Insulin Resistance and Inflammation in Hypogonadotropic Hypogonadism and Their Reduction After Testosterone Replacement in Men With Type 2 Diabetes
- PMID: 26622051
- PMCID: PMC4686848
- DOI: 10.2337/dc15-1518
Insulin Resistance and Inflammation in Hypogonadotropic Hypogonadism and Their Reduction After Testosterone Replacement in Men With Type 2 Diabetes
Abstract
Objective: One-third of men with type 2 diabetes have hypogonadotropic hypogonadism (HH). We conducted a randomized placebo-controlled trial to evaluate the effect of testosterone replacement on insulin resistance in men with type 2 diabetes and HH.
Research design and methods: A total of 94 men with type 2 diabetes were recruited into the study; 50 men were eugonadal, while 44 men had HH. Insulin sensitivity was calculated from the glucose infusion rate (GIR) during hyperinsulinemic-euglycemic clamp. Lean body mass and fat mass were measured by DEXA and MRI. Subcutaneous fat samples were taken to assess insulin signaling genes. Men with HH were randomized to receive intramuscular testosterone (250 mg) or placebo (1 mL saline) every 2 weeks for 24 weeks.
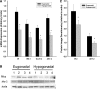
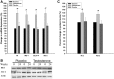
Results: Men with HH had higher subcutaneous and visceral fat mass than eugonadal men. GIR was 36% lower in men with HH. GIR increased by 32% after 24 weeks of testosterone therapy but did not change after placebo (P = 0.03 for comparison). There was a decrease in subcutaneous fat mass (-3.3 kg) and increase in lean mass (3.4 kg) after testosterone treatment (P < 0.01) compared with placebo. Visceral and hepatic fat did not change. The expression of insulin signaling genes (IR-β, IRS-1, AKT-2, and GLUT4) in adipose tissue was significantly lower in men with HH and was upregulated after testosterone treatment. Testosterone treatment also caused a significant fall in circulating concentrations of free fatty acids, C-reactive protein, interleukin-1β, tumor necrosis factor-α, and leptin (P < 0.05 for all).
Conclusions: Testosterone treatment in men with type 2 diabetes and HH increases insulin sensitivity, increases lean mass, and decreases subcutaneous fat.
Trial registration: ClinicalTrials.gov NCT01127659.
© 2016 by the American Diabetes Association. Readers may use this article as long as the work is properly cited, the use is educational and not for profit, and the work is not altered.
Figures
Similar articles
-
Testosterone Increases the Expression and Phosphorylation of AMP Kinase α in Men With Hypogonadism and Type 2 Diabetes.J Clin Endocrinol Metab. 2020 Apr 1;105(4):1169-75. doi: 10.1210/clinem/dgz288. J Clin Endocrinol Metab. 2020. PMID: 31858126 Free PMC article.
-
The effect of testosterone replacement therapy on adipocytokines and C-reactive protein in hypogonadal men with type 2 diabetes.Eur J Endocrinol. 2007 May;156(5):595-602. doi: 10.1530/EJE-06-0737. Eur J Endocrinol. 2007. PMID: 17468196 Clinical Trial.
-
Hypogonadotropic Hypogonadism in Men With Diabesity.Diabetes Care. 2018 Jul;41(7):1516-1525. doi: 10.2337/dc17-2510. Diabetes Care. 2018. PMID: 29934480 Free PMC article. Review.
-
The fatty acid transporter FAT/CD36 is upregulated in subcutaneous and visceral adipose tissues in human obesity and type 2 diabetes.Int J Obes (Lond). 2006 Jun;30(6):877-83. doi: 10.1038/sj.ijo.0803212. Int J Obes (Lond). 2006. PMID: 16418758
-
Metabolic Effects of Testosterone Therapy in Men with Type 2 Diabetes and Metabolic Syndrome.Sex Med Rev. 2019 Jul;7(3):476-490. doi: 10.1016/j.sxmr.2018.12.004. Epub 2019 Feb 22. Sex Med Rev. 2019. PMID: 30803918 Review.
Cited by
-
Testosterone Increases the Expression and Phosphorylation of AMP Kinase α in Men With Hypogonadism and Type 2 Diabetes.J Clin Endocrinol Metab. 2020 Apr 1;105(4):1169-75. doi: 10.1210/clinem/dgz288. J Clin Endocrinol Metab. 2020. PMID: 31858126 Free PMC article.
-
The association between serum testosterone and insulin resistance: a longitudinal study.Endocr Connect. 2018 Dec 1;7(12):1491-1500. doi: 10.1530/EC-18-0480. Endocr Connect. 2018. PMID: 30592706 Free PMC article.
-
Testosterone replacement therapy and cardiovascular risk.Nat Rev Cardiol. 2019 Sep;16(9):555-574. doi: 10.1038/s41569-019-0211-4. Nat Rev Cardiol. 2019. PMID: 31123340 Review.
-
Relationship between total testosterone, sex hormone-binding globulin levels and the severity of non-alcoholic fatty liver disease in males: a meta-analysis.Ther Adv Endocrinol Metab. 2022 Jun 24;13:20420188221106879. doi: 10.1177/20420188221106879. eCollection 2022. Ther Adv Endocrinol Metab. 2022. PMID: 35785018 Free PMC article.
-
The role of the androgen receptor in the pathogenesis of obesity and its utility as a target for obesity treatments.Obes Rev. 2022 Jun;23(6):e13429. doi: 10.1111/obr.13429. Epub 2022 Jan 27. Obes Rev. 2022. PMID: 35083843 Free PMC article. Review.
References
-
- Dhindsa S, Prabhakar S, Sethi M, Bandyopadhyay A, Chaudhuri A, Dandona P. Frequent occurrence of hypogonadotropic hypogonadism in type 2 diabetes. J Clin Endocrinol Metab 2004;89:5462–5468 - PubMed
-
- Bhatia V, Chaudhuri A, Tomar R, Dhindsa S, Ghanim H, Dandona P. Low testosterone and high C-reactive protein concentrations predict low hematocrit in type 2 diabetes. Diabetes Care 2006;29:2289–2294 - PubMed
-
- Hamilton EJ, Gianatti E, Strauss BJ, et al. . Increase in visceral and subcutaneous abdominal fat in men with prostate cancer treated with androgen deprivation therapy. Clin Endocrinol (Oxf) 2011;74:377–383 - PubMed
Publication types
MeSH terms
Substances
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

