Platelet/lymphocyte ratio was associated with impaired myocardial perfusion and both in-hospital and long-term adverse outcome in patients with ST-segment elevation acute myocardial infarction undergoing primary coronary intervention
- PMID: 26677378
- PMCID: PMC4679796
- DOI: 10.5114/pwki.2015.55599
Platelet/lymphocyte ratio was associated with impaired myocardial perfusion and both in-hospital and long-term adverse outcome in patients with ST-segment elevation acute myocardial infarction undergoing primary coronary intervention
Abstract
Introduction: Platelet/lymphocyte ratio (PLR) has been shown to be an inflammatory and thrombotic biomarker for coronary heart disease, but its prognostic value in ST-segment elevation myocardial infarction (STEMI) has not been fully investigated.
Aim: To investigate the relationship between PLR and no-reflow, along with the in-hospital and long-term outcomes in patients with STEMI.
Material and methods: In the present study, we included 304 consecutive patients suffering from STEMI who underwent primary percutaneous coronary intervention (p-PCI). Patients were stratified according to PLR tertiles based on the blood samples obtained in the emergency room upon admission. No-reflow after p-PCI was defined as a coronary thrombolysis in myocardial infarction (TIMI) flow grade ≤ 2 after vessel recanalization, or TIMI flow grade 3 together with a final myocardial blush grade (MBG) < 2.
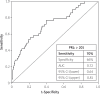
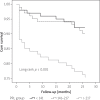
Results: The mean follow-up period was 24 months (range: 22-26 months). The number of patients characterized with no-reflow was counted to depict increments throughout successive PLR tertiles (14% vs. 20% vs. 45%, p < 0.001). In-hospital major adverse cardiovascular events and death increased as the PLR increased (p < 0.001, p < 0.001). Long-term MACE and death also increased as the PLR increased (p < 0.001, p < 0.001). Multivariable logistic regression analysis revealed that PLR remained an independent predictor for both in-hospital (OR = 1.01, 95% CI: 1.00-1.01; p = 0.002) and major long-term (OR = 1.01, 95% CI: 1.00-1.01; p < 0.001) adverse cardiac events.
Conclusions: Platelet/lymphocyte ratio on admission is a strong and independent predictor of both the no-reflow phenomenon and long-term prognosis following p-PCI in patients with STEMI.
Keywords: ST-segment elevation acute myocardial infarction; in-hospital mortality; long-term mortality; no-reflow; platelet/lymphocyte ratio.
Figures
Similar articles
-
The neutrophil to lymphocyte ratio was associated with impaired myocardial perfusion and long term adverse outcome in patients with ST-elevated myocardial infarction undergoing primary coronary intervention.Atherosclerosis. 2013 May;228(1):203-10. doi: 10.1016/j.atherosclerosis.2013.02.017. Epub 2013 Feb 24. Atherosclerosis. 2013. PMID: 23489347
-
Predictive value of admission red cell distribution width-platelet ratio for no-reflow phenomenon in acute ST segment elevation myocardial infarction undergoing primary percutaneous coronary intervention.Cardiol J. 2016;23(1):84-92. doi: 10.5603/CJ.a2015.0070. Epub 2015 Oct 27. Cardiol J. 2016. PMID: 26503078
-
Usefulness of the platelet-to-lymphocyte ratio in predicting angiographic reflow after primary percutaneous coronary intervention in patients with acute ST-segment elevation myocardial infarction.Am J Cardiol. 2014 Aug 1;114(3):342-7. doi: 10.1016/j.amjcard.2014.04.045. Epub 2014 May 15. Am J Cardiol. 2014. PMID: 24948493
-
Platelet-to-lymphocyte ratio and prognosis in STEMI: A meta-analysis.Eur J Clin Invest. 2021 Mar;51(3):e13386. doi: 10.1111/eci.13386. Epub 2020 Sep 25. Eur J Clin Invest. 2021. PMID: 32810283 Review.
-
Predictive value of neutrophil to lymphocyte ratio in patients with acute ST segment elevation myocardial infarction after percutaneous coronary intervention: a meta-analysis.BMC Cardiovasc Disord. 2018 May 2;18(1):75. doi: 10.1186/s12872-018-0812-6. BMC Cardiovasc Disord. 2018. PMID: 29716535 Free PMC article. Review.
Cited by
-
Inflammatory Conditions in Acute Coronary Syndrome Patients Treated with Percutaneous Coronary Intervention of Saphenous Vein Graft.Int J Angiol. 2020 Dec;29(4):237-244. doi: 10.1055/s-0040-1714751. Epub 2020 Aug 30. Int J Angiol. 2020. PMID: 33268974 Free PMC article.
-
Platelet-To-Lymphocyte Ratio Efficiency in Predicting Major Adverse Cardiovascular Events After Percutaneous Coronary Intervention in Acute Coronary Syndromes: A Meta-Analysis.Rev Cardiovasc Med. 2025 May 21;26(5):27942. doi: 10.31083/RCM27942. eCollection 2025 May. Rev Cardiovasc Med. 2025. PMID: 40475740 Free PMC article.
-
Prognostic Value of Circulating Inflammatory Cells in Patients with Stable and Acute Coronary Artery Disease.Front Cardiovasc Med. 2017 Jul 14;4:44. doi: 10.3389/fcvm.2017.00044. eCollection 2017. Front Cardiovasc Med. 2017. PMID: 28770211 Free PMC article. Review.
-
The prognostic value of dynamic changes in SII for the patients with STEMI undergoing PPCI.BMC Cardiovasc Disord. 2024 Jan 23;24(1):67. doi: 10.1186/s12872-023-03679-w. BMC Cardiovasc Disord. 2024. PMID: 38262934 Free PMC article.
-
The Pathogenic Role of Oxidative Stress, Cytokine Expression, and Impaired Hematological Indices in Diabetic Cardiovascular Diseases.Inflammation. 2023 Feb;46(1):146-160. doi: 10.1007/s10753-022-01718-w. Epub 2022 Aug 23. Inflammation. 2023. PMID: 35997998 Free PMC article.
References
-
- Brosh D, Assali AR, Mager A, et al. Effect of no-reflow during primary percutaneous coronary intervention for acute myocardial infarction on six-month mortality. Am J Cardiol. 2007;99:442–5. - PubMed
-
- Bolognese L, Carrabba N, Parodi G, et al. Impact of microvascular dysfunction on left ventricular remodeling and long-term clinical outcome after primary coronary angioplasty for acute myocardial infarction. Circulation. 2004;109:1121–6. - PubMed
-
- Rezkalla SH, Kloner RA. No-reflow phenomenon. Circulation. 2002;105:656–62. - PubMed
-
- Tanboga IH, Topcu S, Aksakal E, et al. Determinants of angiographic thrombus burden in patients with ST-segment elevation myocardial infarction. Clin Appl Thromb Hemost. 2014;20:716–22. - PubMed
-
- Gürsoy OM, Karakoyun S, KalçIk M, et al. Usefulness of novel hematologic inflammatory parameters to predict prosthetic mitral valve. Am J Cardiol. 2014;113:860–4. - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous