Esophagogastric junction contractile integral (EGJ-CI) quantifies changes in EGJ barrier function with surgical intervention
- PMID: 26768087
- PMCID: PMC4842118
- DOI: 10.1111/nmo.12757
Esophagogastric junction contractile integral (EGJ-CI) quantifies changes in EGJ barrier function with surgical intervention
Abstract
Background: Esophagogastric junction contractile integral (EGJ-CI) assesses EGJ barrier function on esophageal high resolution manometry (HRM). We assessed EGJ-CI values in achalasia and gastroesophageal reflux disease (GERD) to determine if postoperative EGJ-CI changes reflected surgical intervention.
Methods: Twenty-one achalasia patients (42.8 ± 3.2 years, 62% F) with HRM before and after Heller myotomy (HM) and 68 GERD patients (53.9 ± 1.8 years, 66% F) undergoing antireflux surgery (ARS) were compared to 21 healthy controls (27.6 ± 0.6 years, 52% F). Esophagogastric junction contractile integral (mmHg.cm) was calculated using the distal contractile integral measurement across the EGJ, measured above the gastric baseline and corrected for respiration. Pre and postsurgical EGJ-CI and conventional lower esophageal sphincter pressure (LESP) metrics were compared within and between these groups using non-parametric tests. Correlation between EGJ-CI and conventional LESP metrics was assessed.
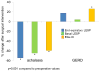
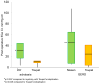
Key results: Baseline EGJ-CI was higher in achalasia compared to GERD (p < 0.001) or controls (p = 0.03). Esophagogastric junction contractile integral declined by 59.2% after HM in achalasia (p = 0.001), and increased by 26.3% after ARS in GERD (p = 0.005). End-expiratory and basal LESP decreased by 74.5% and 64.5% with HM, but increased by only 17.8% and 4.3% with ARS. Differences were noted between Dor vs Toupet fundoplication in achalasia (p = 0.007), and partial vs complete ARS in GERD (p = 0.03). Esophagogastric junction contractile integral correlated modestly with both end-expiratory and basal LESP (Pearson's r of 0.8 for all), but was less robust in GERD (0.7).
Conclusions & inferences: Esophagogastric junction contractile integral has clinical utility in assessing EGJ barrier function at baseline and after surgical intervention to the EGJ, and could complement conventional EGJ metrics.
Keywords: antireflux surgery; esophagogastric junction; high-resolution manometry; myotomy.
© 2016 John Wiley & Sons Ltd.
Conflict of interest statement
No conflicts of interest exist. No writing assistance was obtained.
Figures





Similar articles
-
The Utility of Esophageal Motility Testing in Gastroesophageal Reflux Disease (GERD).Curr Gastroenterol Rep. 2019 Jul 10;21(8):37. doi: 10.1007/s11894-019-0704-7. Curr Gastroenterol Rep. 2019. PMID: 31289922 Review.
-
Assessment of the esophagogastric junction (EGJ) using the EGJ contractile integral (EGJ-CI) following per-oral endoscopic myotomy (POEM) in achalasia.Rev Esp Enferm Dig. 2018 Nov;110(11):706-711. doi: 10.17235/reed.2018.5560/2018. Rev Esp Enferm Dig. 2018. PMID: 30032628
-
Esophagogastric junction contractile integral and morphology: Two high-resolution manometry metrics of the anti-reflux barrier.J Gastroenterol Hepatol. 2017 Aug;32(8):1443-1449. doi: 10.1111/jgh.13720. J Gastroenterol Hepatol. 2017. PMID: 28061013
-
Novel 3D high-resolution manometry metrics for quantifying esophagogastric junction contractility.Neurogastroenterol Motil. 2017 Aug;29(8):10.1111/nmo.13054. doi: 10.1111/nmo.13054. Epub 2017 Apr 5. Neurogastroenterol Motil. 2017. PMID: 28378424 Free PMC article.
-
Laparoscopic Heller Myotomy: A Fundoplication Is Necessary to Control Gastroesophageal Reflux.J Laparoendosc Adv Surg Tech A. 2019 Jun;29(6):721-725. doi: 10.1089/lap.2019.0155. Epub 2019 Apr 19. J Laparoendosc Adv Surg Tech A. 2019. PMID: 31009312 Review.
Cited by
-
The Esophageal Manometry with Gas-perfused Catheters.Open Med (Wars). 2018 Jun 14;13:232-236. doi: 10.1515/med-2018-0036. eCollection 2018. Open Med (Wars). 2018. PMID: 29915812 Free PMC article.
-
High-resolution esophageal manometry: interpretation in clinical practice.Curr Opin Gastroenterol. 2017 Jul;33(4):301-309. doi: 10.1097/MOG.0000000000000369. Curr Opin Gastroenterol. 2017. PMID: 28426462 Free PMC article. Review.
-
Esophageal motor abnormalities in gastroesophageal reflux disorders.Tzu Chi Med J. 2024 Mar 26;36(2):120-126. doi: 10.4103/tcmj.tcmj_209_23. eCollection 2024 Apr-Jun. Tzu Chi Med J. 2024. PMID: 38645779 Free PMC article. Review.
-
The Utility of Esophageal Motility Testing in Gastroesophageal Reflux Disease (GERD).Curr Gastroenterol Rep. 2019 Jul 10;21(8):37. doi: 10.1007/s11894-019-0704-7. Curr Gastroenterol Rep. 2019. PMID: 31289922 Review.
-
Current Advancement on the Dynamic Mechanism of Gastroesophageal Reflux Disease.Int J Biol Sci. 2021 Oct 3;17(15):4154-4164. doi: 10.7150/ijbs.65066. eCollection 2021. Int J Biol Sci. 2021. PMID: 34803489 Free PMC article. Review.
References
-
- Gyawali CP, Patel A. Esophageal Motor Function: Technical Aspects of Manometry. Gastrointest Endosc Clin N Am. 2014 - PubMed
-
- Bredenoord AJ, Weusten BL, Timmer R, et al. Intermittent spatial separation of diaphragm and lower esophageal sphincter favors acidic and weakly acidic reflux. Gastroenterology. 2006;130:334–40. - PubMed
-
- Shaker R, Dodds WJ, Kahrilas PJ, et al. Relationship of intraluminal pH and pressure within the lower esophageal sphincter. Am J Gastroenterol. 1991;86:812–6. - PubMed
-
- Chan WW, Haroian LR, Gyawali CP. Value of preoperative esophageal function studies before laparoscopic antireflux surgery. Surg Endosc. 2011;25:2943–9. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

