Emergency Physician Attitudes, Preferences, and Risk Tolerance for Stroke as a Potential Cause of Dizziness Symptoms
- PMID: 26587108
- PMCID: PMC4644052
- DOI: 10.5811/westjem.2015.7.26158
Emergency Physician Attitudes, Preferences, and Risk Tolerance for Stroke as a Potential Cause of Dizziness Symptoms
Abstract
Introduction: We evaluated emergency physicians' (EP) current perceptions, practice, and attitudes towards evaluating stroke as a cause of dizziness among emergency department patients.
Methods: We administered a survey to all EPs in a large integrated healthcare delivery system. The survey included clinical vignettes, perceived utility of historical and exam elements, attitudes about the value of and requisite post-test probability of a clinical prediction rule for dizziness. We calculated descriptive statistics and post-test probabilities for such a clinical prediction rule.
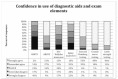
Results: The response rate was 68% (366/535). Respondents' median practice tenure was eight years (37% female, 92% emergency medicine board certified). Symptom quality and typical vascular risk factors increased suspicion for stroke as a cause of dizziness. Most respondents reported obtaining head computed tomography (CT) (74%). Nearly all respondents used and felt confident using cranial nerve and limb strength testing. A substantial minority of EPs used the Epley maneuver (49%) and HINTS (head-thrust test, gaze-evoked nystagmus, and skew deviation) testing (30%); however, few EPs reported confidence in these tests' bedside application (35% and 16%, respectively). Respondents favorably viewed applying a properly validated clinical prediction rule for assessment of immediate and 30-day stroke risk, but indicated it would have to reduce stroke risk to <0.5% to be clinically useful.
Conclusion: EPs report relying on symptom quality, vascular risk factors, simple physical exam elements, and head CT to diagnose stroke as the cause of dizziness, but would find a validated clinical prediction rule for dizziness helpful. A clinical prediction rule would have to achieve a 0.5% post-test stroke probability for acceptability.
Figures



References
-
- Saber Tehrani AS, Coughlan D, Hsieh YH, et al. Rising annual costs of dizziness presentations to U.S. emergency departments. Acad Emerg Med. 2013;20(7):689–96. - PubMed
-
- Kerber KA, Meurer WJ, West BT, et al. Dizziness presentations in U.S. emergency departments, 1995–2004. Acad Emerg Med. 2008;15(8):744–50. - PubMed
-
- Kuppermann N, Holmes JF, Dayan PS, et al. Identification of children at very low risk of clinically-important brain injuries after head trauma: a prospective cohort study. Lancet. 2009;374(9696):1160–70. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

