Comparison of the Disposable Streamlined Liner of the Pharynx Airway and the Disposable I-gel in Anaesthetized, Paralyzed Adults: A Randomized Prospective Study
- PMID: 26697064
- PMCID: PMC4678238
- DOI: 10.1155/2015/971059
Comparison of the Disposable Streamlined Liner of the Pharynx Airway and the Disposable I-gel in Anaesthetized, Paralyzed Adults: A Randomized Prospective Study
Abstract
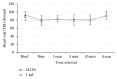
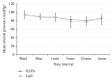
Introduction. This study compared streamlined liner of the pharynx airway (SLIPA) and I-gel noninflatable, single-use, supraglottic airway device (SAD) performance in anesthetized, paralyzed adults. Methods. Eighty adults (ASA physical statuses I-III) who were undergoing elective procedures under general anesthesia with an SAD were enrolled in this prospective, randomized, single-blind study. Subjects were randomly and evenly assigned to the SLIPA or I-gel group for intraoperative airway management. Ease and number of insertions, insertion time, oropharyngeal sealing pressure, hemodynamic response, oxygen saturation (SpO2), end-tidal CO2 (EtCO2), and peri- and postoperative complications were examined. Results. The SLIPA and I-gel devices were successfully inserted in 100% and 95% of subjects, respectively. In two I-gel subjects (5%), ventilation was not possible after two attempts, but a size 55 SLIPA was successfully inserted in both cases. Forty-two and 38 patients were ultimately included in the SLIPA and I-gel groups, respectively. Insertion time was significantly shorter with the SLIPA (11.19 ± 3.03 s) than with the I-gel (15.05 ± 6.37 s, P = 0.003). Oropharyngeal sealing pressure was significantly higher in SLIPA (28.76 ± 3.11 cmH2O) than in I-gel (25.9 ± 3.65 cmH2O) subjects (P = 0.001). Blood staining occurred more frequently in SLIPA (n = 8, 19.0%) than in I-gel (n = 5, 13.2%) patients (P < 0.01). Heart rate, mean arterial blood pressure, SpO2, and EtCO2 were not significantly different between groups. Conclusion. Although blood staining incidence was higher, SLIPA insertion was easier and faster than I-gel insertion. The SLIPA provided better airway sealing pressure. Both devices had similar mechanical ventilation and oxygenation characteristics and comparable hemodynamic stability. Both noninflatable SADs are useful, but SLIPA rapid insertion and good airway sealing make it an effective alternative to the I-gel.
Figures
Similar articles
-
Comparison of the third-generation streamlined liner of the pharynx airway (SLIPA-3G) with the laryngeal mask airway supreme for laparoscopic cholecystectomy: a randomized prospective study.BMC Anesthesiol. 2022 Apr 5;22(1):97. doi: 10.1186/s12871-022-01638-0. BMC Anesthesiol. 2022. PMID: 35382763 Free PMC article. Clinical Trial.
-
Comparison of streamlined liner of the pharynx airway (SLIPA™) with the laryngeal mask airway Proseal™ for lower abdominal laparoscopic surgeries in paralyzed, anesthetized patients.Saudi J Anaesth. 2011 Jul;5(3):270-6. doi: 10.4103/1658-354X.84100. Saudi J Anaesth. 2011. PMID: 21957405 Free PMC article.
-
A randomized comparison of pediatric-sized Streamlined Liner of Pharyngeal Airway and Laryngeal Mask Airway-Unique in paralyzed children.Paediatr Anaesth. 2016 May;26(5):557-63. doi: 10.1111/pan.12883. Epub 2016 Mar 24. Paediatr Anaesth. 2016. PMID: 27012370 Clinical Trial.
-
Brief review: the Cobra Perilaryngeal Airway (CobraPLA and the Streamlined Liner of Pharyngeal Airway (SLIPA) supraglottic airways.Can J Anaesth. 2008 Mar;55(3):177-85. doi: 10.1007/BF03016093. Can J Anaesth. 2008. PMID: 18310629 Review.
-
Comparison of the Laryngeal Mask Airway ProSeal and the Streamlined Liner of the Pharynx Airway During General Anesthesia: A Systematic Review and Meta-analysis.J Perianesth Nurs. 2024 Feb;39(1):48-57.e3. doi: 10.1016/j.jopan.2023.05.008. Epub 2023 Oct 11. J Perianesth Nurs. 2024. PMID: 37831044
Cited by
-
Choice of supraglottic airway devices: a network meta-analysis of randomised controlled trials.Br J Anaesth. 2024 Dec;133(6):1284-1306. doi: 10.1016/j.bja.2024.09.001. Epub 2024 Oct 15. Br J Anaesth. 2024. PMID: 39406569
References
-
- Ueki R., Komasawa N., Nishimoto K., Sugi T., Hirose M., Kaminoh Y. Utility of the Aintree Intubation Catheter in fiberoptic tracheal intubation through the three types of intubating supraglottic airways: a manikin simulation study. Journal of Anesthesia. 2014;28(3):363–367. doi: 10.1007/s00540-013-1724-3. - DOI - PMC - PubMed
-
- Gruber C., Nabecker S., Wohlfarth P., et al. Evaluation of airway management associated hands-off time during cardiopulmonary resuscitation: a randomised manikin follow-up study. Scandinavian Journal of Trauma, Resuscitation and Emergency Medicine. 2013;21, article 10 doi: 10.1186/1757-7241-21-10. - DOI - PMC - PubMed
-
- Sardi A. S., Britto M., Rangel J. Comparison of postoperative throat and neck complaints after the use of the i-gel versus the traditional laryngeal mask. Open Journal of Anesthesiology. 2013;3(4):233–236. doi: 10.4236/ojanes.2013.34053. - DOI
LinkOut - more resources
Full Text Sources
Other Literature Sources

