Trans-Sector Integrated Treatment in Psychosis and Addiction
- PMID: 26554316
- PMCID: PMC4643160
- DOI: 10.3238/arztebl.2015.0683
Trans-Sector Integrated Treatment in Psychosis and Addiction
Abstract
Background: Patients with psychosis often develop comorbid addiction, with a lifetime prevalence of ca. 50%. Dual diagnoses are considered hard to treat. Long-term integrated treatment programs might improve such patients' outcomes, at least to a moderate extent, but they have not yet been adequately studied or implemented in Germany to date.
Methods: 100 dual diagnosis patients participated in a single-center, randomized, controlled trial under standard hospital treatment conditions. They were randomly allotted to two groups. Patients in the intervention group were admitted to a specialized open hospital ward, where they were given integrated treatment, including disorder-specific group therapy. Their treatment was continued with further disorder-specific group therapy in the outpatient setting. Patients in the control group were admitted to an open general psychiatric ward and received treatment as usual, but no disorder-specific treatment either during their hospitalization or in the subsequent outpatient phase. Follow-up examinations were performed three, six, and twelve months after inclusion. The primary outcome was defined as the changes in substance use and abstinence motivation. The secondary outcome consisted of the patients' satisfaction with treatment and with life in general, retention rate, psychopathology, rehospitalizations, and global level of functioning.
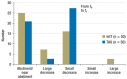
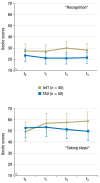
Results: The patients in the intervention group developed higher abstinence motivation than those in the control group (p = 0.009) and transiently reduced their substance use to a greater extent (p = 0.039 at three months). They were also more satisfied with their treatment (group effect: p = 0.011). Their global level of functioning and their retention rate were also higher, but these differences did not reach statistical significance.
Conclusion: Low-threshold, motivational, integrated treatment programs with psycho-educative and behavioral therapeutic elements may be helpful in the treatment of dual diagnosis patients and should be more extensively implemented as part of standard hospital treatment. Larger-scale, methodologically more complex studies will be needed to identify subgroups of patients that respond to such treatments in different ways.
Figures






Comment in
-
Effective and Neurobiologically Sound.Dtsch Arztebl Int. 2015 Oct 9;112(41):681-2. doi: 10.3238/arztebl.2015.0681. Dtsch Arztebl Int. 2015. PMID: 26554315 Free PMC article. No abstract available.
References
-
- Regier DA, Farmer ME, Rae DS, et al. Comorbidity of mental disorders with alcohol and other drug abuse. Results from the Epidemiologic Catchment Area (ECA) Study. JAMA. 1990;264:2511–2518. - PubMed
-
- Drake RE, Mueser KT. Psychosocial approaches to dual diagnosis. Schizophr Bull. 2000;261:05–18. - PubMed
-
- Gouzoulis-Mayfrank E. Komorbidität Psychose und Sucht - Grundlagen und Praxis. Mit Manualen für die Psychoedukation und Verhaltenstherapie. 2. erweiterte Auflage unter Mitarbeit von Schnell T. Darmstadt. Steinkopff. 2007
-
- Dixon L. Dual diagnosis of substance abuse in schizophrenia: prevalence and impact on outcomes. Schizophr Res. 1999;(35 Suppl):93–100. - PubMed
-
- Mueser KT, Yarnold PR, Rosenberg SD, Swett C, Jr, Miles KM, Hill D. Substance use disorder in hospitalized severely mentally ill psychiatric patients: prevalence, correlates, and subgroups. Schizophr Bull. 2000;26:179–192. - PubMed
Publication types
MeSH terms
Substances
Associated data
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

