Integration of 3D Printed and Micropatterned Polycaprolactone Scaffolds for Guidance of Oriented Collagenous Tissue Formation In Vivo
- PMID: 26820240
- PMCID: PMC4805502
- DOI: 10.1002/adhm.201500758
Integration of 3D Printed and Micropatterned Polycaprolactone Scaffolds for Guidance of Oriented Collagenous Tissue Formation In Vivo
Abstract
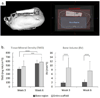
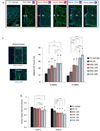
Scaffold design incorporating multiscale cues for clinically relevant, aligned tissue regeneration has potential to improve structural and functional integrity of multitissue interfaces. The objective of this preclinical study is to develop poly(ε-caprolactone) (PCL) scaffolds with mesoscale and microscale architectural cues specific to human ligament progenitor cells and assess their ability to form aligned bone-ligament-cementum complexes in vivo. PCL scaffolds are designed to integrate a 3D printed bone region with a micropatterned PCL thin film consisting of grooved pillars. The patterned film region is seeded with human ligament cells, fibroblasts transduced with bone morphogenetic protein-7 genes seeded within the bone region, and a tooth dentin segment positioned on the ligament region prior to subcutaneous implantation into a murine model. Results indicate increased tissue alignment in vivo using micropatterned PCL films, compared to random-porous PCL. At week 6, 30 μm groove depth significantly enhances oriented collagen fiber thickness, overall cell alignment, and nuclear elongation relative to 10 μm groove depth. This study demonstrates for the first time that scaffolds with combined hierarchical mesoscale and microscale features can align cells in vivo for oral tissue repair with potential for improving the regenerative response of other bone-ligament complexes.
Keywords: 3D printing; cell alignment; micropatterning; periodontal ligaments (PDL); polycaprolactone (PCL).
© 2016 WILEY-VCH Verlag GmbH & Co. KGaA, Weinheim.
Figures





Similar articles
-
Micropatterned Scaffolds with Immobilized Growth Factor Genes Regenerate Bone and Periodontal Ligament-Like Tissues.Adv Healthc Mater. 2018 Nov;7(22):e1800750. doi: 10.1002/adhm.201800750. Epub 2018 Oct 19. Adv Healthc Mater. 2018. PMID: 30338658 Free PMC article.
-
Incorporation of aligned PCL-PEG nanofibers into porous chitosan scaffolds improved the orientation of collagen fibers in regenerated periodontium.Acta Biomater. 2015 Oct;25:240-52. doi: 10.1016/j.actbio.2015.07.023. Epub 2015 Jul 15. Acta Biomater. 2015. PMID: 26188325
-
Effects of 3D-Printed Polycaprolactone/β-Tricalcium Phosphate Membranes on Guided Bone Regeneration.Int J Mol Sci. 2017 Apr 25;18(5):899. doi: 10.3390/ijms18050899. Int J Mol Sci. 2017. PMID: 28441338 Free PMC article.
-
Three-Dimensional Printed Polycaprolactone Scaffolds for Bone Regeneration Success and Future Perspective.Tissue Eng Part A. 2019 Jul;25(13-14):931-935. doi: 10.1089/ten.TEA.2019.0102. Tissue Eng Part A. 2019. PMID: 31084409 Review.
-
Biomaterial-Based Approaches for Regeneration of Periodontal Ligament and Cementum Using 3D Platforms.Int J Mol Sci. 2019 Sep 5;20(18):4364. doi: 10.3390/ijms20184364. Int J Mol Sci. 2019. PMID: 31491973 Free PMC article. Review.
Cited by
-
Role of three-dimensional printing in periodontal regeneration and repair: Literature review.J Indian Soc Periodontol. 2019 Nov-Dec;23(6):504-510. doi: 10.4103/jisp.jisp_46_19. J Indian Soc Periodontol. 2019. PMID: 31849394 Free PMC article. Review.
-
Polyphenol-mediated redox-active hydrogel with H2S gaseous-bioelectric coupling for periodontal bone healing in diabetes.Nat Commun. 2024 Oct 21;15(1):9071. doi: 10.1038/s41467-024-53290-6. Nat Commun. 2024. PMID: 39433776 Free PMC article.
-
Main Applications and Recent Research Progresses of Additive Manufacturing in Dentistry.Biomed Res Int. 2022 Feb 24;2022:5530188. doi: 10.1155/2022/5530188. eCollection 2022. Biomed Res Int. 2022. PMID: 35252451 Free PMC article. Review.
-
Microfabrication approaches for oral research and clinical dentistry.Front Dent Med. 2023 Mar 9;4:1120394. doi: 10.3389/fdmed.2023.1120394. eCollection 2023. Front Dent Med. 2023. PMID: 39916924 Free PMC article. Review.
-
The recent advances in scaffolds for integrated periodontal regeneration.Bioact Mater. 2021 Mar 18;6(10):3328-3342. doi: 10.1016/j.bioactmat.2021.03.012. eCollection 2021 Oct. Bioact Mater. 2021. PMID: 33817414 Free PMC article. Review.
References
-
- Bettinger CJ, Langer R, Borenstein JT. Angew. Chem. Int. Ed. Engl. 2009;48:5406. - PMC - PubMed
- Hui EE, Bhatia SN. Proc. Natl. Acad. Sci. USA. 2007;104:5722. - PMC - PubMed
- Hoehme S, Brulport M, Bauer A, Bedawy E, Schormann W, Hermes M, Puppe V, Gebhardt R, Zellmer S, Schwarz M, Bockamp E, Timmel T, Hengstler JG, Drasdo D. Proc. Natl. Acad. Sci. USA. 2010;107:10371. - PMC - PubMed
-
- Eke PI, Dye BA, Wei L, Thornton-Evans GO, Genco RJ. J. Dent. Res. 2012;91:914. - PubMed
-
- Yu N, Prodanov L, te Riet J, Yang F, Walboomers XF, Jansen JA. J. Periodontol. 2013;84:1504. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

