Incidence of malaria by cotrimoxazole use in HIV-infected Ugandan adults on antiretroviral therapy: a randomised, placebo-controlled study
- PMID: 26558729
- PMCID: PMC4732005
- DOI: 10.1097/QAD.0000000000000956
Incidence of malaria by cotrimoxazole use in HIV-infected Ugandan adults on antiretroviral therapy: a randomised, placebo-controlled study
Abstract
Introduction: Previous unblinded trials have shown increased malaria among HIV-infected adults on antiretroviral therapy (ART) who stop cotrimoxazole (CTX) prophylaxis. We investigated the effect of stopping CTX on malaria in HIV-infected adults on ART in a double-blind, placebo-controlled trial.
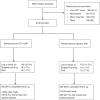
Methods: HIV-infected Ugandan adults stable on ART and CTX with CD4 cell count at least 250 cells/μl were randomized (1 : 1) to continue CTX or stop CTX and receive matching placebo (COSTOP trial; ISRCTN44723643). Clinical malaria was defined as fever and a positive blood slide, and considered severe if a participant had at least one clinical or laboratory feature of severity or was admitted to hospital. Malaria incidence and rate ratios were estimated using random effects Poisson regression, accounting for multiple episodes.
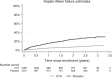
Results: A total of 2180 participants were enrolled and followed for a median of 2.5 years; 453 malaria episodes were recorded. Malaria incidence was 9.1/100 person-years (pyrs) [95% confidence interval (CI) = 8.2-10.1] and was higher on placebo (rate ratio 3.47; CI = 2.74-4.39). Malaria in the placebo arm decreased over time; although incidence remained higher than in the CTX arm, the difference between arms reduced slightly (interaction P value = 0.10). Fifteen participants experienced severe malaria (<1%); overall incidence was 0.30/100 pyrs (CI = 0.18-0.49). There was one malaria-related death (CTX arm).
Conclusion: HIV-infected adults - who are stable on ART and stop prophylactic CTX - experience more malaria than those that continue, but this difference is less than has been reported in previous trials. Few participants had severe malaria. Further research might be useful in identifying groups that can safely stop CTX prophylaxis.
Figures
Similar articles
-
Longitudinal effect of CD4 by cotrimoxazole use on malaria incidence among HIV-infected Ugandan adults on antiretroviral therapy: a randomized controlled study.Malar J. 2016 Jul 15;15:361. doi: 10.1186/s12936-016-1426-z. Malar J. 2016. PMID: 27417903 Free PMC article. Clinical Trial.
-
Effect of antiretroviral therapy on malaria incidence in HIV-infected Ugandan adults.AIDS. 2017 Feb 20;31(4):577-582. doi: 10.1097/QAD.0000000000001344. AIDS. 2017. PMID: 28121670 Free PMC article. Clinical Trial.
-
Safety of discontinuing cotrimoxazole prophylaxis among HIV infected adults on anti-retroviral therapy in Uganda (COSTOP trial): Design.Contemp Clin Trials. 2015 Jul;43:100-4. doi: 10.1016/j.cct.2015.05.015. Epub 2015 May 22. Contemp Clin Trials. 2015. PMID: 26009024 Free PMC article. Clinical Trial.
-
Folic acid supplementation and malaria susceptibility and severity among people taking antifolate antimalarial drugs in endemic areas.Cochrane Database Syst Rev. 2022 Feb 1;2(2022):CD014217. doi: 10.1002/14651858.CD014217. Cochrane Database Syst Rev. 2022. PMID: 36321557 Free PMC article.
-
Mefloquine for preventing malaria in pregnant women.Cochrane Database Syst Rev. 2018 Nov 14;11(11):CD011444. doi: 10.1002/14651858.CD011444.pub3. Cochrane Database Syst Rev. 2018. PMID: 30480761 Free PMC article.
Cited by
-
TSCQ study: a randomized, controlled, open-label trial of daily trimethoprim-sulfamethoxazole or weekly chloroquine among adults on antiretroviral therapy in Malawi: study protocol for a randomized controlled trial.Trials. 2016 Jul 18;17(1):322. doi: 10.1186/s13063-016-1392-3. Trials. 2016. PMID: 27431995 Free PMC article. Clinical Trial.
-
Prevalence, antimicrobial susceptibility and risk factors associated with non-typhoidal Salmonella on Ugandan layer hen farms.BMC Vet Res. 2017 Nov 29;13(1):365. doi: 10.1186/s12917-017-1291-1. BMC Vet Res. 2017. PMID: 29187195 Free PMC article.
-
The Manifesto of Pharmacoenosis: Merging HIV Pharmacology into Pathocoenosis and Syndemics in Developing Countries.Microorganisms. 2021 Jul 31;9(8):1648. doi: 10.3390/microorganisms9081648. Microorganisms. 2021. PMID: 34442727 Free PMC article. Review.
-
Effect of HIV and malaria parasites co-infection on immune-hematological profiles among patients attending anti-retroviral treatment (ART) clinic in Infectious Disease Hospital Kano, Nigeria.PLoS One. 2017 Mar 27;12(3):e0174233. doi: 10.1371/journal.pone.0174233. eCollection 2017. PLoS One. 2017. PMID: 28346490 Free PMC article.
-
Low prevalence of laboratory-confirmed malaria in clinically diagnosed adult women from the Wakiso district of Uganda.Malar J. 2016 Nov 14;15(1):555. doi: 10.1186/s12936-016-1604-z. Malar J. 2016. PMID: 27842555 Free PMC article.
References
-
- French N, Nakiyingi J, Lugada E, Watera C, Whitworth JA, Gilks CF. Increasing rates of malarial fever with deteriorating immune status in HIV-1-infected Ugandan adults. AIDS 2001; 15:899–906. - PubMed
-
- Morgan D, Maude GH, Malamba SS, Okongo MJ, Wagner HU, Mulder DW, et al. HIV-1 disease progression and AIDS-defining disorders in rural Uganda. Lancet 1997; 350:245–250. - PubMed
-
- Vergis EN, Mellors JW. Natural history of HIV-1 infection. Infect Dis Clin North Am 2000; 14:809–825.v-vi. - PubMed
-
- Boeree MJ, Sauvageot D, Banda HT, Harries AD, Zijlstra EE. Efficacy and safety of two dosages of cotrimoxazole as preventive treatment for HIV-infected Malawian adults with new smear-positive tuberculosis. Trop Med Int Health 2005; 10:723–733. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials