Molecular Genetic Analysis of Ovarian Brenner Tumors and Associated Mucinous Epithelial Neoplasms: High Variant Concordance and Identification of Mutually Exclusive RAS Driver Mutations and MYC Amplification
- PMID: 26797085
- PMCID: PMC5903309
- DOI: 10.1016/j.ajpath.2015.11.008
Molecular Genetic Analysis of Ovarian Brenner Tumors and Associated Mucinous Epithelial Neoplasms: High Variant Concordance and Identification of Mutually Exclusive RAS Driver Mutations and MYC Amplification
Abstract
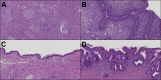
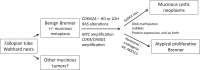
Benign ovarian Brenner tumors often are associated with mucinous cystic neoplasms, which are hypothesized to share a histogenic origin and progression, however, supporting molecular characterization is limited. Our goal was to identify molecular mechanisms linking these tumors. DNA from six Brenner tumors with paired mucinous tumors, two Brenner tumors not associated with a mucinous neoplasm, and two atypical proliferative (borderline) Brenner tumors was extracted from formalin-fixed, paraffin-embedded tumor samples and sequenced using a 358-gene next-generation sequencing assay. Variant calls were compared within tumor groups to assess somatic mutation profiles. There was high concordance of the variants between paired samples (40% to 75%; P < 0.0001). Four of the six tumor pairs showed KRAS hotspot driver mutations specifically in the mucinous tumor. In the two paired samples that lacked KRAS mutations, MYC amplification was detected in both of the mucinous and the Brenner components; MYC amplification also was detected in a third Brenner tumor. Five of the Brenner tumors had no reportable potential driver alterations. The two atypical proliferative (borderline) Brenner tumors both had RAS mutations. The high degree of coordinate variants between paired Brenner and mucinous tumors supports a shared origin or progression. Differences observed in affected genes and pathways, particularly involving RAS and MYC, may point to molecular drivers of a divergent phenotype and progression of these tumors.
Copyright © 2016 American Society for Investigative Pathology. Published by Elsevier Inc. All rights reserved.
Figures

References
-
- Kondi-Pafiti A., Kairi-Vassilatou E., Iavazzo C.H., Vouza E., Mavrigiannaki P., Kleanthis C.H., Vlahodimitropoulos D., Liapis A. Clinicopathological features and immunoprofile of 30 cases of Brenner ovarian tumors. Arch Gynecol Obstet. 2012;285:1699–1702. - PubMed
-
- Gilks C.B., Carinelli S.G., Liu A., Prat J., Seidman J.D., Soslow R. Brenner tumors. In: Kurman R.J., Carcangiu M.L., Herrington C.S., Young R.H., editors. WHO Classification of Tumours of Female Reproductive Organs. IARC; Lyon: 2014. pp. 35–37.
-
- Kuhn E., Ayhan A., Shih IeM., Seidman J.D., Kurman R.J. Ovarian Brenner tumour: a morphologic and immunohistochemical analysis suggesting an origin from fallopian tube epithelium. Eur J Cancer. 2013;49:3839–3849. - PubMed
-
- Seidman J.D., Khedmati F. Exploring the histogenesis of ovarian mucinous and transitional cell (Brenner) neoplasms and their relationship with Walthard cell nests: a study of 120 tumors. Arch Pathol Lab Med. 2008;132:1753–1760. - PubMed
-
- Roma A.A., Masand R.P. Different staining patterns of ovarian Brenner tumor and the associated mucinous tumor. Ann Diagn Pathol. 2015;19:29–32. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

