Continued high incidence of children with severe influenza A(H1N1)pdm09 admitted to paediatric intensive care units in Germany during the first three post-pandemic influenza seasons, 2010/11-2012/13
- PMID: 26678835
- PMCID: PMC4683816
- DOI: 10.1186/s12879-015-1293-1
Continued high incidence of children with severe influenza A(H1N1)pdm09 admitted to paediatric intensive care units in Germany during the first three post-pandemic influenza seasons, 2010/11-2012/13
Abstract
Background: Previous influenza surveillance at paediatric intensive care units (PICUs) in Germany indicated increased incidence of PICU admissions for the pandemic influenza subtype A(H1N1)pdm09. We investigated incidence and clinical characteristics of influenza in children admitted to PICUs during the first three post-pandemic influenza seasons, using active screening.
Methods: We conducted a prospective surveillance study in 24 PICUs in Bavaria (Germany) from October 2010 to September 2013. Influenza cases among children between 1 month and 16 years of age admitted to these PICUs with acute respiratory infection were confirmed by PCR analysis of respiratory secretions.
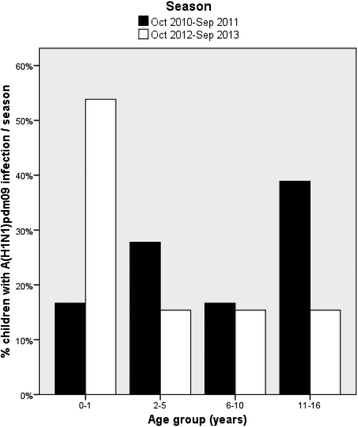
Results: A total of 24/7/20 influenza-associated PICU admissions were recorded in the post-pandemic seasons 1/2/3; incidence estimates per 100,000 children were 1.72/0.76/1.80, respectively. Of all 51 patients, 80% had influenza A, including 65% with A(H1N1)pdm09. Influenza A(H1N1)pdm09 was almost absent in season 2 (incidence 0.11), but dominated PICU admissions in seasons 1 (incidence 1.35) and 3 (incidence 1.17). Clinical data was available for 47 influenza patients; median age was 4.8 years (IQR 1.6-11.0). The most frequent diagnoses were influenza-associated pneumonia (62%), bronchitis/bronchiolitis (32%), secondary bacterial pneumonia (26 %), and ARDS (21%). Thirty-six patients (77 %) had underlying medical conditions. Median duration of PICU stay was 3 days (IQR 1-11). Forty-seven per cent of patients received mechanical ventilation, and one patient (2%) extracorporeal membrane oxygenation; 19% were treated with oseltamivir. Five children (11%) had pulmonary sequelae. Five children (11%) died; all had underlying chronic conditions and were infected with A(H1N1)pdm09. In season 3, patients with A(H1N1)pdm09 were younger than in season 1 (p = 0.020), were diagnosed more often with bronchitis/bronchiolitis (p = 0.004), and were admitted to a PICU later after the onset of influenza symptoms (p = 0.041).
Conclusions: Active screening showed a continued high incidence of A(H1N1)pdm09-associated PICU admissions in the post-pandemic seasons 1 and 3, and indicated possible underestimation of incidence in previous German studies. The age shift of severe A(H1N1)pdm09 towards younger children may be explained by increasing immunity in the older paediatric population. The high proportion of patients with underlying chronic conditions indicates the importance of consistent implementation of the current influenza vaccination recommendations for risk groups in Germany.
Figures
References
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources

