Management of Neuropsychiatric Systemic Lupus Erythematosus: Current Approaches and Future Perspectives
- PMID: 26809245
- PMCID: PMC4791452
- DOI: 10.1007/s40265-015-0534-3
Management of Neuropsychiatric Systemic Lupus Erythematosus: Current Approaches and Future Perspectives
Abstract
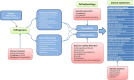
Neuropsychiatric systemic lupus erythematosus (NPSLE) is a generic definition referring to a series of neurological and psychiatric symptoms directly related to systemic lupus erythematosus (SLE). NPSLE includes heterogeneous and rare neuropsychiatric (NP) manifestations involving both the central and peripheral nervous system. Due to the lack of a gold standard, the attribution of NP symptoms to SLE represents a clinical challenge that obligates the strict exclusion of any other potential cause. In the acute setting, management of these patients does not differ from other non-SLE subjects presenting with the same NP manifestation. Afterwards, an individualized therapeutic strategy, depending on the presenting manifestation and severity of symptoms, must be started. Clinical trials in NPSLE are scarce and most of the data are extracted from case series and case reports. High-dose glucocorticoids and intravenous cyclophosphamide remain the cornerstone for patients with severe symptoms that are thought to reflect inflammation or an underlying autoimmune process. Rituximab, intravenous immunoglobulins, or plasmapheresis may be used if response is not achieved. When patients present with mild to moderate NP manifestations, or when maintenance therapy is warranted, azathioprine and mycophenolate may be considered. When symptoms are thought to reflect a thrombotic underlying process, anticoagulation and antiplatelet agents are the mainstay of therapy, especially if antiphospholipid antibodies or antiphospholipid syndrome are present. Recent trials on SLE using new biologicals, based on newly understood SLE mechanisms, have shown promising results. Based on what we currently know about its pathogenesis, it is tempting to speculate how these new therapies may affect the management of NPSLE patients. This article provides a comprehensive and critical review of the literature on the epidemiology, pathophysiology, diagnosis, and management of NPSLE. We describe the most common pharmacological treatments used in NPSLE, based on both a literature search and our expert opinion. The extent to which new drugs in the advanced development of SLE, or the blockade of new targets, may impact future treatment of NPSLE will also be discussed.
Figures
References
-
- Tsokos GC. Systemic lupus erythematosus. N Engl J Med. 2011;365(22):2110–2121. - PubMed
-
- Jeltsch-David H, Muller S. Neuropsychiatric systemic lupus erythematosus: pathogenesis and biomarkers. Nat Rev Neurol. 2014;10(10):579–596. - PubMed
-
- Zirkzee EJ, Steup-Beekman GM, van der Mast RC, Bollen EL, van der Wee NJ, Baptist E, et al. Prospective study of clinical phenotypes in neuropsychiatric systemic lupus erythematosus; multidisciplinary approach to diagnosis and therapy. J Rheumatol. 2012;39(11):2118–2126. - PubMed
-
- Amur S, Parekh A, Mummaneni P. Sex differences and genomics in autoimmune diseases. J Autoimmun. 2012;38(2–3):J254–J265. - PubMed
-
- Miller MH, Urowitz MB, Gladman DD, Killinger DW. Systemic lupus erythematosus in males. Medicine (Baltimore). 1983;62(5):327–334. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Molecular Biology Databases
Miscellaneous