Predictors of response to 17-alpha hydroxyprogesterone caproate for prevention of recurrent spontaneous preterm birth
- PMID: 26692181
- PMCID: PMC4803498
- DOI: 10.1016/j.ajog.2015.12.010
Predictors of response to 17-alpha hydroxyprogesterone caproate for prevention of recurrent spontaneous preterm birth
Abstract
Background: Prematurity is the leading cause of neonatal morbidity and death among nonanomalous neonates in the United States. Intramuscular 17-alpha hydroxyprogesterone caproate injections reduce the risk of recurrent prematurity by approximately one third. Unfortunately, prophylactic 17-alpha hydroxyprogesterone caproate is not always effective, and one-third of high-risk women will have a recurrent preterm birth, despite 17-alpha hydroxyprogesterone caproate therapy. The reasons for this variability in response are unknown. Previous investigators have examined the influence of a variety of factors on 17-alpha hydroxyprogesterone caproate response but have analyzed data that used a fixed outcome of term delivery to define progesterone response.
Objective: We hypothesized that the demographics, history, and pregnancy course among women who deliver at a similar gestational age with 17-alpha hydroxyprogesterone caproate for recurrent spontaneous preterm birth prevention differs when compared with those women who deliver later with 17-alpha hydroxyprogesterone caproate and that these associations could be refined by the use of a contemporary definition of 17-alpha hydroxyprogesterone caproate "responder."
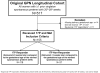
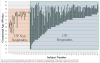
Study design: This was a planned secondary analysis of a prospective, multicenter, longitudinal study of women with ≥1 previous documented singleton spontaneous preterm birth at <37 weeks gestation. Data were collected at 3 prespecified gestational age epochs during pregnancy. All women who were included in this analysis received 17-alpha hydroxyprogesterone caproate during the studied pregnancy. We classified women as a 17-alpha hydroxyprogesterone caproate responder or nonresponder by calculating the difference in delivery gestational age between the 17-alpha hydroxyprogesterone caproate-treated pregnancy and her earliest spontaneous preterm birth. Responders were defined as those with pregnancy that extended ≥3 weeks later with 17-alpha hydroxyprogesterone caproate, compared with the delivery gestational age of their earliest previous spontaneous preterm birth. Data were analyzed with the use of chi-square test, t-test, and logistic regression.
Results: One hundred fifty-five women met the inclusion criteria. The 118 responders delivered later on average (37.7 weeks gestation) than the 37 nonresponders (33.5 weeks gestation; P < .001). Among responders, 32% (38/118 women) had a recurrent spontaneous preterm birth. Demographics (age, race/ethnicity, education, and parity) were similar between groups. In the regression model, the gestational age of the previous spontaneous preterm birth (odds ratio, 0.68; 95% confidence interval, 0.56-0.82; P < .001), vaginal bleeding/abruption in the current pregnancy (odds ratio, 0.24; 95% confidence interval, 0.06-0.88; P = .031), and first-degree family history of spontaneous preterm birth (odds ratio, 0.37; 95% confidence interval, 0.15-0.88; P = .024) were associated with response to 17-alpha hydroxyprogesterone caproate. Because women with a penultimate preterm pregnancy were more likely to be 17-alpha hydroxyprogesterone caproate nonresponders, we performed an additional limited analysis examining only the 130 women whose penultimate pregnancy was preterm. In regression models, the results were similar to those in the main cohort.
Conclusion: Several historic and current pregnancy characteristics define women who are at risk for recurrent preterm birth at a similar gestational age, despite 17-alpha hydroxyprogesterone caproate therapy. These data should be studied prospectively in larger cohorts and combined with genetic and environmental data to identify women who are most likely to benefit from this intervention.
Keywords: decidual hemorrhage; progesterone; recurrent preterm birth; spontaneous preterm labor.
Copyright © 2016 Elsevier Inc. All rights reserved.
Conflict of interest statement
Figures
Comment in
-
Always ask why!Am J Obstet Gynecol. 2016 Mar;214(3):303-5. doi: 10.1016/j.ajog.2015.12.001. Am J Obstet Gynecol. 2016. PMID: 26928144 No abstract available.
-
17 Alpha-hydroxyprogesterone caproate for preterm prevention: issues in subgroup analysis.Am J Obstet Gynecol. 2016 Mar;214(3):306-7. doi: 10.1016/j.ajog.2015.12.002. Am J Obstet Gynecol. 2016. PMID: 26928145 No abstract available.
References
-
- Schoen CN, Tabbah S, Iams JD, Caughey AB, Berghella V. Why the United States preterm birth rate is declining. American journal of obstetrics and gynecology. 2014 - PubMed
-
- Henderson JJ, McWilliam OA, Newnham JP, Pennell CE. Preterm birth aetiology 2004–2008. Maternal factors associated with three phenotypes: spontaneous preterm labour, preterm pre-labour rupture of membranes and medically indicated preterm birth. The journal of maternal-fetal & neonatal medicine: the official journal of the European Association of Perinatal Medicine, the Federation of Asia and Oceania Perinatal Societies, the International Society of Perinatal Obstet. 2012;25:642–7. - PubMed
-
- Adams MM, Elam-Evans LD, Wilson HG, Gilbertz DA. Rates of and factors associated with recurrence of preterm delivery. JAMA. 2000;283:1591–6. - PubMed
-
- Esplin MS, O’Brien E, Fraser A, et al. Estimating recurrence of spontaneous preterm delivery. Obstet Gynecol. 2008;112:516–23. - PubMed
-
- Simonsen SE, Lyon JL, Stanford JB, Porucznik CA, Esplin MS, Varner MW. Risk factors for recurrent preterm birth in multiparous Utah women: a historical cohort study. BJOG. 2013;120:863–72. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
- U01 HD050078/HD/NICHD NIH HHS/United States
- U01-HD-050062/HD/NICHD NIH HHS/United States
- U01 HD050088/HD/NICHD NIH HHS/United States
- U01-HD-050094/HD/NICHD NIH HHS/United States
- 5K23HD067224/HD/NICHD NIH HHS/United States
- U01 HD050094/HD/NICHD NIH HHS/United States
- U01-HD-050080/HD/NICHD NIH HHS/United States
- U01 HD050062/HD/NICHD NIH HHS/United States
- U01-HD-050088/HD/NICHD NIH HHS/United States
- K23 HD067224/HD/NICHD NIH HHS/United States
- U01-HD-050078/HD/NICHD NIH HHS/United States
- U01 HD050080/HD/NICHD NIH HHS/United States
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous