Differential Impact of Constrictive Physiology after Pericardiocentesis in Malignancy Patients with Pericardial Effusion
- PMID: 26691279
- PMCID: PMC4686385
- DOI: 10.1371/journal.pone.0145461
Differential Impact of Constrictive Physiology after Pericardiocentesis in Malignancy Patients with Pericardial Effusion
Abstract
Background: Echocardiographic signs of constrictive physiology (CP) after pericardiocentesis are frequently observed in malignancy patients. The purpose of the current study was to explore whether features of CP after pericardiocentesis have prognostic impact in malignancy patients with pericardial effusion (PE).
Methods: We retrospectively reviewed 467 consecutive patients who underwent pericardiocentesis at our institution from January 2006 to May 2014. Among them, 205 patients with advanced malignancy who underwent comprehensive echocardiography after the procedure comprised the study population. Co-primary end points were all-cause mortality (ACM) and repeated drainage (RD) for PE. Patients were divided into four subgroups according to cytologic result for malignant cells and CP (positive cytology with negative CP, both positive, both negative, and negative cytology with positive CP).
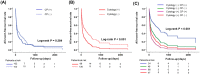
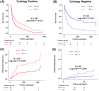
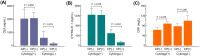
Results: CP after pericardiocentesis was present in 106 patients (50%) at median 4 days after the procedure. During median follow-up of 208 days, ACM and RD occurred in 162 patients (79%) and 29 patients (14%), respectively. Cox regression analysis revealed that independent predictors for ACM were male gender and positive cytology (all, p < 0.05). For RD, predictors were positive cytology, the absence of cardiac tamponade, and negative CP after pericardiocentesis (all, p < 0.05). When the patients were divided into four subgroups, patients with negative cytology and positive CP demonstrated the most favorable survival (hazard ratio [HR]: 0.39, p = 0.005) and the lowest RD rates (HR: 0.07, p = 0.012).
Conclusion: CP after pericardiocentesis is common, but does not always imply poor survival or the need for RD in patients with advanced malignancies. On the contrary, the presence of CP in patients with negative cytology conferred the most favorable survival and the lowest rate of RD. Comprehensive echocardiographic evaluation for CP after pericardiocentesis would be helpful for predicting prognosis in patients with advanced malignancies.
Conflict of interest statement
Figures

Similar articles
-
Abnormal cytology predicts poor prognosis in cancer patients with pericardial effusion.J Clin Oncol. 2005 Aug 1;23(22):5211-6. doi: 10.1200/JCO.2005.00.745. J Clin Oncol. 2005. PMID: 16051963
-
Effectiveness and prognosis of initial pericardiocentesis in the primary management of malignant pericardial effusion.Interact Cardiovasc Thorac Surg. 2010 Aug;11(2):154-61. doi: 10.1510/icvts.2010.232546. Epub 2010 May 26. Interact Cardiovasc Thorac Surg. 2010. PMID: 20504889
-
Safety and Outcome of Percutaneous Drainage of Pericardial Effusions in Patients with Cancer.Am J Cardiol. 2018 Sep 15;122(6):1091-1094. doi: 10.1016/j.amjcard.2018.06.002. Epub 2018 Jun 22. Am J Cardiol. 2018. PMID: 30064854
-
Patient characteristics and predictors of mortality associated with pericardial decompression syndrome: a comprehensive analysis of published cases.Eur Heart J Acute Cardiovasc Care. 2015 Apr;4(2):113-20. doi: 10.1177/2048872614547975. Epub 2014 Sep 1. Eur Heart J Acute Cardiovasc Care. 2015. PMID: 25178691 Review.
-
Echocardiography in the diagnosis and management of pericardial disease.J Cardiovasc Med (Hagerstown). 2006 Jul;7(7):533-44. doi: 10.2459/01.JCM.0000234772.73454.57. J Cardiovasc Med (Hagerstown). 2006. PMID: 16801815 Review.
Cited by
-
Characteristics and Clinical Outcomes of Cancer Patients who Developed Constrictive Physiology After Pericardiocentesis.Korean Circ J. 2022 Jan;52(1):74-83. doi: 10.4070/kcj.2021.0217. Epub 2021 Nov 1. Korean Circ J. 2022. PMID: 34877827 Free PMC article.
-
Post-pericardiocentesis Constrictive Physiology in Cancer Patients With Pericardial Effusion.Korean Circ J. 2022 Jan;52(1):84-86. doi: 10.4070/kcj.2021.0382. Korean Circ J. 2022. PMID: 34989195 Free PMC article. No abstract available.
-
Case report: Successful treatment of malignant pericardial effusion with pericardiocentesis, concurrent anti-inflammatory therapy and cancer therapy.Front Cardiovasc Med. 2023 Oct 12;10:1285233. doi: 10.3389/fcvm.2023.1285233. eCollection 2023. Front Cardiovasc Med. 2023. PMID: 37900575 Free PMC article.
References
-
- Ben-Horin S, Bank I, Guetta V, Livneh A. Large symptomatic pericardial effusion as the presentation of unrecognized cancer: a study in 173 consecutive patients undergoing pericardiocentesis. Medicine (Baltimore). 2006;85: 49–53. - PubMed
-
- Tsang TS, Seward JB, Barnes ME, Bailey KR, Sinak LJ, Urban LH, et al. Outcomes of primary and secondary treatment of pericardial effusion in patients with malignancy. Mayo Clin Proc. 2000;75: 248–253. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

