Sorafenib treatment during partial hepatectomy reduces tumorgenesis in an inflammation-associated liver cancer model
- PMID: 26695439
- PMCID: PMC4826248
- DOI: 10.18632/oncotarget.6638
Sorafenib treatment during partial hepatectomy reduces tumorgenesis in an inflammation-associated liver cancer model
Abstract
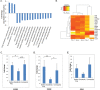
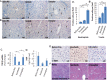
The long-term prognosis after resection of hepatocellular carcinoma (HCC), which is one of the treatment options for early-stage HCC, remains unsatisfactory as a result of a high incidence of disease recurrence. Recent studies performed in murine models revealed a link between liver regeneration under chronic inflammation and hepatic tumorigenesis. Sorafenib is a potent drug for advanced HCC with multikinase inhibition activity. We propose that inhibition of signal transduction pathways which are activated during hepatectomy, using Sorafenib, will reduce accelerated tumorigenesis. To test this hypothesis, we studied the Mdr2-knockout (KO) mouse strain, a model of inflammation-associated cancer, which underwent partial hepatectomy (PHx) at three months of age, with or without Sorafenib.Here we show that Sorafenib treatment during PHx inhibited different signal transduction pathways at the multikinase levels, but did not result in increased morbidity or mortality. At the early stages after PHx, Sorafenib treatment had no effect on the course of proliferation, apoptosis and DNA repair in the regenerating liver, but resulted in decreased stellate cells activation and inflammatory response. Finally, we show that Sorafenib treatment during PHx at three months of age resulted in decreased fibrosis and tumor formation at 8.5 months.In conclusion our study indicates that short-term Sorafenib treatment during PHx is safe and effective in inhibiting inflammation-associated cancer, and is therefore a potential strategy for recurrence prevention in patients with early-stage HCC treated with PHx.
Keywords: Mdr2 knockout; Sorafenib; hepatectomy; liver cancer; stellate cells.
Conflict of interest statement
The authors have no conflicts to disclose in relation to this work.
Figures



Similar articles
-
Fasting inhibits hepatic stellate cells activation and potentiates anti-cancer activity of Sorafenib in hepatocellular cancer cells.J Cell Physiol. 2018 Feb;233(2):1202-1212. doi: 10.1002/jcp.25987. Epub 2017 Jul 11. J Cell Physiol. 2018. PMID: 28471474
-
MiR-338-3p inhibits hepatocarcinoma cells and sensitizes these cells to sorafenib by targeting hypoxia-induced factor 1α.PLoS One. 2014 Dec 22;9(12):e115565. doi: 10.1371/journal.pone.0115565. eCollection 2014. PLoS One. 2014. PMID: 25531114 Free PMC article.
-
Sorafenib prolongs liver regeneration after hepatic resection in rats.J Surg Res. 2013 Oct;184(2):847-54. doi: 10.1016/j.jss.2013.04.062. Epub 2013 May 18. J Surg Res. 2013. PMID: 23726434
-
Hepatocellular carcinoma.Wien Med Wochenschr. 2014 Nov;164(21-22):450-5. doi: 10.1007/s10354-014-0296-7. Epub 2014 Sep 3. Wien Med Wochenschr. 2014. PMID: 25182146 Review.
-
A short update on cancer chemoresistance.Wien Med Wochenschr. 2014 Nov;164(21-22):456-60. doi: 10.1007/s10354-014-0311-z. Epub 2014 Sep 24. Wien Med Wochenschr. 2014. PMID: 25249024 Review.
Cited by
-
Incorporation of alpha-fetoprotein(AFP) into subclassification of BCLC C stage hepatocellular carcinoma according to a 5-year survival analysis based on the SEER database.Oncotarget. 2016 Dec 6;7(49):81389-81401. doi: 10.18632/oncotarget.13232. Oncotarget. 2016. PMID: 27835609 Free PMC article.
-
Insights into the Role and Interdependence of Oxidative Stress and Inflammation in Liver Diseases.Oxid Med Cell Longev. 2016;2016:4234061. doi: 10.1155/2016/4234061. Epub 2016 Dec 14. Oxid Med Cell Longev. 2016. PMID: 28070230 Free PMC article. Review.
-
Sorafenib and Mesenchymal Stem Cell Therapy: A Promising Approach for Treatment of HCC.Evid Based Complement Alternat Med. 2020 Jun 14;2020:9602728. doi: 10.1155/2020/9602728. eCollection 2020. Evid Based Complement Alternat Med. 2020. PMID: 32617114 Free PMC article.
-
PDGF signaling pathway in hepatic fibrosis pathogenesis and therapeutics (Review).Mol Med Rep. 2017 Dec;16(6):7879-7889. doi: 10.3892/mmr.2017.7641. Epub 2017 Sep 27. Mol Med Rep. 2017. PMID: 28983598 Free PMC article. Review.
-
Elucidating tissue specific genes using the Benford distribution.BMC Genomics. 2016 Aug 9;17:595. doi: 10.1186/s12864-016-2921-x. BMC Genomics. 2016. PMID: 27506195 Free PMC article.
References
-
- Berasain C, Castillo J, Perugorria MJ, Latasa MU, Prieto J, Avila MA. Inflammation and Liver Cancer: New Molecular Links. Ann N Y Acad Sci. 2009;1155:206–221. - PubMed
-
- Marrero JA. Multidisciplinary management of hepatocellular carcinoma: where are we today? Semin Liver Dis. 2013;33:S3–10. - PubMed
-
- Schwartz M, Roayaie S, Konstadoulakis M. Strategies for the management of hepatocellular carcinoma. Nat Clin Pract Oncol. 2007;4:424–432. - PubMed
-
- Livraghi T, Mäkisalo H, Line P-D. Treatment options in hepatocellular carcinoma today. Scand J Surg SJS Off Organ Finn Surg Soc Scand Surg Soc. 2011;100:22–29. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials

