In vitro fertilisation for unexplained subfertility
- PMID: 26583517
- PMCID: PMC7154339
- DOI: 10.1002/14651858.CD003357.pub4
In vitro fertilisation for unexplained subfertility
Update in
-
In vitro fertilisation for unexplained subfertility.Cochrane Database Syst Rev. 2023 Sep 27;9(9):CD003357. doi: 10.1002/14651858.CD003357.pub5. Cochrane Database Syst Rev. 2023. PMID: 37753821 Free PMC article.
Abstract
Background: One-third of subfertile couples have no identifiable cause for their inability to conceive. In vitro fertilisation (IVF) is a widely accepted treatment for this condition; however, this treatment is invasive and expensive and is associated with risks.
Objectives: To evaluate the effectiveness and safety of IVF compared with expectant management, unstimulated intrauterine insemination (IUI) or intrauterine insemination along with ovarian stimulation with gonadotropins (IUI + gonadotropins) or clomiphene (IUI + CC) or letrozole (IUI + letrozole) in improving pregnancy outcomes.
Search methods: This review has drawn on the search strategy developed by the Cochrane Menstrual Disorders and Subfertility Group. We searched the Cochrane Menstrual Disorders and Subfertility Group Trials Register (searched May 2015), the Cochrane Central Register of Controlled Trials (CENTRAL; 2015, first quarter), MEDLINE (1946 to May 2015), EMBASE (1985 to May 2015), the Cumulative Index to Nursing and Allied Health Literature (CINAHL) (May 2015) and reference lists of articles. We searched the following trial registries: clinicaltrials.gov (http://www.clinicaltrials.gov) and the World Health Organization International Trials Registry Platform search portal (http://www.who.int/trialsearch/Default.aspx). We searched the Web of Science (http://wokinfo.com/) as another source of trials and conference abstracts, OpenGrey (http://www.opengrey.eu/) for unpublished literature from Europe and the Latin American Caribbean Health Sciences Literature (LILACS) database (http://regional.bvsalud.org/php/index.php?lang=en). Moreover, we handsearched relevant conference proceedings and contacted study authors to ask about additional publications.Two review authors independently assessed trial eligibility, extracted data and assessed risk of bias. The primary review outcome was cumulative live birth rate. Multiple pregnancy and other adverse effects were secondary outcomes. We combined data to calculate pooled risk ratios (RRs) and 95% confidence intervals (CIs). We assessed statistical heterogeneity by using the I(2) statistic. We assessed the overall quality of evidence for the main comparisons using Grades of Recommendation, Assessment, Development and Evaluation (GRADE) methods.
Selection criteria: We included randomised controlled trials (RCTs) in which the effectiveness of IVF in couples with unexplained subfertility was compared with that of other treatments, including expectant management, unstimulated IUI and stimulated IUI using gonadotropins or clomiphene or letrozole.Live birth rate (LBR) per woman was the primary outcome.
Data collection and analysis: Two review authors independently assessed the eligibility and quality of trials and evaluated the quality of the evidence by using GRADE criteria.
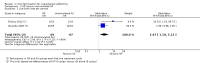
Main results: IVF versus expectant management (two RCTs):Live birth rate per woman was higher with IVF than with expectant management (odds ratio (OR) 22.00, 95% confidence interval (CI) 2.56 to 189.37, one RCT, 51 women, very low quality evidence). Multiple pregnancy rates (MPRs), ovarian hyperstimulation syndrome (OHSS) and miscarriage were not reported. IVF versus unstimulated IUI (two RCTs):Live birth rate was higher with IVF than with unstimulated IUI (OR 2.47, 95% CI 1.19 to 5.12, two RCTs, 156 women, I(2) = 60%, low quality evidence). There was no evidence of a difference between the groups in multiple pregnancy rates (OR 1.03, 95% CI 0.04 to 27.29, one RCT, 43 women, very low quality evidence) IVF versus IUI + ovarian stimulation with gonadotropins (three RCTs) or clomiphene (one RCT) or letrozole (no RCTs):Data from these trials could not be pooled because of high statistical heterogeneity (I(2) = 93.3%). Heterogeneity was eliminated when studies were stratified by pretreatment status.In trials comparing IVF versus IUI + gonadotropins among treatment-naive women, there was no conclusive evidence of a difference between the groups in live birth rates (OR 1.27, 95% CI 0.94 to 1.73, four RCTs, 745 women, I(2) = 8.0%, moderate-quality evidence). In women pretreated with IUI + clomiphene, a higher live birth rate was reported among those who underwent IVF than those given IUI + gonadotropins (OR 3.90, 95% CI 2.32 to 6.57, one RCT, 280 women, moderate-quality evidence).There was no conclusive evidence of a difference in live birth rates between IVF and IUI + CC in treatment-naive women (OR 2.51, 95% CI 0.96 to 6.55, one RCT, 103 women, low quality evidence).In treatment-naive women, there was no evidence of a difference in rates of multiple pregnancy between women who underwent IVF and those who received IUI + gonadotropins (OR 0.79, 95% CI 0.45 to 1.39, four RCTs, 745 women, I(2) = 0%, moderate quality evidence). There was no evidence of a difference in MPRs between women who underwent IVF compared with those given IUI + CC (OR 1.02, 95% CI 0.20 to 5.31, one RCT, 103 women, low-quality evidence).There was no evidence of a difference in ovarian hyperstimulation syndrome rate between treatment-naive women who underwent IVF and those given IUI + gonadotropins (OR 1.23, 95% CI 0.36 to 4.14, two RCTs, 221 women, low quality evidence). There was no evidence of a difference in OHSS rates between groups receiving IVF versus those receiving IUI + CC (OR 1.02, 95% CI 0.20 to 5.31, one RCT, 103 women, low-quality evidence).In treatment naive women, there was no evidence of a difference in miscarriage rates between IVF and IUI + CC (OR 1.16, 95% CI 0.44 to 3.02, one RCT, 103 women, low-quality evidence), nor between women treated with IVF versus those receiving IUI+ gonadotropins (OR 1.16, 95% CI 0.44 to 3.02, one RCT, 103 women).No studies compared IVF with IUI + letrozole.The quality of the evidence ranged from very low to moderate. The main limitation was serious imprecision resulting from small study numbers and low event rates.
Authors' conclusions: IVF may be associated with higher live birth rates than expectant management, but there is insufficient evidence to draw firm conclusions. IVF may also be associated with higher live birth rates than unstimulated IUI. In women pretreated with clomiphene + IUI, IVF appears to be associated with higher birth rates than IUI + gonadotropins. However in women who are treatment-naive there is no conclusive evidence of a difference in live birth rates between IVF and IUI + gonadotropins or between IVF and IUI + clomiphene. Adverse events associated with these interventions could not be adequately assessed owing to lack of evidence.
Conflict of interest statement
None known.
Figures


















Update of
-
In vitro fertilisation for unexplained subfertility.Cochrane Database Syst Rev. 2012 Apr 18;(4):CD003357. doi: 10.1002/14651858.CD003357.pub3. Cochrane Database Syst Rev. 2012. Update in: Cochrane Database Syst Rev. 2015 Nov 19;(11):CD003357. doi: 10.1002/14651858.CD003357.pub4. PMID: 22513911 Updated.
References
References to studies included in this review
Bensdorp 2015 {published data only}
-
- Bensdorp AJ, Tjon‐Kon‐Fat RI, Bossuyt PMM, Koks CA, Oosterhuis GJ, Hoek A, et al. Prevention of multiple pregnancies in couples with unexplained or mild male subfertility: a randomised controlled trial comparing in vitro fertilisation with single embryo transfer or in vitro fertilisation in a modified natural cycle to intrauterine insemination with controlled ovarian stimulation. BMJ 2015;9(350):g7771. - PMC - PubMed
Elzeiny 2014 {published data only}
-
- Elzeiny H, Garrett C, Toledo M, Stern K, McBain J, William H, et al. A randomised controlled trial of intra‐uterine insemination versus in vitro fertilisation in patients with idiopathic or mild male factor. Australian and New Zealand Journal of Obstetrics & Gynaecology 2014;54:156‐61. - PubMed
Goldman 2014 {published data only}
Goverde 2000 {published data only}
-
- Goverde AJ, McDonnell J, Vermeiden JPW, Schats R, Rutten FFH, Schoemaker J. Intrauterine insemination or in vitro fertilisation in idiopathic subfertility and male subfertility: a randomised trial and cost‐effectiveness analysis. Lancet 2000;355:13‐8. - PubMed
Hughes 2004 {published data only}
-
- Hughes EG, Beecroft ML, Wilkie V, Burville L, Claman P, Tummon I, et al. A multicentre randomized controlled trial of expectant management versus IVF in women with fallopian tube patency. Human Reproduction 2004;19(5):1105‐9. - PubMed
Reindollar 2010 {published data only}
-
- Reindollar RH, Regan MM, Neumann PJ, Levine BS, Thornton KL, Alper MM, et al. A randomized clinical trial to evaluate optimal treatment for unexplained infertility: the fast track and standard treatment (FASTT) trial. Fertility and Sterility 2010;94(3):888‐99. - PubMed
Soliman 1993 {published data only}
-
- Soliman S, Daya S, Collins J, Jarrell J. A randomized trial of in vitro fertilization versus conventional treatment for infertility. Fertility and Sterility 1993;59(6):1239‐44. - PubMed
van Rumste 2014 {published data only}
-
- Custers IM, Konig TE, Broekmans FJ, Hompes P, Kaaijk E, Oosterhuis J, et al. Couples with unexplained subfertility and unfavourable prognosis; a randomized pilot trial comparing the effectiveness of IVF‐eSET and IUI‐COS. Fertility & Sterility 2011;96(5):1107‐11. - PubMed
-
- Rumste MME, Custers IM, Koks CA, Weering HGI, Beckers NGM, Scheffer GJ, et al. IVF with planned single‐embryo transfer versus IUI with ovarian stimulation in couples with unexplained subfertility: an economic analysis. Reproductive Biomedicine Online 2014;28(3):336‐42. - PubMed
-
- Rumste MME, Custers IM, Koks CA, Weering HGI, Beckers NGM, Scheffer GJ, et al. IVF with single embryo transfer versus IUI with ovarian hyperstimulation in couples with unexplained subfertility, an economic analysis. Abstracts of the 25th Annual Meeting of ESHRE, Amsterdam, the Netherlands. 28 June‐1 July 2009;25:0‐110 Oral.
References to studies excluded from this review
Crosignani 1991 {published data only}
-
- Crosignani PG, Walters DE, Soliani A. Addendum to the ESHRE multicentre trial: a summary of the abortion and birth statistics. Human Reproduction 1992;2(7):286‐7. - PubMed
Custers 2012 {published data only}
-
- Custers IM, Rumste ME, Steeg JW, Wely M, Hompes PG, Bossuyt P, et al. Long‐term outcome in couples with unexplained subfertility and an intermediate prognosis initially randomized between expectant management and immediate treatment. Human Reproduction 2012;27(2):444‐50. - PubMed
Jarrell 1993 {published data only}
-
- Jarrell JF, Labelle R, Goeree R, Milner R, Collins J. In vitro fertilisation and embryo transfer: a randomised controlled trial. Online Journal of Current Clinical Trials 1993; Vol. Document number 73:73. - PubMed
Karande 1998 {published data only}
-
- Karande VC, Korn A, Morris A, Pao R, Balin M, Rinehart J, et al. Prospective randomized trial comparing the outcome and cost of in vitro fertilisation with that of a traditional treatment algorithm as first line therapy for couples with unexplained infertility. Fertility and Sterility 1998;71(3):468‐75. - PubMed
Leeton 1987 {published data only}
-
- Leeton J, Rogers P, Caro C, Healy D, Yates C. A controlled study between the use of gamete intrafallopian transfer and in vitro fertilisation and embryo transfer in the management of idiopathic and male infertility. Fertility and Sterility 1987;48(4):605‐7. - PubMed
Raneiri 1995 {published data only}
-
- Raneiri M, Beckett VA, Marchant S, Kinis A, Serhal P. Gamete intrafallopian transfer or in vitro fertilisation after failed ovarian stimulation and intrauterine insemination in unexplained infertility. Human Reproduction 1995;10(8):2023‐6. - PubMed
Tanbo 1990 {published data only}
-
- Tanbo T, Dale PO, Jarrell J. Assisted fertilization in infertile women with patent fallopian tubes. A comparison of in‐vitro fertilization, gamete intra‐fallopian transfer and tubal embryo stage transfer. Human Reproduction 1990;3(5):266‐70. - PubMed
Zayed 1997 {published data only}
-
- Zayed F, Lenton EA, Cooke ID. Comparison between stimulated in‐vitro fertilization and stimulated intrauterine insemination for the treatment of unexplained and mild male factor infertility. Human Reproduction 1997;12(11):2408‐13. - PubMed
References to ongoing studies
Nandi 2015 {published data only}
-
- Controlled ovarian stimulation and intrauterine insemination or in vitro fertilisation as first‐line treatment for unexplained infertility: a randomised controlled trial. Ongoing study 17/6/2013.
Additional references
Bhattacharya 2008
Collins 1995
-
- Collins JA, Burrows EA, Willan AR. The prognosis for live birth among untreated infertile couples. Fertility and Sterility 1995;64:22‐8. [MEDLINE: ] - PubMed
FIVNAT 2012
-
- Annual report of FIVNAT. French IVF National Registry, 2012 report.
Glujovsky 2012
-
- Glujovsky D, Blake D, Bardach A, Farquhar C. Cleavage stage versus blastocyst stage embryo transfer in assisted reproductive technology. Cochrane Database of Systematic Reviews 2012, Issue 7. - PubMed
HFEA 2012
-
- Fertility Treatment in 2012: Trends and Figures. http://www.hfea.gov.uk/104.html 2013.
Higgins 2011
-
- Higgins JPT, Green S (editors). Cochrane Handbook for Systematic Reviews of Interventions Version 5.1.0 [updated March 2011]. The Cochrane Collaboration, 2011. www.cochrane‐handbook.org.
Hughes 2010
Hunault 2004
-
- Hunault CC, Habbema JD, Eijkemans MJ, Collins JA, Evers JL, Velde ER. Two new prediction rules for spontaneous pregnancy leading to live birth among subfertile couples, based on the synthesis of three previous models. Human Reproduction 2004;19(9):2019‐26. - PubMed
Lenton 1977
-
- Lenton EA, Weston GA, Cooke ID. Long term follow up of apparently normal couple with a complaint of infertility. Fertility and Sterility 1977;28:913‐9. - PubMed
Maheshwari 2008
-
- Maheshwari M, Hamilton M, Bhattacharya S. Effect of female age on the diagnostic categories of infertility. Human Reproduction 2008;23:538‐42. - PubMed
Mouzon 2010
-
- Mouzon J, Goossens V, Bhattacharya S, Castilla JA, Ferraretti AP, Korsak V, et al. Assisted reproductive technology in Europe, 2006: results generated from European registers by ESHRE. Human Reproduction 2010;25(8):1851‐62. - PubMed
NICE 2013
-
- National Collaborating Centre for Women's and Children's Health. Fertility: Assessment and Treatment for People With Fertility Problems. Clinical Guideline. London: RCOG Press, 2013.
SART/ASRM 2014
-
- Society for Assisted Reproductive Technology and American Society for Reproductive Medicine. Assisted reproductive technology in the United States: 2012 results generated from the American Society for Reproductive Medicine/Society for Assisted Reproductive Technology Registry. ASRM Bulletin 2014;16(12).
Schulz 1995
-
- Schulz KF, Chalmers I, Hayes RJ, Altman DG. Empirical evidence of bias. Dimensions of methodological quality associated with estimates of treatment effects in controlled trials. JAMA 1995;273:408‐12. - PubMed
Snick 1997
-
- Snick HKA, Snick TS, Evers JLH, Collins JA. The spontaneous pregnancy prognosis in untreated subfertile couples: the Walcheren primary care study. Human Reproduction 1997;12(7):1582‐8. - PubMed
Steures 2006
-
- Steures P, Steeg JW, Hompes PG, Habbema JD, Eijkemans MJ, Broekmans FJ, et al. Intrauterine insemination with controlled ovarian hyperstimulation versus expectant management for couples with unexplained subfertility and an intermediate prognosis: a randomised clinical trial. Lancet 2006;368(9531):216‐21. - PubMed
Steures 2008
-
- Steures P, Steeg JW, Hompes PG, Bossuyt PM, Veen F, Habbema JD, et al. Intra‐uterine insemination with controlled ovarian hyperstimulation compared to an expectant management in couples with unexplained subfertility and an intermediate prognosis: a randomised study. Nederlands Tijdschrift voor Geneeskunde 2008;152(27):1525‐31. - PubMed
VARTA 2013
-
- Victorian Assisted Reproductive Treatment Authority. 2013 Annual Report. Melbourne, Australia, 2013.
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials

