of Clinical Oncology. 2002;20:1809–1817. - PubMed
-
- Bickell NA, Wang JJ, Oluwole S, et al. Missed opportunities: racial disparities in adjuvant breast cancer treatment. Journal of Clinical Oncology. 2006;24:1357–1362. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

