Posterior Urethral Strictures
- PMID: 26691883
- PMCID: PMC4672120
- DOI: 10.1155/2015/628107
Posterior Urethral Strictures
Abstract
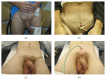
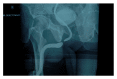
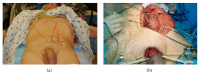
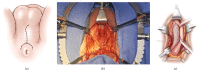
Pelvic fracture urethral injuries are typically partial and more often complete disruptions of the most proximal bulbar and distal membranous urethra. Emergency management includes suprapubic tube placement. Subsequent primary realignment to place a urethral catheter remains a controversial topic, but what is not controversial is that when there is the development of a stricture (which is usually obliterative with a distraction defect) after suprapubic tube placement or urethral catheter removal, the standard of care is delayed urethral reconstruction with excision and primary anastomosis. This paper reviews the management of patients who suffer pelvic fracture urethral injuries and the techniques of preoperative urethral imaging and subsequent posterior urethroplasty.
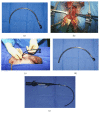
Figures




Similar articles
-
Traumatic Posterior Urethral Strictures in Children and Adolescents.Front Pediatr. 2019 Feb 19;7:24. doi: 10.3389/fped.2019.00024. eCollection 2019. Front Pediatr. 2019. PMID: 30838189 Free PMC article. Review.
-
Pelvic fracture urethral injuries in girls.J Urol. 2001 May;165(5):1660-5. J Urol. 2001. PMID: 11342950
-
Straddle injuries to the bulbar urethra: management and outcome in 53 patients.Int Braz J Urol. 2009 Jul-Aug;35(4):450-8. doi: 10.1590/s1677-55382009000400009. Int Braz J Urol. 2009. PMID: 19719861
-
Management of posterior urethral disruption injuries.Nat Clin Pract Urol. 2009 Mar;6(3):154-63. doi: 10.1038/ncpuro1319. Nat Clin Pract Urol. 2009. PMID: 19265857 Review.
-
The management of the acute setting of pelvic fracture urethral injury (realignment vs. suprapubic cystostomy alone).Arab J Urol. 2015 Mar;13(1):7-12. doi: 10.1016/j.aju.2014.08.003. Epub 2014 Sep 17. Arab J Urol. 2015. PMID: 26019971 Free PMC article. Review.
Cited by
-
Reconstruction of Membranous Urethral Strictures.Curr Urol Rep. 2018 Apr 11;19(6):37. doi: 10.1007/s11934-018-0786-z. Curr Urol Rep. 2018. PMID: 29644478 Review.
-
Development of a novel indwelling catheter for urethral surgery.Medicine (Baltimore). 2018 Aug;97(35):e12030. doi: 10.1097/MD.0000000000012030. Medicine (Baltimore). 2018. PMID: 30170412 Free PMC article.
-
[Contemporary management of pelvic fracture urethral injuries].Urologie. 2022 Jun;61(6):602-608. doi: 10.1007/s00120-022-01833-4. Epub 2022 Apr 27. Urologie. 2022. PMID: 35476111 Review. German.
-
Perineal midline vertical incision verses inverted-U incision in the urethroplasty: which is better?World J Urol. 2018 Aug;36(8):1267-1274. doi: 10.1007/s00345-018-2267-x. Epub 2018 Mar 14. World J Urol. 2018. PMID: 29541891
-
Mesh Graft Urethroplasty-Still a Safe and Promising Technique in Mostly Unpromising Complex Urethral Strictures.J Clin Med. 2022 Oct 11;11(20):5989. doi: 10.3390/jcm11205989. J Clin Med. 2022. PMID: 36294313 Free PMC article. Review.
References
-
- Coffield K. S., Weems W. L. Experience with management of posterior urethral injury associated with pelvic fracture. The Journal of Urology. 1977;117(6):722–724. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources

