Definitions, End Points, and Clinical Trial Designs for Non-Muscle-Invasive Bladder Cancer: Recommendations From the International Bladder Cancer Group
- PMID: 26811532
- PMCID: PMC5321095
- DOI: 10.1200/JCO.2015.64.4070
Definitions, End Points, and Clinical Trial Designs for Non-Muscle-Invasive Bladder Cancer: Recommendations From the International Bladder Cancer Group
Abstract
Purpose: To provide recommendations on appropriate clinical trial designs in non-muscle-invasive bladder cancer (NMIBC) based on current literature and expert consensus of the International Bladder Cancer Group.
Methods: We reviewed published trials, guidelines, meta-analyses, and reviews and provided recommendations on eligibility criteria, baseline evaluations, end points, study designs, comparators, clinically meaningful magnitude of effect, and sample size.
Results: NMIBC trials must be designed to provide the most clinically relevant data for the specific risk category of interest (low, intermediate, or high). Specific eligibility criteria and baseline evaluations depend on the risk category being studied. For the population of patients for whom bacillus Calmette-Guérin (BCG) has failed, the type of failure (BCG unresponsive, refractory, relapsing, or intolerant) should be clearly defined to make comparisons across trials feasible. Single-arm designs may be relevant for the BCG-unresponsive population. Here, a clinically meaningful initial complete response rate (for carcinoma in situ) or recurrence-free rate (for papillary tumors) of at least 50% at 6 months, 30% at 12 months, and 25% at 18 months is recommended. For other risk levels, randomized superiority trial designs are recommended; noninferiority trials are to be used sparingly given the large sample size required. Placebo control is considered unethical for all intermediate- and high-risk strata; therefore, control arms should comprise the current guideline-recommended standard of care for the respective risk level. In general, trials should use time to recurrence or recurrence-free survival as the primary end point and time to progression, toxicity, disease-specific survival, and overall survival as potential secondary end points. Realistic efficacy thresholds should be set to ensure that novel therapies receive due review by regulatory bodies.
Conclusion: The International Bladder Cancer Group has developed formal recommendations regarding definitions, end points, and clinical trial designs for NMIBC to encourage uniformity among studies in this disease.
© 2016 by American Society of Clinical Oncology.
Conflict of interest statement
Authors’ disclosures of potential conflicts of interest are found in the article online at
Figures
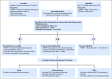
Comment in
-
Re: Definitions, End Points, and Clinical Trial Designs for Non-Muscle-Invasive Bladder Cancer: Recommendations from the International Bladder Cancer Group.J Urol. 2018 May;199(5):1111-1112. doi: 10.1016/j.juro.2018.02.035. Epub 2018 Feb 17. J Urol. 2018. PMID: 29677899 No abstract available.
References
-
- Jarow JP, Lerner SP, Kluetz PG, et al. Clinical trial design for the development of new therapies for nonmuscle-invasive bladder cancer: Report of a Food and Drug Administration and American Urological Association public workshop. Urology. 2014;83:262–264. - PubMed
-
- FDA/AUA Bladder Cancer Workshop: Clinical trial design issues: Development of new therapies for non-muscle invasive bladder cancer. https://www.auanet.org/university/live-course-wip.cfm?id=476id=476&video....
-
- Amrhein J, Kamat AM, Morales A. Re: Jarrow JP et al: Clinical trial design for the development of new therapies for non-muscle-invasive bladder cancer: Report of a Food and Drug Administration and American Urological Association public workshop (Urology 2014;83:262-265) Urology. 2014;84:494–495. - PubMed
-
- van der Meijden AP. The use of the marker tumor concept in Ta, T1 bladder cancer: is it justified? Urol Oncol. 2002;7:31–33. - PubMed
-
- McCullough LB. Ethical issues in the use of tumor markers in clinical investigation of the management of bladder cancer. Urol Oncol. 2002;7:35–37. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

