RECALCITRANT CYSTOID MACULAR EDEMA AFTER PARS PLANA VITRECTOMY
- PMID: 26655611
- PMCID: PMC7362957
- DOI: 10.1097/IAE.0000000000000892
RECALCITRANT CYSTOID MACULAR EDEMA AFTER PARS PLANA VITRECTOMY
Abstract
Purpose: To evaluate the outcomes of different types of treatment of chronic cystoid macular edema (CME) after pars plana vitrectomy.
Methods: Retrospective review of eyes that developed chronic CME after pars plana vitrectomy treated with intravitreal triamcinolone acetonide (TCA) with or without the addition of anti-vascular endothelial growth factor.
Results: Thirty-nine eyes of 37 patients were included, with a median duration between pars plana vitrectomy and onset of CME of 5 months (interquartile range, 3-12). In most eyes (66.7%), the main indication for surgery was for vitreomacular interface disorders, such as epiretinal membrane, vitreomacular traction, and macular hole. With intravitreal TCA, there was a significant decrease in central foveal thickness at 3, 6, and 12 months, compared with baseline (P = 0.0171, 0.0401, and 0.0024, respectively). A significant gain in vision was noted at 1 month compared with baseline (P = 0.0169), but this was not sustained at 3, 6, and 12 months (P = 0.4862, 0.9098, and 0.4312, respectively). The addition of bevacizumab to TCA did not provide any additional benefit for central foveal thickness and visual acuity. Thirty-two eyes (82.1%) were started on prophylactic antiglaucoma drops 2 weeks after a TCA injection, and no eye needed laser or surgery to control intraocular pressure.
Conclusion: Chronic CME after pars plana vitrectomy is recurrent and difficult to treat. Intravitreal TCA is effective in reducing CME, but there was only short-term visual acuity improvement even with continued reduction of central foveal thickness. Intraocular pressure did not significantly rise with the use of prophylactic antiglaucoma drops even with repeated injections.
Conflict of interest statement
Financial Disclosures:
No financial disclosures. None of the authors have any proprietary interest.
Figures


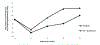

References
-
- Kim SJ, Martin DF, Hubbard GB 3rd, et al. Incidence of postvitrectomy macular edema using optical coherence tomography. Ophthalmology 2009;116(8):1531–7. - PubMed
-
- Frisina R, Pinackatt SJ, Sartore M, et al. Cystoid macular edema after pars plana vitrectomy for idiopathic epiretinal membrane. Graefes Arch Clin Exp Ophthalmol 2015;253(1):47–56. - PubMed
-
- Furino C, Boscia F, Recchimurzo N, Sborgia C, Alessio G. Intravitreal dexamethasone implant for refractory macular edema secondary to vitrectomy for macular pucker. Retina 2014;34(8):1612–6. - PubMed
-
- Chen CH, Wu PC, Liu YC. Intravitreal bevacizumab injection therapy for persistent macular edema after idiopathic macular epiretinal membrane surgery. J Ocul Pharmacol Ther 2011;27(3):287–92. - PubMed
-
- Taney LS, Baumal CR, Duker JS. Sustained-release dexamethasone intravitreal implant for persistent macular edema after vitrectomy for epiretinal membrane. Ophthalmic Surg Lasers Imaging Retina 2015;46(2):224–8. - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

