The emerging role of coagulation proteases in kidney disease
- PMID: 26592189
- PMCID: PMC4933505
- DOI: 10.1038/nrneph.2015.177
The emerging role of coagulation proteases in kidney disease
Abstract
A role of coagulation proteases in kidney disease beyond their function in normal haemostasis and thrombosis has long been suspected, and studies performed in the past 15 years have provided novel insights into the mechanisms involved. The expression of protease-activated receptors (PARs) in renal cells provides a molecular link between coagulation proteases and renal cell function and revitalizes research evaluating the role of haemostasis regulators in renal disease. Renal cell-specific expression and activity of coagulation proteases, their regulators and their receptors are dynamically altered during disease processes. Furthermore, renal inflammation and tissue remodelling are not only associated, but are causally linked with altered coagulation activation and protease-dependent signalling. Intriguingly, coagulation proteases signal through more than one receptor or induce formation of receptor complexes in a cell-specific manner, emphasizing context specificity. Understanding these cell-specific signalosomes and their regulation in kidney disease is crucial to unravelling the pathophysiological relevance of coagulation regulators in renal disease. In addition, the clinical availability of small molecule targeted anticoagulants as well as the development of PAR antagonists increases the need for in-depth knowledge of the mechanisms through which coagulation proteases might regulate renal physiology.
Conflict of interest statement
The authors declare no competing interests.
Figures


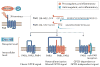
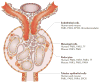

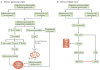
References
-
- Esmon CT. The interactions between inflammation and coagulation. Br J Haematol. 2005;131:417–430. - PubMed
-
- Benmira S, Banda ZK, Bhattacharya V. Old versus new anticoagulants: focus on pharmacology. Recent Pat Cardiovasc Drug Discov. 2010;5:120–137. - PubMed
-
- Ramachandran R, Noorbakhsh F, Defea K, Hollenberg MD. Targeting proteinase-activated receptors: therapeutic potential and challenges. Nat Rev Drug Discov. 2012;11:69–86. - PubMed
-
- Adams RL, Bird RJ. Review article: coagulation cascade and therapeutics update: relevance to nephrology. Part 1: Overview of coagulation, thrombophilias and history of anticoagulants. Nephrology (Carlton) 2009;14:462–470. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

