Navigational Tools for Interventional Radiology and Interventional Oncology Applications
- PMID: 26622105
- PMCID: PMC4640922
- DOI: 10.1055/s-0035-1564705
Navigational Tools for Interventional Radiology and Interventional Oncology Applications
Abstract
The interventional radiologist is increasingly called upon to successfully access challenging biopsy and ablation targets, which may be difficult based on poor visualization, small size, or the proximity of vulnerable regional anatomy. Complex therapeutic procedures, including tumor ablation and transarterial oncologic therapies, can be associated with procedural risk, significant procedure time, and measurable radiation time. Navigation tools, including electromagnetic, optical, laser, and robotic guidance systems, as well as image fusion platforms, have the potential to facilitate these complex interventions with the potential to improve lesion targeting, reduce procedure time, and radiation dose, and thus potentially improve patient outcomes. This review will provide an overview of currently available navigational tools and their application to interventional radiology and oncology. A summary of the pertinent literature on the use of these tools to improve safety and efficacy of interventional procedures compared with conventional techniques will be presented.
Keywords: interventional oncology; interventional radiology; navigation; navigational tools; targeting.
Figures






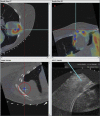


References
-
- Ward T J, Goldman R E, Weintraub J L. Electromagnetic navigation with multimodality image fusion for image-guided percutaneous interventions. Tech Vasc Interv Radiol. 2013;16(3):177–181. - PubMed
-
- Maintz J B, Viergever M A. A survey of medical image registration. Med Image Anal. 1998;2(1):1–36. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources

