Effect of P144® (Anti-TGF-β) in an "In Vivo" Human Hypertrophic Scar Model in Nude Mice
- PMID: 26720517
- PMCID: PMC4697841
- DOI: 10.1371/journal.pone.0144489
Effect of P144® (Anti-TGF-β) in an "In Vivo" Human Hypertrophic Scar Model in Nude Mice
Abstract
Background: Hypertrophic scars are one of the most important complications in surgery due to their cosmetic and functional impairments. Previous studies in tissue fibrotic disorders have shown promising results by inhibiting the biological activity effect of Transforming Growth Factor-beta 1 (TGF-β1). The aim of the current study was to determine the clinical effect of the inhibition of TGF-β1 signaling in human hypertrophic scars implanted in nude mice by topical application of an inhibitor of TGF-β1 (P144®).
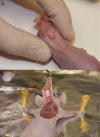
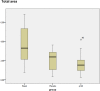
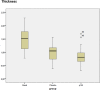
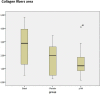
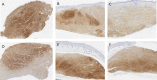
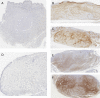
Material and methods: A total of 30 human hypertrophic scars were implanted in 60 nude mice. The animals were divided in two groups, group A (placebo) and group B (treatment). Group C (basal) was considered as the preimplanted scar samples and they were not implanted in the nude mice. After the shedding period, topical application of a lipogel containing placebo (group A) or P144 (group B) was daily administered during two weeks. The animals were sacrificed upon completion of the study. Total area, thickness and collagen fibers area were measure and compared across all groups. Immunohistochemistry was also performed in order to quantify collagen type I and type III and elastic fiber expressions present in the dermis.
Results: Successful shedding was achieved in 83,3% of the xenografts. The mean time for shedding was 35±5.4 days. Statistically significant differences were found in the total area, collagen fibers area and thickness between the groups. Increased elastic fibers and decreased collagen I were found in the P144-treated group compared to the basal group.
Conclusion: Topical application of an inhibitor of TGF-β1 may promote scar maturation and clinical improvement of hypertrophic scar morphology features in an "in vivo" model in nude mice after two weeks of treatment.
Conflict of interest statement
Figures


Similar articles
-
[Effects of transforming growth factor β1 receptor inhibitor SD-208 on human hypertrophic scar].Zhonghua Shao Shang Za Zhi. 2016 Jul 20;32(7):389-95. doi: 10.3760/cma.j.issn.1009-2587.2016.07.002. Zhonghua Shao Shang Za Zhi. 2016. PMID: 27464628 Chinese.
-
[Effect of Col I A1 antisense oligodeoxynucleotide on collagen synthesis in human hypertrophic scar transplanted nude mouse model].Zhongguo Xiu Fu Chong Jian Wai Ke Za Zhi. 2011 Jun;25(6):718-23. Zhongguo Xiu Fu Chong Jian Wai Ke Za Zhi. 2011. PMID: 21735787 Chinese.
-
[Experimental study on BMSCs transfected by endogene inhibiting hypertrophic scar].Zhongguo Xiu Fu Chong Jian Wai Ke Za Zhi. 2008 Feb;22(2):212-6. Zhongguo Xiu Fu Chong Jian Wai Ke Za Zhi. 2008. PMID: 18365621 Chinese.
-
Topical application of a peptide inhibitor of transforming growth factor-beta1 ameliorates bleomycin-induced skin fibrosis.J Invest Dermatol. 2005 Sep;125(3):450-5. doi: 10.1111/j.0022-202X.2005.23859.x. J Invest Dermatol. 2005. PMID: 16117784
-
Emerging evidence for the roles of peptide in hypertrophic scar.Life Sci. 2020 Jan 15;241:117174. doi: 10.1016/j.lfs.2019.117174. Epub 2019 Dec 13. Life Sci. 2020. PMID: 31843531 Review.
Cited by
-
A Systematic Review Comparing Animal and Human Scarring Models.Front Surg. 2022 Apr 22;9:711094. doi: 10.3389/fsurg.2022.711094. eCollection 2022. Front Surg. 2022. PMID: 35529910 Free PMC article. Review.
-
OMICS Approaches Evaluating Keloid and Hypertrophic Scars.Int J Inflam. 2022 Oct 27;2022:1490492. doi: 10.1155/2022/1490492. eCollection 2022. Int J Inflam. 2022. PMID: 36483731 Free PMC article. Review.
-
TGF-β signaling in health, disease, and therapeutics.Signal Transduct Target Ther. 2024 Mar 22;9(1):61. doi: 10.1038/s41392-024-01764-w. Signal Transduct Target Ther. 2024. PMID: 38514615 Free PMC article. Review.
-
TGF-β1 peptide-based inhibitor P144 ameliorates renal fibrosis after ischemia-reperfusion injury by modulating alternatively activated macrophages.Cell Prolif. 2022 Oct;55(10):e13299. doi: 10.1111/cpr.13299. Epub 2022 Jun 28. Cell Prolif. 2022. PMID: 35762283 Free PMC article.
-
[Effect of tranilast on wound healing and administration time on scar hyperplasia of deep partial-thickness burn in mice].Zhongguo Xiu Fu Chong Jian Wai Ke Za Zhi. 2017 Apr 15;31(4):465-472. doi: 10.7507/1002-1892.201611033. Zhongguo Xiu Fu Chong Jian Wai Ke Za Zhi. 2017. PMID: 29798614 Free PMC article. Chinese.
References
-
- Peacock EE, Madden JW, Trier WC. Biologic basis for the treatment of keloids and hypertrophic scars. South Med J. 1970; 63: 755–60. - PubMed
-
- Vande Berg JS, Rudolph R. Cultured myofibroblasts: a useful model to study wound contraction and pathological contracture. Ann Plast Surg. 1985; 14: 111–20. - PubMed
-
- Brissett AE, Sherris DA. Scar contractures, hypertrophic scars, and keloids. Facial Plast Surg. 2001; 17: 263–72. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources

